|
Conceiving is a blessing and we don’t think beyond that when we hear the good news. Once things settle and the happiness sinks in, the couple start looking out for the best gynecologist/obstetrician to ensure a smooth pregnancy journey and to welcome their dearest bundle of joy into this world with utmost comfort and health. Parents these days are blessed in one way-they have the technology and facilities to predict a baby’s health and brain development as much as possible inside the womb but at the same time, they are also under constant pressure to take care of their health and too much of information also crumples their peace of mind. Don’t you think that ignorance is bliss sometimes in lives? Our mothers and grandmothers too delivered hale and healthy babies without much fuss and discomfort despite lacking modern hospitals and facilities to treat them as royals inside the maternity ward! While hospitals today function like five-star hotels taking care and pampering to the whims and fancies of the pregnant mum, they cannot ensure well-being and good health but only suggest practical exercise options and diet plans to help us stay healthy. Beyond that, it depends on the pregnant lady to treat her body as a holy place and work towards good health throughout her pregnancy tenure. But despite all these, there are all sorts of medical complications arising during pregnancy affecting both the mom’s and child’s health after delivery.
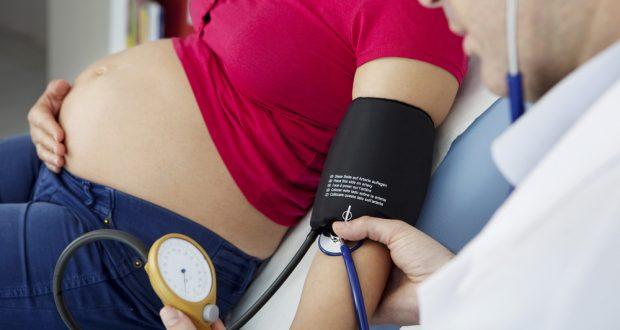
Hypertensive disorders of pregnancy (HDP) that includes gestational hypertension and pre-eclampsia affect almost 5-10% pregnancies worldwide. HDP exists as a major cause of maternal and infant mortality and morbidity everywhere. The World Health Organization (WHO) estimates that almost 4 million stillbirths and 3 million deaths occur during the first week of life every year of which 98% happen in developing countries. Such deaths often reflect the mother’s health and healthcare facilities as they are the results of events that happen in utero and during birth. Gestational Hypertension Hypertension in pregnancy (HIP) is when diastolic blood pressure is at least 90 mmHg, systolic blood pressure is at least 140 mmHg, there is a rise in diastolic blood pressure by at least 15 mmHg and rise in systolic blood pressure by 30 mmHg in a pregnant woman on at least two different occasions at least 6 hours apart. There are various studies showing that hypertension paves ways for a number of maternal and fetal complications. High blood pressure levels lead to maternal complications, affect different organs and these women are at an increased risk of post-pregnancy cardiometabolic disease. Infants born to such mothers with HPD also have high blood pressure and body mass index (BMI) in comparison to those infants born to mothers with normal blood pressure levels. Such children grow up with vagaries through young adulthood which can even lay the foundation for type 2 diabetes and stroke in life. We have animal models suggesting that reduced uterine perfusion and exposure to anti-angiogenic factors during pregnancy can increase long-term blood pressure in the offspring. Studies indicating cardiovascular disease risk as adults has been universally proven and large offspring size at birth and risk of cardio metabolic diseases in the offspring too is positive but we don’t have human studies linking hypertension in adults to increased risk of hypertension in offspring. The study below finds an association between exposure to maternal HPD and offspring hypertension and cardiometabolic risk factor at age 40 years. Population-based Cohort Study Data on first-born individuals who were born between 1955 and 1972 attending the Västerbotten Health Survey was collected and this included 14,947 participants. All the residents of the county of Västerbotten were invited of which 60% of those eligible attended. All of them were provided with a self-administered questionnaire containing queries on lifestyle such as previous diagnosis of hypertension, smoking habits and family history of cardiovascular disease. Body weight and height measurements were noted down and BMI readings were calculated. Every participant was measured of his/her systolic blood pressure (SBP) and diastolic blood pressure (DBP) in supine position before August 2009 and twice again in a seated position. A 75 g 2-hour oral glucose tolerance test (OGTT) and total serum cholesterol measurements were taken. Of the total number of participants 383 participants (2.8%) were exposed to maternal HDP. Around the age of 40 there was not much of a difference in smoking status or education level between participants exposed and not exposed to maternal HDP. Three different models were used to investigate association between maternal HDP and offspring relative risk of hypertension at age 40 years. Poisson regression