|
“Let food be thy medicine” these are golden words which reward you in the best of ways possible. Crops and harvests are covered by pesticides and produce quality is diminishing every day. Even if we consume the same portion of fruits and vegetables like our ancestors we are not assured of a healthier body and a stronger mind. Real agony is that we have all have forgotten to eat more of produce and have shown a greater inclination towards eating processed foods thereby stooping to even lower energy and health levels comparatively. Even toddlers and infants know what’s a burger or a French Fries, they choose their own favorite pasta or roll at restaurants and don’t prefer anything mild! It has become a difficult affair to please kids with their lunch nor it is easy to make adults eat a well-balanced meal that’s high in nutrients and energy. Apart from all this, the fast-paced world does not have time for preparing nutritious meals, going for a walk daily or reducing intake of outside foods-Isn’t food our way of celebrating team efforts, target achievements or a way of meeting and greeting friends/colleagues? Such intake of poor diet exists as the leading case of premature death and disability in many countries of the world. This is also the culprit behind metabolic syndrome and other diseases such as heart disease and diabetes which are ruling the world affecting as many people as possible.
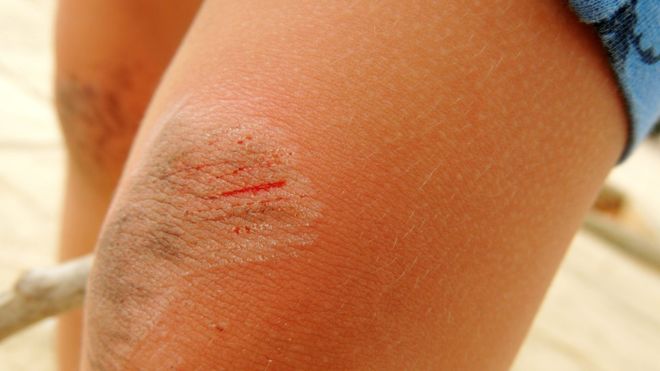
Chronic diseases ruin the quality of life of individuals and raise the health care cost of treating patients. We do have research and trials comforting us with the good news that consuming fruits and vegetables (FV) or whole grains (WG) have potential effects on the markers of metabolic syndrome. Metabolic syndrome is the cluster of conditions such as dyslipidemia, high blood pressure, impaired glucose tolerance and abdominal fat accumulation that’s linked to increased risk of cardiovascular diseases. Of late, rather than relying on medicines the trend has changed and people have accepted that treatment for BP, obesity and hypertension should focus on diets for weight loss and exercise programs that help in increasing physical activity. In the recent decades we have numerous proofs justifying the fact that consumption of fruits, vegetables, nuts, whole grains, legumes, fish and low-fat dairy products are protective and good for health. Physicians and health experts recommend consuming at least five portions of fruits and vegetables every day for our health. But what we do is to avoid every fruit/veggie that comes our way and also use every opportunity to get lost of these nutritious foods. There are some of us who don’t even eat a single portion of veggie on many days of the week or go without munching on a slice of pineapple or kiwi. Metabolic Benefits of Foods Diseases such as diabetes and cardiovascular disease have robbed people of their health and the underlying mechanism for such diseases is chronic low-grade inflammation. The gut microbiota has been in the limelight for quite sometime now as we do have numerous researches showing that the quality of the gut microbiota can prevent or lead to various diseases. The immune system and the gut microbiota interact with each other and any changes in the gut microbiota can contribute to chronic inflammation. The composition of the gut changes through the lifetime of an individual affected by the diet we eat, stress and other environmental factors. One way in which the gut microbiota induces an anti-inflammatory effect is by the production of short chain fatty acids (SCFA) that also decrease the risk of cancer and obesity. Inflammation in the body is both good and bad depending on the extent. You cut your finger or get hurt and the area around the affected part swells immediately. This means that your immune system is pretty good and the immune cells are doing their job releasing inflammatory compounds that kill bacteria and prevent the spread of infection. But sometimes, low-grade inflammation that persists over time are the root cause behind chronic diseases. The immune cells are the ones fighting here too but rather than attacking the enemy they attack the body including blood vessels and organs. This might be the work of stress, obesity or diet and if diet is the culprit we can make commendable improvements here by making strategic alterations to the diet. A diet rich in white flour, fried foods and sugar while being low in fruits and vegetables is said to be bad for health. Controlling all aspects of the diet is great but cannot be termed as a practical approach here. We know that intake of whole grains and fruits and vegetables is appreciated for gut health and anti-inflammatory effect but what is effect the of each on inflammatory markers and gut microbiota composition? Study Comparing WG and FV Participants for the study were selected via flyers advertised at grocery stores based on numerous criteria that included BMI >25, no diagnosed gastrointestinal disease, no antibiotic use, <60 min/week of physical activity and low intake of fruits and vegetables. Food intake was measured using a questionnaire that included questions on serving size. A total of 49 individuals were finally selected for the study. All the participants were enrolled into one of the three groups randomly- control, WG and FV. Participants in the control group were given 3 servings/d of refined grains, those in the FV group were given 3 servings per day of fruits and vegetables that’s still below recommended levels and those in the WG group were given 3 servings/d of whole grains that was within recommended limits. All the participants visited the research lab every week during the study period and in this time they ordered their required foods from the list of foods available within each treatment group. While each of the participants were allowed to choose any combination of foods all of them had to order at least 21 and no more than 30 servings for the week . Every week when the participants visited the research lab they brought two diaries-one contained a list of all the test foods eaten during the week and another one recorded all the gastrointestinal symptoms experienced during the week. The test foods diary listed down all the foods consumed and their individual serving sizes too. The participants were given a weekly GI symptoms questionnaire that consisted of the frequency and severity of symptoms such as stomach pain, heart burn, acid reflux, hunger pains, nausea, bloating, constipation, burping, diarrhea, abnormal stools and feelings of incomplete bowel emptying. Stool and blood samples were collected at the beginning and end of the study. Results revealed that:
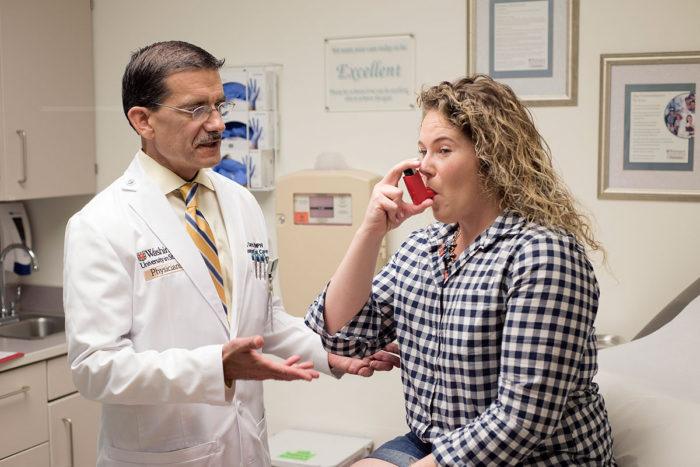
References Role of Whole Grains Versus Fruits and Vegetables in Reducing Subclinical Inflammation & Promoting Gastrointestinal Health in Individuals Affected by Overweight & Obesity: https://nutritionj.biomedcentral.com/articles/10.1186/s12937-018-0381-7  Coughing & Chest Tightness can Occur Occasionally or Frequently in All Asthma Patients Coughing & Chest Tightness can Occur Occasionally or Frequently in All Asthma Patients A simple cough makes us tired and we feel like taking the day off from school, work or even household chores. For people with asthma, they experience periods of wheezing, chest tightness, shortness of breath and coughing that might be mild or severe and might happen occasionally or even every day in life! The term ‘asthma’ is common and we all know that asthma patients carry a small tube-like device that’s called the inhaler but not many of us know what exactly causes the illness and if it can be prevented too! Asthma is a chronic, long-term condition that intermittently inflames and narrows the airways in the lungs. Its prevalence has increased tremendously in the recent decades affecting more than 300 million people worldwide and the numbers are expected to grow with yet another 100 million people affected by it by 2025. The World Health Organization (WHO) has estimated that 15 million disability-adjusted life-years (DALY) are lost and 2,50,000 deaths happen every year. It not only has social and financial burden on the affected individual but also poses a huge burden on healthcare resources. Symptoms mainly occur during the night or early in the morning disrupting sleep and above all, the quality of life of the individual is severely compromised. Anyone of any age can be a victim of this illness whose risk factors are not evident as it presents differently in both adults and children. Genes, obesity, environmental factors, allergens, infections, outdoor/indoor pollutants and tobacco smoke are some of the risk factors of asthma. The disease cannot be cured but only be managed and controlled. Treatment usually includes using controllers and relievers. Vitamin D There are increasing evidences showing that vitamin D deficiency plays an integral role in chronic diseases including asthma. Also known as the sunshine vitamin, this nutrient deficiency is increasingly witnessed among the general population in individuals as young as 10-year-old to elderly people. Would you believe if I say that half of the healthy population worldwide are vitamin D-deficient? A fat-soluble vitamin, vitamin D helps in calcium absorption, for improved bone health, is vital for immune regulation and plays an important role in respiratory infections. The increase in this nutrient deficiency is mainly due to inappropriate dietary intake, lifestyle factors, behavioral changes and insufficient exposure to sun. This vitamin is also critical for inborn and adaptive immunity that might be relevant in preventing asthma, protecting against asthma, reducing its morbidity and severity. There are many examples in which vitamin D deficiency has been associated with increased airway hyperresponsiveness (AWH), lower pulmonary function, worse asthma control and steroid resistance. The present indoor-based lifestyle and our modernized and Westernized practices keep us indoors away from the bright sun’s shining rays leading to severe vitamin D deficiency levels among any population. Though the role of vitamin D in asthma is not crystal clear we do have several cross-sectional studies that show a link between vitamin D and asthma: low levels of 25(OH)D levels in patients with mild to moderate asthma is related to poor asthma control, reduced lung function, reduced glucocorticoid response, frequent exacerbations and increased steroid use. There are also clinical trials showing the protective influence of vitamin D supplementation among asthmatic patients. Asia is a continent that mostly faces the warmth of sunshine and in South Asia most of the days are sunny. Still, vitamin D deficiency is highly prevalent in the countries here due to various factors such as improper diet, inadequate calcium levels, culture and customs that mostly keep elderly, female population and children confined within the four walls of the house preventing them from enjoying the sun’s rays or enabling them to have sufficient vitamin D levels in their body. Indians are majorly affected with almost 69% to 82% of the Indian population suffering from vitamin D deficiency. Surprisingly, it’s not only those living in the subcontinent suffering from the deficiency but also immigrants in other countries such as Denmark, UK and Norway are highly affected. Research on Vitamin D’s Relationship with Markers of Asthma Severity The study was conducted in North India with 120 participants who were aged between 18 and 80 consisting of both males and females. These individuals met the asthma criteria, did not have a history of vitamin D or calcium intake in the past one month and did not have any other respiratory and systemic disorders. All the 120 participants’ sputum eosinophil count, blood eosinophil count, serum IgE level measurements, serum 25-hydroxy vitamin D levels and spirometry tests were performed. Those individuals whose vitamin D levels were on par with requirements were taken as controls in the study. The mean age of the subjects was 30.81 ±8.97, there were 72 males (60%), 48 females (40%), 57.5% were smokers and 42.5% were non-smokers. All the patients were separated into vitamin D-sufficient and vitamin D-insufficient groups and were also grouped depending on asthma severity as intermittent, mild, moderate and severe asthmatics. Vitamin D deficiency was highly witnessed in asthma patients, there was a direct relationship between serum vitamin D levels, severity of asthma, asthma control, serum IgE levels, sputum eosinophils and lung function. The table below shows different asthma severity levels in patients who are vitamin D-sufficient and insufficient.
Serum IgE levels are linked to asthma and in this study, vitamin D-sufficient participants had lower serum IgE levels compared to the other group. IgE is an excellent determinant of allergy and the study showed that severe asthma patients had higher IgE levels compared to mild asthma. Those individuals with insufficient vitamin D had a higher mean for sputum eosinophils than those with sufficient vitamin. Higher vitamin D levels are inversely associated with IgE, sputum eosinophils and peripheral blood eosinophil counts and also decreased use of anti-inflammatory meds, reduced hospital stays and less airway hyper responsiveness. This study clearly shows that vitamin D insufficiency was highly prevalent in asthma patients and the severity of asthma also depended on the insufficiency of the vitamin. Hence, supplements could be considered for those patients with asthma.
Studies on Bronchial Asthma among Sudanese Patients The study included 86 asthmatic patients aged 18 and above diagnosed with clinical asthma. Those >70 years of age, suffering from renal, lung and liver disease and on vitamin D, calcium and anticonvulsant drugs were excluded from the study. Their asthma levels were classified from mild to severe based on the different symptoms and blood samples were taken to measure vitamin D levels. Almost 70% patients were females and all the participants had suffered from this illness for around 10 years or so. Two-thirds of the study group had normal body mass index and only one-third were overweight/obese. Those who had well-controlled asthma were 24.4%, their mean age was 40 years, had normal BMI and 12 were males, participants with partially controlled asthma were 37.2%, mean age was 37.46 years and 26 of them were females. Those with uncontrolled asthma were 38.4%, their mean age was 45.36 years and 24 of them were females. Normal Vitamin D levels were present only in 2.3% patients while the rest had insufficient or deficient vitamin D levels. 25 (OH) level in the controlled asthma group was 25.82±17.27 ng/ml, in the partially controlled group it was 17.85±7.06ng/ml and in the uncontrolled asthma group it was 16.48±7.14ng/ml. This study showed that only 47.7% individuals had vitamin D deficiency in comparison to few other studies which showed that almost 90% patients suffered from the deficiency. This might be because of the geographic location of Sudan that’s sunnier and hence, the people there are exposed to much more sunlight. This study also showed that vitamin D level had no role in asthma severity contradicting with previous study results. The Sudan study clearly shows that vitamin D level played a significant role in asthma control and aggravation of asthma but did not affect the severity of the illness in any way. Vitamin D Deficiency in Asthmatic Children The case-controlled study included 53 asthma patients and 53 controls. Children with asthma and hyperreactive airway disease were included as asthma patients. Vitamin D levels in both the groups were measured by radioimmunoassay (RIA) and was categorized as sufficient (>30 ng/ml), insufficient (20-30) and deficient (<20 ng/ml). The severity of asthma was also classified as mild, moderate and severe persistent. Both the groups had similar male gender distribution (56% vs 59%) and mean age. In the asthmatic group the mean duration of the disease was 13.1±24.6 months, 11.3% had mild asthma, 45.3% had moderate asthma and 43.4% had severe asthma. 5 of 31 kids aged below 5 years (16.1%) had high risk and 7 of 22 kids older than 5 years (31.8%) had high risk. While 73.6% asthma patients had vitamin D deficiency only 49.1% people in the control group had vitamin D deficiency, vitamin D insufficiency was 18.9% in both groups and normal vitamin D levels were 7.5% and 32.1% respectively. Observational Studies A study on 616 asthmatic kids showed that vitamin D deficiency/insufficiency was present in 28% kids and increased vitamin D levels led to decrease in asthma aggravations and also decreased the need for visits to the emergency department in hospitals. A cross-sectional study on 560 kids aged 6-14 years showed that kids with vitamin D insufficiency were 2.6 times at an increased risk of developing asthma exacerbations. Cohort studies show that lower dietary maternal intake of vitamin D result in increased asthma morbidity and wheezing rates in children. Studies in Finland and Japan on more than 750 mother-kid pairs show that dietary vitamin D intake during pregnancy was inversely linked to incidence of wheezing in kids. Clinical trials show that vitamin D offers protection against serious asthma attacks. A 6-month clinical trial showed that kids who received 500 IU/d supplementation of vitamin D had lower risk of asthma exacerbation; another trial on 100 asthmatic kids too showed the same results. But there were some other trials which did not show any association between vitamin D intake and reduction in asthma levels. Vitamin D can definitely be a supplement therapy for managing asthma. While most studies do support the use of vitamin D for keeping asthma under control there are few studies that show that vitamin D supplements either have no effect or are responsible for increased asthma attacks. References Correlation between Asthma Severity & Serum Vitamin D Levels: Experience from a Tertiary Care Centre in North India: http://www.jbiomeds.com/biomedical-sciences/correlation-between-asthma-severity-and-serum-vitamin-d-levels-experience-from-a-tertiary-care-centre-in-north-india.php?aid=23236 The Relationship between Vitamin D Level & Severity & Control of Bronchial Asthma among Adult Sudanese Patients: https://www.msjonline.org/index.php/ijrms/article/view/4784/3904 Vitamin D Deficiency and its Impact on Asthma Severity in Asthmatic Children: https://ijponline.biomedcentral.com/articles/10.1186/s13052-016-0300-5 A Review on the Role of Vitamin D in Asthma: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5491340/ Conceiving is a blessing and we don’t think beyond that when we hear the good news. Once things settle and the happiness sinks in, the couple start looking out for the best gynecologist/obstetrician to ensure a smooth pregnancy journey and to welcome their dearest bundle of joy into this world with utmost comfort and health. Parents these days are blessed in one way-they have the technology and facilities to predict a baby’s health and brain development as much as possible inside the womb but at the same time, they are also under constant pressure to take care of their health and too much of information also crumples their peace of mind. Don’t you think that ignorance is bliss sometimes in lives? Our mothers and grandmothers too delivered hale and healthy babies without much fuss and discomfort despite lacking modern hospitals and facilities to treat them as royals inside the maternity ward! While hospitals today function like five-star hotels taking care and pampering to the whims and fancies of the pregnant mum, they cannot ensure well-being and good health but only suggest practical exercise options and diet plans to help us stay healthy. Beyond that, it depends on the pregnant lady to treat her body as a holy place and work towards good health throughout her pregnancy tenure. But despite all these, there are all sorts of medical complications arising during pregnancy affecting both the mom’s and child’s health after delivery.