models incrementally adjusted for co-variables were used. While Model I included maternal HDP in index pregnancy, Model II (this is the main model) included infant’s sex, family history of cardiovascular disease and maternal diabetes during pregnancy. Model III included education level, smoking and BMI at age 40 years. Those participants who were affected with HDP had a higher risk of hypertension in all three models-model I, Model II and Model III. Maternal HDP was also linked to higher mean BMI, SBP, DBP and 2-hour OGTT result in Model II. This study was the first to show that infants whose mothers suffered from HDP during pregnancy has an increased risk of hypertension. Also, maternal HDP puts the adult at an increased risk of higher blood pressure and BMI. Children born to mothers with pregnancies complicated by HDP mostly suffer from higher blood pressure, increased risk of hypertension and higher BMI compared to those kids born to mothers without any HDP risks. Hypertensive Disorders Elevate Risk of Hypertension after Delivery Hypertensive disorders are associated with long-term risk of cardiovascular disease but we don’t know much about the effect of it on the woman after delivery. We have study results showing that those women who develop hypertension during pregnancy are affected by elevated blood pressure in the first year after delivery. The study was on 5,960 women of whom those with pre-pregnancy high blood pressure were excluded from the analysis. Results showed that women with hypertensive disorder during pregnancy were 2.4 times likelier to develop pre-hypertension or hypertension in the ensuing year after delivery compared to those women with normal blood pressure during the pregnancy tenure. It was also seen that in comparison to women with normal blood pressure during pregnancy women with pregnancy-related hypertension were slightly younger and overweight/obese before pregnancy. This surely indicates that women who suffer from hypertension during pregnancy should keep monitoring their blood pressure with a physician after delivery to ensure that BP levels are kept under control. This helps in preventing major cardiovascular risks and complications that might arise in the future. There are evidences suggesting that the immediate few years after delivery are crucial as there is even a fivefold increase in hypertension rate in the first five years after a pre-eclamptic pregnancy. It is possible that 25-45% women with a hypertensive disorder develop hypertension within five years of delivery. So, it is critical that women start taking care of their health even before pregnancy. Every lady in her reproductive years is advised to stay on a healthy weight and lead a healthy lifestyle to prepare herself for the pregnancy that would come her way in a few years’ time. Failing to do so not only increases the complications of pregnancy but also puts the life of both the pregnant woman and her infant at a higher risk of pregnancy-related complications. References Maternal Hypertensive Disorders of Pregnancy & Offspring Risk of Hypertension: https://academic.oup.com/ajh/article/32/4/331/5205123 Hypertensive Disorders during Pregnancy Increase Risk of High Blood Pressure After Delivery: https://www.sciencedaily.com/releases/2016/01/160129090124.htm Risk of Post-pregnancy Hypertension in Women with a History of Hypertensive Disorders of Pregnancy: https://www.bmj.com/content/358/bmj.j3078 Comments are closed.
|
AVOID FRAUD. EAT SMART+91 7846 800 800
|
- Home
- Written Testimonials
- Consult
- Clinics
- Blogs
-
Diet & Nutrition
- Diabetes Reversal
- IVF IUI not needed for PCOS PCOD Infertility
-
Medical Nutrition
>
-
Disease & Conditions
>
- Infertility | PCOS
- Diabetes Mellitus
- Cholesterol
- Hypothyroid
- Kidney Problems
- Hypertension
- Cardiovascular Diseases
- Liver Diseases
- Gastro intestinal disorder
- Cancer
- Metabolic Disorders
- Orthopedic Disorders
- Eating Disorders
- Dietary Recall
- Weight Record Filled By Clients
- Online Payment Transaction Details
- Online Clients Weight Check Form
- Our Program Package Service Charges
- Weight Record 2017 Clients
- Measurements sent by Clients
- Terms & Conditions Of Payment
- Thanks. Your Form is Submitted
- Video Testimonials
- Lifestyle & Wellness
- Lifestyle & Wellness Blog
- Allergy & Intolerance
- Weight Loss / Gain
- Weight Loss / Slimming Blog
-
Disease & Conditions
>
- Life Cycle Nutrition >
- Sports Nutrition >
- Integrity in Nutrition
- Knowledge Centre
© COPYRIGHT 2022. ALL RIGHTS RESERVED. FRST HEALTHCARE PVT LTD.
Dr. Nafeesa Imteyaz of First Eat Right clinic, is the Best Dietitian Nutritionist in Bangalore. Best Dietitian Nutritionist in Pune. Best Dietitian Nutritionist in Hyderabad. Best Dietitian Nutritionist in Chennai. Best Dietitian Nutritionist in Mumbai. Best Dietitian Nutritionist in Delhi. Best Dietitian Nutritionist in Kolkata.