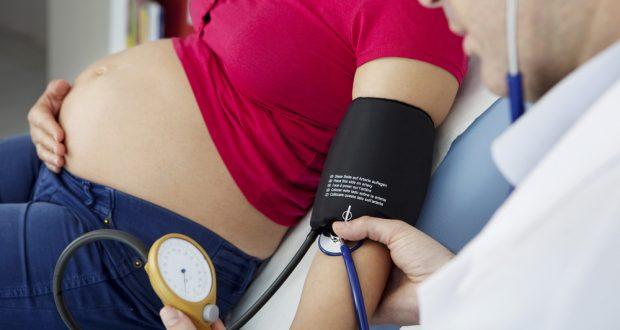
Hypertensive disorders of pregnancy (HDP) that includes gestational hypertension and pre-eclampsia affect almost 5-10% pregnancies worldwide. HDP exists as a major cause of maternal and infant mortality and morbidity everywhere. The World Health Organization (WHO) estimates that almost 4 million stillbirths and 3 million deaths occur during the first week of life every year of which 98% happen in developing countries. Such deaths often reflect the mother’s health and healthcare facilities as they are the results of events that happen in utero and during birth. Gestational Hypertension Hypertension in pregnancy (HIP) is when diastolic blood pressure is at least 90 mmHg, systolic blood pressure is at least 140 mmHg, there is a rise in diastolic blood pressure by at least 15 mmHg and rise in systolic blood pressure by 30 mmHg in a pregnant woman on at least two different occasions at least 6 hours apart. There are various studies showing that hypertension paves ways for a number of maternal and fetal complications. High blood pressure levels lead to maternal complications, affect different organs and these women are at an increased risk of post-pregnancy cardiometabolic disease. Infants born to such mothers with HPD also have high blood pressure and body mass index (BMI) in comparison to those infants born to mothers with normal blood pressure levels. Such children grow up with vagaries through young adulthood which can even lay the foundation for type 2 diabetes and stroke in life. We have animal models suggesting that reduced uterine perfusion and exposure to anti-angiogenic factors during pregnancy can increase long-term blood pressure in the offspring. Studies indicating cardiovascular disease risk as adults has been universally proven and large offspring size at birth and risk of cardio metabolic diseases in the offspring too is positive but we don’t have human studies linking hypertension in adults to increased risk of hypertension in offspring. The study below finds an association between exposure to maternal HPD and offspring hypertension and cardiometabolic risk factor at age 40 years. Population-based Cohort Study Data on first-born individuals who were born between 1955 and 1972 attending the Västerbotten Health Survey was collected and this included 14,947 participants. All the residents of the county of Västerbotten were invited of which 60% of those eligible attended. All of them were provided with a self-administered questionnaire containing queries on lifestyle such as previous diagnosis of hypertension, smoking habits and family history of cardiovascular disease. Body weight and height measurements were noted down and BMI readings were calculated. Every participant was measured of his/her systolic blood pressure (SBP) and diastolic blood pressure (DBP) in supine position before August 2009 and twice again in a seated position. A 75 g 2-hour oral glucose tolerance test (OGTT) and total serum cholesterol measurements were taken. Of the total number of participants 383 participants (2.8%) were exposed to maternal HDP. Around the age of 40 there was not much of a difference in smoking status or education level between participants exposed and not exposed to maternal HDP. Three different models were used to investigate association between maternal HDP and offspring relative risk of hypertension at age 40 years. Poisson regression models incrementally adjusted for co-variables were used. While Model I included maternal HDP in index pregnancy, Model II (this is the main model) included infant’s sex, family history of cardiovascular disease and maternal diabetes during pregnancy. Model III included education level, smoking and BMI at age 40 years. Those participants who were affected with HDP had a higher risk of hypertension in all three models-model I, Model II and Model III. Maternal HDP was also linked to higher mean BMI, SBP, DBP and 2-hour OGTT result in Model II. This study was the first to show that infants whose mothers suffered from HDP during pregnancy has an increased risk of hypertension. Also, maternal HDP puts the adult at an increased risk of higher blood pressure and BMI. Children born to mothers with pregnancies complicated by HDP mostly suffer from higher blood pressure, increased risk of hypertension and higher BMI compared to those kids born to mothers without any HDP risks. Hypertensive Disorders Elevate Risk of Hypertension after Delivery Hypertensive disorders are associated with long-term risk of cardiovascular disease but we don’t know much about the effect of it on the woman after delivery. We have study results showing that those women who develop hypertension during pregnancy are affected by elevated blood pressure in the first year after delivery. The study was on 5,960 women of whom those with pre-pregnancy high blood pressure were excluded from the analysis. Results showed that women with hypertensive disorder during pregnancy were 2.4 times likelier to develop pre-hypertension or hypertension in the ensuing year after delivery compared to those women with normal blood pressure during the pregnancy tenure. It was also seen that in comparison to women with normal blood pressure during pregnancy women with pregnancy-related hypertension were slightly younger and overweight/obese before pregnancy. This surely indicates that women who suffer from hypertension during pregnancy should keep monitoring their blood pressure with a physician after delivery to ensure that BP levels are kept under control. This helps in preventing major cardiovascular risks and complications that might arise in the future. There are evidences suggesting that the immediate few years after delivery are crucial as there is even a fivefold increase in hypertension rate in the first five years after a pre-eclamptic pregnancy. It is possible that 25-45% women with a hypertensive disorder develop hypertension within five years of delivery. So, it is critical that women start taking care of their health even before pregnancy. Every lady in her reproductive years is advised to stay on a healthy weight and lead a healthy lifestyle to prepare herself for the pregnancy that would come her way in a few years’ time. Failing to do so not only increases the complications of pregnancy but also puts the life of both the pregnant woman and her infant at a higher risk of pregnancy-related complications. References Maternal Hypertensive Disorders of Pregnancy & Offspring Risk of Hypertension: https://academic.oup.com/ajh/article/32/4/331/5205123 Hypertensive Disorders during Pregnancy Increase Risk of High Blood Pressure After Delivery: https://www.sciencedaily.com/releases/2016/01/160129090124.htm Risk of Post-pregnancy Hypertension in Women with a History of Hypertensive Disorders of Pregnancy: https://www.bmj.com/content/358/bmj.j3078  Lifestyle & Diet Routine Greatly Affect Bowel Movement Lifestyle & Diet Routine Greatly Affect Bowel Movement Waking up in the morning is a tough job for many and even after getting up, completing the morning chores and getting ready for work is a tiresome routine for some! Brushing teeth, having a bath and dressing up are a regular part of your morning activity but passing stool doesn’t line up as a routine in each of our lives! Though a healthy body routine includes this, not all of us are habituated to smooth bowel movements every day in our lives. Gastrointestinal issues including constipation remain a common condition in adults and children residing in every corner of the world. This not only disrupts morning routine and affects time management but also has a greater impact on the quality of life and well-being of the individual. People avoid using buses, freak out when they are travelling, eating habits change according to bowel movement and general well-being too is dramatically affected. Constipation is pain or difficulty experienced while passing hardened stools or when there is three days in between bowel movements. Every individual faces this problem sometime in life and even healthy individuals become victims despite having no physical or physiological problems. This condition affects almost up to 25% of the population at any given time and is more common in women than men due to factors such as diet, lifestyle, old age, bowel habits and use of medications. Presently, people with constipation problems are recommended lifestyle and dietary modifications apart from other interventions such as stool softeners, osmotic laxatives and stimulant laxatives. But these laxatives sometimes can pave way for unnecessary side effects and it would be preferable to use natural methods to alleviate inappropriate bowel movement. A diet-based change is always the best approach as it is a long-term solution that has no side effects. It is suggested to eat a well-balanced meal that includes bran, whole-wheat grain, plenty of fresh fruits and vegetables, drinking fluids and staying active as a preventive as well as treatment protocol for constipation problems. Basically, it’s a food-based approach that contains aplenty water that’s prescribed as a treatment against constipation. This includes the exotic kiwifruit that has captured the attention of individuals worldwide with its sour-sweet taste and consistency. Though priced a tad higher than many regular fruits kiwis are an excellent source of vitamins and minerals, dietary fiber and polyphenols. Being used as a traditional Chinese medicine the fresh kiwis have been proclaimed to increase laxation in the elderly population due to its high fiber content. Clinical trials show that consuming the whole fruit helps enhance laxation in healthy individuals and also in those individuals with irritable bowel syndrome (IBS) and constipation. Researchers confer these benefits to the presence of soluble and insoluble fiber, polyphenols and the enzyme actinidin present in the fruit. Effect of Kiwifruit-derived Ingredients on Bowel Movement The kiwifruit has a strong Asian origin but are also mostly grown in New Zealand. Actazin and Gold are two powdered ingredients derived from whole New Zealand green (Actinidia deliciosa) and gold (Actinidia chinensis). In both of the varieties, the skin and seeds are removed and the flesh is cold processed for use in supplements. A group of researchers hypothesized that fleshy part in both these varieties played integral roles in improving stool frequency, stool form and gastrointestinal comfort in healthy as well as constipated individuals. The research team selected participants to prove the hypothesis right using several criteria such as age between 18 and 60 years, BMI between 19 and 30 kg/m2, had gastrointestinal symptoms, were vegans or followed a high-fiber diet, had surgery for weight loss, were pregnant or were allergic/sensitive to kiwifruit. Blood samples of the participants were collected at the beginning and end of the study. It was a double-blind, placebo-controlled study which had two groups of participants: healthy participants with no symptoms of constipation and those with functional constipation who met the Rome III criteria for C3 functional constipation. The criteria includes 2 or more of the following: lumpy or hard stools at least 25% of the time, straining at least 25% of the time while passing stools, a sensation of anorectal obstruction or blockage at least 25% of the defecation time, 3 or less than 3 defecations per week, loose stools that rarely occur without using laxatives and insufficient criteria for irritable bowel syndrome. There was a 14-day washout period before the study and all participants consumed 4 dietary interventions each for 28 days with a 14-day washout period between interventions. The interventions included were placebo, Actazin low (Actazin-L) dose (600 mg/day), Actazin high (Actazin-H) dose (2400 mg/day) and Gold (2400 mg/day) which were given in 4*600 mg capsules along with a glass of water. While there were no additional ingredients in Gold powder the Actazin powder contained silica and microcrystalline cellulose. Each of the participants completed a 3-day food dairy at the start and end of the trial, noted down daily bowel movements and well-being parameters. There were 19 participants in the healthy cohort group whose average age was 38 years and BMI 23. There were 9 participants in the functionally constipated cohort whose average age was 44 years and BMI was 25. Results showed that:
Effect of Kivia Powder on Gut Health Kiwifruit has non-digestible oligosaccharides and insoluble fiber that act as a prebiotic by being fermented to small chain fatty acids of butyrate (increases gut motility), acetate and propionate. This combination in the kiwifruit is terrific as both the oligosaccharide and the fiber pass unaltered from the small intestine to the colon acting both as a prebiotic (growth of gut microflora) and as a fiber (to bulk the stool). Kivia powder derived from kiwis is a freeze-dried powder containing Zyactinase, the enzyme actinidin (enhances gastric protein digestion), plant polyphenols, dietary fiber, carbohydrates and oligosaccharides. The study below deals with the benefits of the Kivia powder derived from kiwifruit. Kivia powder contained extracts of kiwifruit prepared by a freeze-drying technique without any solvents or extraction. The placebo contained inactive components such as lemon powder, vital spirulina, citric acid, fructose, sucralose and tropical flavors. The Kivia powder was packed as a 5.5g dose per sachet but both, the placebo and the intervention powder were packed in identical sachets and the participants received a daily dose of one sachet dissolved in cold water along with breakfast. The study included participants aged between 18 and 65 years with a BMI between 20 and 35. All the participants followed the following criteria to be labeled as suffering from occasional constipation: three or fewer defecations per week, straining to pass stools at least 25% of the time, lumpy or hard stools at least 25% times, a feeling of incomplete evacuation at least 25% times, having a sensation of anorectal obstruction or blockage at least 25% of the time and manual maneuvers to facilitate at least 25% of defecations. There were several other exclusion criteria and at the end there were 87 men and women consuming the study product daily for four weeks. Primary endpoint of the study was bowel movement frequency, a parameter used to assess how often an individual has his/her bowel movement; secondary endpoint was to determine the efficiency of the Kivia powder in comparison to the placebo on gut health. Endpoints included stool form (Bristol Stool Scale), bowel urgency (yes/no), abdominal bloating (0 = none, 1 = mild, 2 = moderate, 3 = intense, 4 = severe), abdominal discomfort or pain (0 = none, 1 = mild, 2 = moderate, 3 = intense, 4 = severe), satisfaction with bowel habits (0 = a great deal satisfied, 1 = a good deal satisfied, 2 = moderately satisfied, 3 = hardly satisfied, 4 = not satisfied at all), flatulence (0 = none, 1 = mild, 2 = moderate, 3 = intense, 4 = severe), and burping (0 = none, 1 = mild, 2 = moderate, 3 = intense, 4 = severe). The Bristol Stool Scale is used to classify the form of feces into categories (type 1 = separate hard lumps, like nuts, type 2 = sausage-shaped but lumpy, type 3 = like a sausage with cracks on surface, type 4 = like a sausage or snake, smooth and soft, type 5 = soft blobs with clear-cut edges and passed easily, type 6 = fluffy pieces with ragged edges, a mushy stool, type 7 = watery, no solid pieces, entirely liquid). Tertiary endpoint was to determine the efficiency of the Kivia powder compared to the placebo and quaternary endpoint included determining the safety of the Kivia powder compared to the placebo. There were 87 participants (44 in placebo and 43 in product) but there were 4 withdrawals in the active group and 1 in the placebo group resulting in 43 participants in the placebo and 39 in the active group finally. Results showed that: Primary Endpoint: Participants in the active group witnessed increase in number of spontaneous bowel movements (SBM) every week of the study compared to baseline. Changes in SBM from baseline to week 3 and from baseline to week 4 were significantly higher in the treatment group compared to the control group. There was a significant increase in the number of complete spontaneous bowel movements (CSBM) observed every week compared to baseline. Secondary Endpoint: There was significant decrease in abdominal bloating at the end of every week compared to baseline, significant and nearly significant decrease in abdominal discomfort at the end of week 2 and 4 compared to baseline, abdominal pain or discomfort was lower in the treatment group compared to placebo at week 1 and 3 and significant increase in satisfaction with bowel habits at every week of the study compared to baseline. No difference was observed between the two groups in terms of abdominal bloating and satisfaction in bowel habits. Flatulence was lower for the active group compared to placebo at week 2 and 3. There was a reduction in stool forms 1 and 2 and an increase in stool forms 3, 4 and 5 in both groups. By week 2, there was a significant increase in type 4 bowel movement in the Kivia powder group compared to placebo and by week 3 (follow-up phase), there was an increase in type 5 bowel movement in the treatment group compared to placebo. A clinical trial on Zyactinase was conducted on 58 participants with 30 of them belonging to the placebo group and 28 belonging to the experimental group. The Rome III criteria system was once again used here to measure abdominal discomfort of the participants and from 7 days (run-in period) before the study the participants were prevented from using any dietary supplement or medicine to relieve constipation. After this, there was a 7-day dosing period where each of the participants were given 6 capsules a day either of the placebo or the fruit extract. Again, during the next 7 days they were not allowed to eat anything (supplements or pills) that would facilitate easy passage of stools. Results showed that during the dosing period there was a significant difference in the number of bowel movements per week, though not quite significant there was a slight increase in the frequency of bowel movements per week in the placebo group and during the follow-up phase there still existed significant difference between the two groups. The researchers expressed 0 as an ideal fecal score. The baseline fecal score was 1.9, during the dosing period there was a softening of the stool experienced in both the groups with the active group expressing even potent results. During the follow-up period, fecal score remained low for the active group but for the placebo group the scores increased thereby showing that the fecal stools were also becoming harder again. Abdominal discomfort scores improved drastically for the active group during the dosing and follow-up phase and consumption of 2160 mg/day of kiwi extract returned stools to near normal within the seven-day dosing period and the effect remained intact during the follow-up period. The trial thus shows that the green kiwifruit extract helped inducing normal bowel movements, relieved constipation and symptoms of IBS with no adverse effects. References Kiwifruit-derived supplements increase stool frequency in healthy adults: https://www.sciencedirect.com/science/article/pii/S0271531715000718 Effects of Kivia Powder on Gut Health in Patients with Occasional Constipation: https://link.springer.com/article/10.1186/1475-2891-12-78 Efficacy of Actinidin-containing Kiwifruit Extract Zyactinase on Constipation: https://www.ncbi.nlm.nih.gov/pubmed/29737803 Encapsulated Green Kiwifruit Extract: A Randomized Control Trial Investigating Alleviation of Constipation in Otherwise Healthy Adults: https://pdfs.semanticscholar.org/40a6/6d4a2f551b5835ecea9d00e79db9cec49414.pdf  Most Kids Prefer to Eat Cereals Over Breads & Crackers Most Kids Prefer to Eat Cereals Over Breads & Crackers The world is not in shortage of advertisements for high-fiber biscuits, cereals and other foods to warm people to the idea of a healthy body by gaining access to their heart. Nutrients can be macro- and micronutrients. We are all too familiar with the macronutrients that include carbohydrates, fats and proteins and the micronutrients such as vitamins, iron and zinc but what many of us don’t know is that fiber is a type of carbohydrates that the body cannot digest. It is a good carb that is essential for the body to help it with numerous processes. While most carbs are broken down into sugars and converted into energy fiber passes through the body in an undigested form. Each of us need daily consumption of dietary fiber to prevent individuals from getting hungry sooner, increase satiety levels and regulate blood sugar levels. Kids and adults alike are becoming victims to obesity and overweight. Obesity epidemic in adults is bad but the same in children is worse as it lays the foundation for a future that’s occupied by unhealthy and diseased citizens. We are familiar with obesity and diabetes as serious risk factors for ill health in kids but there does exist a huge gap regarding fiber intake and health in kids resulting in serious constipation problems and digestion issues. These problems affect the day-to-day functioning of the kid affecting his/her quality of life and ruining her/her competency in studies and other streams. It is indeed surprising to know that such constipation problems affect the individual’s well-being even more than those kids with gastric reflux or inflammatory bowel disease. While children and adults need around 15 to 30 grams of fiber per day for good health it is a sad fact that most of us get between 10 and 15 grams only through various sources. The dietary fiber recommendations for children are extrapolated from adult data and there is a serious lack of coherence between intake recommendations and the regular fiber intake levels are fall below recommended ranges. Fiber is classified as dietary and functional fiber-dietary fiber includes nondigestible carbs and lignin that are intrinsic and intact in plants whereas functional fiber includes isolated or purified carbs that are nondigestible, absorbed in the small intestine and have physiological advantages on the individual. Vegetables, whole grains, fruits and legumes are excellent sources of dietary fiber while functional fiber is found in cereals, soups, frozen foods, etc. There are certain whole grains such as wheat and barley that increase dietary fiber consumption levels in children but these are also the foods that are not well-accepted by many kids. It has been seen that children get much of their dietary fiber from foods that are low in fiber density but the good thing is that they consume huge quantities of these foods. It was also seen that kids who eat cereal for breakfast consumed only 1 g of fiber more than kids and teens who skipped breakfast or ate other foods for breakfast. Increased Fiber Intake to Reduce Constipation Rate Increased dietary fiber (DF) was one of the main objectives of American Dietary Guidelines in 2010 but still intake levels remained below recommendations. Such decreased intake is greatly associated with poor diet outcomes and is a serious risk factor for constipation. We might seem to be relieved on reading that the side effects are only as trivial as constipation but what we fail to notice is that functional constipation has a worldwide prevalence between 7 and 30% and comes with painful symptoms that debilitates the life of the kid. While reduced fiber intake remains a risk factor for constipation children suffering from it have lower fiber intake than healthy kids. We do have evidences linking the benefits of consuming fiber on constipation problems in kids making it one of the best solutions and finest treatment options. Intake of DF foods such as veggies, fruits and whole grains is linked to better diet quality that’s high in nutritive value in younger kids while the same is linked to reduced fat consumption in older kids. Hence, it is clear that there is a need for increasing DF intake to reduce the risk of constipation. A study was conducted on the same to check the effectiveness of DF intake with the help of introducing two high-fiber snacks per day on gastrointestinal function and nutrient intake in kids aged 7-11 years. Randomized Controlled Study The study on 7-11-year-old kids was conducted for 8 weeks in an elementary school on children whose teachers granted permission. 11 teachers granted permission for the study on their kids but it was seen that children with digestive disorders, food restrictions and food allergies were not included in the study. During the intervention period the participants were asked to consume two high-fiber snacks per day (all 7 days of the week) and the control group continued consuming their regular snacks irrespective of whether or not the snacks contained any fiber. All the participants were collected information on their gastrointestinal function and regular dietary pattern at the start of the study, again another set of details were collected midway through the study (4th week) and finally, a third set of data was collected after the eighth week of study. Each child in the intervention group was given 2 high-fiber snacks which were selected based on their fiber and energy content such that the snacks fulfilled 10-12 g and also with the goal of increasing the consumption by 8 g per day. Every child who consumes both the snacks consumed around 314 kcal and 10.2 g of fiber per day. Along with the snack, all the kids were provided with a 30-ml glass of slim milk to avoid any GI distress. The beverage was included during each snack as too much of fiber intake too suddenly can cause constipation, gas and bloating and the person can relieve this discomfort by consuming fluids. Fiber is required for solid bowel movements but too much of it can cause constipation as well. All of the snacks were deprived of its original packaging, repacked by the team and served. Each of the kid’s consumption was marked as ‘none’, ‘one-quarter’, ‘one-half’, ‘three-quarters’ or ‘all’. The snacks offered included: Kellogg’s Frosted Mini-Wheats Little Bites Chocolate® Kellogg’s FiberPlus Cinnamon Oat Crunch® Kellogg’s Frosted Mini-Wheats Little Bites Original® Kellogg’s Cracklin Oat Bran® Kellogg’s Frosted Mini-Wheats Bite Size Blueberry Muffin® Kellogg’s FiberPlus Berry Yogurt Crunch® Kellogg’s NutriGrain Bar® Kellogg’s Frosted Mini-Wheats Big Bite® Kellogg’s Frosted Mini-Wheats Blueberry® Kellogg’s Frosted Mini-Wheats Strawberry® Kellogg’s Frosted Mini-Wheats Touch of Fruit in the Middle Mixed Berry® Crackers Kellogg’s Special K Snack Crackers - Savory Herb® Kellogg’s Special K Crackers Multigrain® Kellogg’s All-Bran Crackers Multi Grain® Breads Sara Lee Soft and Smooth White Bread with Whole Wheat® Sara Lee Soft and Smooth 100% White bread with Ca/Vit D® Pepperidge Farm Deli Flats (Whole Grain White)® Thomas 100% Whole Wheat Bagel Thins® Pepperidge Farm Stone Ground Whole Grain Bread® Thomas 100% Whole Wheat Mini Bagel® Arnold Whole Wheat Bread® Arnold Sandwich Thins® Thomas Light Multi-Grain English Muffin® Thomas Plain Bagel Thins® Snacks were given at a time convenient for both teachers and students but there were occasions during which the snacks could not be served twice a day at school. During such occasions, the snacks were given home and the same protocol as the one followed during weekends was put into practice. All the kids were given a paper bag with two options for each snack occasion and were instructed to return the empty or full snack bag after the weekend to the research staff in the school. The parents and the kids were requested to fill an 8-question Questionnaire on the child’s digestive health. Two recalls were taken-one between Monday and Thursday and another one between Friday and Sunday via telephone. The average of the two recalls were used to jot down regular intake and total energy intakes below 500 kcal or above 3500 kcal were ignored for the study. Results A total of 80 kids participated in the study and initially there was no difference in energy intake between the intervention and the control group.
Constipation Constipation is characterized by infrequent bowel movement, difficult stool passage and unsatisfactory defecation. A community-based study in Hong Kong on 3-5-year-old kids found that 30% suffered from constipation and so did close to one-third of kids in United Kingdom. Both the studies showed that kids who ate a high-fiber diet did not suffer from constipation and so did an Irish study on 5-8-year-old kids proved that constipation rates were almost double in those kids who failed to eat a high-fiber diet compared to those who had sufficient fiber intake. There are several studies showing that increasing fiber intake is the best first step to decrease the effect of chronic constipation in otherwise healthy children. Different fibers have different effects on the body and by examining isolated fibers the effect of each on constipation could be analyzed in detail. In one study, children were given bran fiber and it was shown that those kids who showed improvements in constipation had higher fiber and bran intake than kid whose constipation did not improve or worsen too. In another study, children with chronic idiopathic constipation were given cocoa husk that resulted in less hard stools compared to those kids who received a placebo. Glucomannan, a special fiber, was given to kids with chronic functional constipation which improved stool consistency in almost 62% of these kids and also in 23% in the control group. Researchers found that giving fiber-rich foods to kids improved constipation levels according to both parents (68 vs. 13%) and kids (42 vs, 13%). There are numerous clinical studies available presently that support the importance of fiber intake on bowel function but sadly, caretakers including parents, grandparents and even healthcare providers are not ready guide their children’s fiber intake. Though fiber affects a person’s health in the same way as sugar or salt, fiber has not been able to reach people in the same vigor as the other two. Making people aware of the health benefits of consuming fiber will help in promoting and increasing fiber intake. References The Effect of Providing High-fiber Snacks on Digestive Function & Diet Quality in a Sample of School-age Children: https://nutritionj.biomedcentral.com/articles/10.1186/1475-2891-12-153 What do we Know about Dietary Fiber Intake in Children & Health? https://academic.oup.com/advances/article/3/1/47/4557086 Fiber: https://www.hsph.harvard.edu/nutritionsource/carbohydrates/fiber/ Do you know that sleep is as important as exercise and diet to your body? Sleep replenishes energy, makes you active and keeps you healthy lack of which can land you in much trouble than you could imagine. The advent of smartphone era and electronic gadgets has ruined our lifestyles, pushed our sleep hours dramatically to 12 or 1 o clock in the night and shift work has brought upon a culture where we eat and sleep anytime of the day or night without minding our natural body clocks and circadian rhythm. Circadian rhythms are integral to each of us regulating our sleep-wake cycles and feelings of sleepiness/wakefulness over a 24-hour period. It works based on the area of the brain that responds to light which clearly shows why we sleep when its dark and remain alert when the outside sun shines brightly. We humans have evolved into creatures who don’t listen to our parents, siblings, spouses or anyone else doing what we like and liking what we do. While we do understand the importance of sleep with regards to regular bed timings, wake up hours and sleep duration to keep us healthy we don’t monitor the same nor do we try doing it. The invention patented here comes to our rescue here as it helps in assisting and guiding the user to set goals that promote consistent sleeping behavior. In fact, the methods and techniques discussed here promote sleep consistency and improve sleep quality.
While the general recommended hours of sleep are between 7 and 9 hours sleep requirements and durations differ from person to person in order to lead a healthy life. The invention here comes with a personalized recommended sleep duration that’s more precise (for example, 8 hours ±0.5 hours) in comparison to 7-9 hours that’s recommended generally. A ‘sleep session’ is the period of time during which the individual is actually sleeping or attempting to sleep too. It depends on the sensors too-sensors might indicate the time beginning from when a person first enters the bed to sleep, the individual might manually indicate to a biometric monitoring device the beginning of a sleep session or when a processor determines that the individual has started to sleep. Likewise, the end of the sleep session might be noted when the person exits a bed, the individual manually notes the end of the sleep session on the biometric monitoring device or again, if the processor has determined when the person stops sleeping. The start and end time of sleep sessions depend on the criteria used to determine the parameters. Wearable fitness trackers such as Fitbit might be treated as biometric monitoring devices to collect biometric sensor data or it might even be sleep-monitoring systems attached to mattresses or even operating from somewhere close by such as from a nightstand or so. An individual goes through different states such as awake state, asleep state, waking state, etc., Again in sleep state the individual might be in REM or non-REM state and its not mandatory that an individual passes through each of the states while sleeping and the sleep duration determines the amount of time an individual spends in one or more sleep states that represent one or more stages of sleep. The biometric monitoring device might determine the time spent in each of the sleep states. After obtaining sleep parameters such as selected sleep duration, scheduled waketime and selected bedtime along with the individual’s selected sleep duration the individual’s sleep schedule may be tracked to find out how consistently the individual is meeting sleep duration goals. Sometime down the line the individual’s scheduled waketime and selected bedtime might also be clocked. Sleep monitoring is done by storing the sleep data in a sleep log data store that associates logs with specific users and sleep efficiency is calculated by monitoring the total time in a sleep session that an individual is in one or more sleep states or is not in an awake state divided by the sleep session duration. For instance if an individual goes to bed at 10.00 pm and falls asleep after 30 minutes, wakes up through the night for a total of 30 minutes and finally wakes up at 6.00 am in the morning the total time duration in bed is 8 hours (10.00 pm to 6.00 am) but he/she was actually sleeping (non-awake state) only for 7 hours (excluding 30 minutes to fall asleep and 30 minutes of waking up through the night). The sleep efficiency of the individual is 7 hours divided by 8 hours which is 0.875. Sleep efficiency changes based on different factors such as sleep environment, physiology, caffeine intake, timing at which the person retires to bed and so on. For example, if the person goes to bed early then he/she is less tired and spends more time trying to fall asleep but if the person goes to bed later, he/she is more tired and falls asleep more easily. In practice, sleep efficiency is always lesser than 1. The invention displays a bedtime reminder in advance to remind the user to go to bed. Sometimes, snooze option in the reminder is also possible and the reminder is generally set based on the sleep state duration data of the user for the previous sleep session. The user might even be congratulated after a sleep session in which the user achieves bedtime target. The invention is of paramount importance as it guides the user and sets the user’s sleeping routine in a disciplined way. The patent was published on December 7th, 2017 and for more information on the patent please visit: United States Patent & Trademark Office: http://patft.uspto.gov/netacgi/nph-Parser?Sect1=PTO2&Sect2=HITOFF&p=1&u=%2Fnetahtml%2FPTO%2Fsearch-bool.html&r=2&f=G&l=50&co1=AND&d=PTXT&s1=%22sleep+consistency%22&s2=%22jacob+antony%22&OS=%22sleep+consistency%22+AND+%22jacob+antony%22&RS=%22sleep+consistency%22+AND+%22jacob+antony%22 World Intellectual Property Organization: https://patentscope.wipo.int/search/en/detail.jsf?docId=US206639948&_cid=P11-JYSF1P-05579-1 European Patent Office: https://worldwide.espacenet.com/publicationDetails/biblio?DB=EPODOC&II=0&ND=3&adjacent=true&locale=en_EP&FT=D&date=20171207&CC=US&NR=2017352287A1&KC=A1 The world is becoming vegan-friendly as a greater number of individuals have started adopting a vegetarian/vegan diet. Ironically, the shift is seen prominently in non-vegetarians who have started following a vegetarian diet owing to several personal reasons whereas, increasing number of vegetarians are turning out to be chicken, meat and fish lovers. Call it open-mindedness, an interest to explore different cuisines or simply the urge to do something forbidden, this transition wasn’t expected! As we see vegetarian, semi-vegetarian and even the stricter vegan diet that excludes even dairy and eggs apart from meat and fish becoming popular their nutritive quality and the ability to satisfy nutrient requirements have always been questioned. People adopt a vegan/vegetarian diet owing to different reasons and the most famous of all is health. These people believe that avoiding consumption of animal products helps prevent the risk of bacterial and other foodborne diseases and also avoid excess intake of saturated fat cholesterol and sodium. There are some who believe a plant-based diet to be rich in nutrients, phytochemicals, fiber and flavonoids, some who don’t eat due to their opposed view on the slaughter of animals for food and others who don’t eat simply due to religious beliefs.
Vegetarian diets are rich in fruits, vegetables, whole grains, legumes, nuts, seeds and soy foods and their characteristics have maximum benefits on the heart, have been associated for a long time with reduced blood pressure rates, reduced inflammation and have also decrease the risk of diabetes, cancer, renal diseases, rheumatoid arthritis and even obesity. Obesity has always been linked to various co-morbidities but the underlying mechanism for these isn’t clear. We have data linking adipose tissue inflammation and chronic diseases associated with obesity. Adipose tissue macrophages (ATMs), especially pro-inflammatory macrophages (M1 ATMs) are linked with insulin resistance. What remains a mystery is whether the accumulation of ATMs in human beings is only related to fat gain or whether it is related to diet also. Ceramides, a family of lipid molecules composed of sphingosine and a fatty acid, is found in high concentration within cell membrane of cells and has often been linked to inflammation and insulin resistance in muscle cell models. Increased exposure to saturated fatty acids shows increase in ceramide levels in rodents and these molecules have also been linked to adverse muscle profiles in humans. In such a scenario, researchers wanted to know whether pursuing a vegetarian diet would benefit the obese individual such that he/she would have less adipose inflammation and reduced muscle ceramide content in comparison to similar obese individuals who follow a non-vegetarian diet. The adipose tissue is a complex organ that comprises of a variety of cell types with diverse energy stores, metabolic regulation and neuroendocrine and immune functions. When obesity strikes, the adipose tissue succumbs to disorders, its function and distribution is affected and also has effects on cytokine, lipid storage and composition of adipose-resident immune cell population causing advanced consequences on inflammation and insulin sensitivity. Earlier studies detected lipid composition differences of adipose tissue in rats which were fed a diet rich in polyunsaturated fatty acids (PUFAs). Linolenic acid is the major PUFA present in human adipose tissue and allows estimation of the stored essential fatty acid. The fatty acid composition of the adipose tissue is closely connected to the dietary fat content and studies show that individuals on a long-term vegan diet display increased composition of PUFAs and reduced levels of saturated fatty acids compared to omnivores and even vegetarians. Study on whether A Vegetarian Diet Leads to Less Adipose Inflammation The study included 16 participants among which 8 of them were vegetarians and 8 were omnivores. All the participants were of the same age and BMI without any chronic conditions such as diabetes or cardiovascular disease. All the vegetarian participants assured following a vegetarian/vegan diet for at least last 5 years and among these 8 participants 2 of them were vegans, one was a lacto-ovo vegetarian, one was a pescatarian and four were lacto-vegetarians. Blood samples were taken, a food frequency questionnaire was given and subcutaneous abdominal and femoral adipose tissue biopsies were collected using a needle liposuction technique. Muscle biopsies were also collected and tested for sphingolipids concentration. Plasma total free fatty acid (FFA) concentrations were measured and plasma IL-6 and TNF concentrations were measured. Fat cell size was measured and composition of fatty acids in tissue lipids were also assessed by extracting tissue lipids. For immunohistochemistry (IHC), adipose tissue samples were taken and viewed under a microscope. Two observers took 10 random images of the slide and counted the number of positively stained macrophages, crown-like structures (CLS) and total adipocytes for each image. Resulting data was expressed in terms of number of positive cells per 100 adipocytes. RNA samples were isolated from abdominal and femoral adipose samples for all omnivores and 5 of 8 vegetarians and analyzed. Results Both the groups did not differ greatly with respect to age, BMI, body composition or blood pressure. Fasting plasma insulin concentrations, plasma IL-6 and TNF concentrations did not differ between the 5 omnivores and vegetarians taken for sampling. The answers in the FFQ helped researchers to confirm that vegetarians adhered to a plant-based diet and also could find out no significant difference in macronutrient and micronutrient intake among vegetarian subtypes. Total calorie intake showed not much of a difference between the two groups; total saturated fat intake was lesser in the vegetarian group but there was no difference found in the case of monounsaturated and polyunsaturated fat intake between the two groups. Individuals following an omnivorous diet consumed more of cholesterol and vitamin D while vegetarians ate more of fiber and vitamin C. Vegetarians had more of oleate in the abdominal depot than omnivores and also had more of oleic, palmitelaidic, linolenic and myristic fatty acids in the femoral depot. Plasma FFA palmitate occupied a lesser percent of total FFA in vegetarians compared to omnivores while other fatty acids did not show any significant difference. Both the groups did not show any difference in the abdominal or femoral adipose tissue depot macrophage burden and the number of abdominal adipose tissue macrophages was also not different when expressed per 100 adipocytes. Vegetarians had fewer femoral CD68 and CD14 macrophages compared to omnivores. Omnivores had more CD206 macrophages in femoral fat than vegetarians. Adipose tissue TNF mRNA expression was greater in omnivores than vegetarians but there was no significant difference in femoral adipose tissue expression of either TNF mRNA or IL-6 mRNA between the two groups. There was no difference seen in muscle ceramide concentrations between the two groups nor any significant correlation found between adipose tissue macrophage burden and intake of total calories, total fat, saturated fat or polyunsaturated fat. Trans-fat and added sugars intake were correlated with total macrophage burden and there was a positive correlation between abdominal CD206 macrophage and monounsaturated fat intake and omega-3 fatty acid intake. The study clearly shows that individuals following a vegetarian diet for at least 5 years consume less saturated fat and is also linked with reduced femoral adipose tissue inflammation. For all those of you who have been struggling to succeed with a switch over from your favorite non-vegetarian diet to a vegetarian diet, this article would definitely be a motivating factor to continue your endeavor as it is not only good for health, helps in weight loss and reduces the risk of diseases but also helps in sustainable living. References Preliminary Evidence for Reduced Adipose Tissue Inflammation in Vegetarians Compared with Omnivores: https://nutritionj.biomedcentral.com/articles/10.1186/s12937-019-0470-2 In Vivo NMR, Applications, Other Nuclei: https://www.sciencedirect.com/topics/agricultural-and-biological-sciences/adipose-tissue  In an Age to Run & Play these Kids are Going Astray with Increased Screentime In an Age to Run & Play these Kids are Going Astray with Increased Screentime 21st century is the age of technology and the adorable MTS baby ad (the baby starts using technology right after getting out of the mother’s womb) would be a reality-don’t you think (or rather fear!) so at least in a couple of decades? Kids and adolescents grow up surrounded by digital information and entertainment with the means of computers, tablets, smartphones and televisions. These young people spend more time online rather than spending quality time with family and friends. The digital world is full of amazement and surprises for these kids who love interacting with virtual friends, make friends without inhibitions as they need not bother about their physical appearance and have lots of fun playing games to which they get addicted to in course of time. The world outside is cunning and business minded. It loves to exploit the children’s weaknesses by developing sensational games that kids would love to explore, play repeatedly and finally shell out money purchasing different apps or unlocking levels. The days of football and basketball are fast disappearing as kids lock themselves in their rooms focused on the tablet or laptop for hours together. This indeed raises the concerns of health professionals and parents who are of the concept that prolonged screen time is bad for health especially with the magazines and the media reporting their harmful effects every other day on sleep, diet, social life and family life. But research studies are not many as many of them mostly include negative behavior such as snacking, sedentariness and socioeconomic grouping too as factors in their study. We do have evidences that increased screen time is associated with obesity, decreased time available for exercise, increase in energy intake and reduction of metabolic rate. There are also side effects such as irritability, mood disorders and poor cognitive performance all of which affect academic performance. Such factors affect quality of life and there have been several guidelines proposed for reducing screen time-the American Academy of Pediatrics in 2015 recommended limiting screen time for children aged 2-5 years to an hour everyday and for those above 6 years it is up to the parents to rationally decide upon a fixed screen time for their children. The Canadian Pediatric Society too came up with similar guidelines in 2017. While time and again we have been insisting on limiting or preventing infants and toddlers from being introduced to gadgets and technology it is depressing to realize that the use of media has only been rising steadily for the past 5-10 years. Kaiser Family Foundation Studies report in 2010 suggested that behavior of 2,000 8-18-year-old kids showed that most of them spent around 7.5 hours daily on media where around 4.31 hours was spent viewing television, 2.31 hours listening to music, 1.29 hours on computer and 1.13 hours playing video games. Yet another study found that youngsters aged around 18 years spent nearly 40 hours every week accessing Internet from home computers. In order to exactly find the effect of these things on kids a review of reviews (RoR) was taken on children and young people (CYP). Review of Reviews The review study question was ‘What is the evidence for health and well-being effects of screen time in children and adolescents?’ Based on different criteria finally 13 studies were included in the review-6 of them considered the association of screen time with body composition measures (including obesity), three for diet and energy intake, seven for mental health related outcomes like self-esteem and quality of life, four for cardiovascular risk, four for fitness, three for sleep and one for pain and one for asthma. We will take up each of these one by one. Body Composition: Most of them were associated with television screentime. Most of the studies unanimously reported increased screen time with increase of overweight/obesity over time. Carsen et al reported that increased adiposity measure was associated with computer screentime in almost 3/4th of the studies but the same team could not find any association between video/videogame screentime and adiposity. In another study Ekris et al reported that across 6971 participants from five prospective cohorts BMI at follow-up was not linked to every added hour of computer viewing. While there is moderate evidence that higher screen time is associated with greater adiposity there is not enough evidence for an association with overall screen time or non-television screentime. Diet & Energy Intake: Screentime in the absence of food commercials still resulted in elevated dietary intake and television screentime increased the consumption of palatable energy-dense foods while evidences were weak for video game screentime. Costigan et al reported that screentime did not promote healthy eating behavior, Pearson and Biddle showed that television screentime was associated with total energy intake and energy dense drinks. Here again, we have moderate evidence linking screentime with high energy intake and less healthy diet quality. Mental Health & Well-being: There was moderate association between anxiety and screentime while positive association between screentime and depression. High rates of depression were linked to ≥2 hours of screentime daily. Carsen et al reported that screentime and behavioral problems were positively associated in 24 studies. There was a positive association between screentime and poorer psychological well-being and quality of life. Physical Health: There was weak association between screentime and cardiovascular risk factor generally. While Costigan et al reported that higher screen time was associated with higher physical activity two other reviews found an inverse association between both. CYP cognition and development were examined in three medium-quality reviews. LeBlanc et al conveyed that there was low-quality evidence that television screentime had negative impact on cognitive development in young children. Many studies acclaimed that there was weak evidence that greater television time was associated with poorer educational attainments. Sleep: There was weak association between screentime and sleep outcomes in all types of media exposure including computer, video screentime and mobile phone screentime. Pain was studied in very few studies and those showed a weak association between screentime and increase in neck/shoulder pain. Likewise, there was insufficient evidence linking asthma with television screentime. This research shows that increased screentime was positively linked with a variety of health harms for CYP having strongest evidence for adiposity, unhealthy diet, depressive symptoms and quality of life. Association between screen time & psychological well-being We have a study where the effects of screentime on psychological well-being was specifically measured on 44,734 children and adolescents 2 years of age and older in the US in the National Survey of Children’s Health (NSCH) conducted in 2016. All the children were between 2 and 17 years of age and were grouped into four categories: Preschoolers 2-5 years old (9361), elementary schoolers 6-10 years old (10,668), middle schoolers 11-13 years old (7555) and high schoolers 14-17 years old (12,753). Two questions on screentime were asked to caregivers (who are the participants here):
Studies show depressing results in terms of life skill development in children. More number of children between 2 and 5 years of age could use technology in a better way than demonstrate skills such as riding a cycle, swimming or tying their shoelace. Lack of enough playtime with traditional toys such as building blocks showed that language development is affected greatly. When toddlers (between 18 and 30 months of age) played building blocks with their caretaker, these toddlers showed improved language scores comparatively. Also, children who view television are captured by the attractiveness of the visual images and colors but mostly forget to pay attention to the storyline thereby failing to learn much from these fictional TV episodes. More time spent viewing per day at ages one and three were associated with attention problems at age seven. Excessive use of television, video games and computer was linked to excess use of tobacco and cigarettes, early sexual debut, sleep deprivation especially when there is a television set in the bedroom (these kids score 7-8 points lower in math tests compared to those without a TV in the bed room), violent behavior not only that’s physical but also verbal, depressive symptoms and anxiety. A study from UCLA showed that screentime was associated with identifying emotional cues of individuals. Study compared a group of people in a nature camp who went without screentime for five consecutive days to another group who were bound to attend the camp later. The first group of people displayed improved emotional cognitive abilities just five days after the camp. The increase in screentime impairs social skills and affects the ability of people to understand emotions of other people. Screentime definitely impairs social development, emotional intelligence, cognitive improvements and overall quality of life. Kids lose the personal touch with other individuals and fall in love with the virtual world ignoring the presence of the people around him/her. It is 100% essential to control screen time in children and help them enjoy a better quality of life. Research Effects of screentime on the health and well-being of children and adolescents: https://bmjopen.bmj.com/content/9/1/e023191 Association between screentime and lower psychological well-being among children and adolescents: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6214874/ The impact of media use and screen time on children, adolescents and families: https://www.acpeds.org/the-college-speaks/position-statements/parenting-issues/the-impact-of-media-use-and-screen-time-on-children-adolescents-and-families The world might be dominated by youngsters owing to their attitude and behavior but speaking mathematically, we are dominated by older adults. Look around and you are sure to see a greater number of older adults everywhere around you. This segment of people seems to be the fastest growing segment in the world and they outnumber kids aged under five in both developing and developed countries. From a humble 500 million this number is expected to spike up to almost 1.5 billion by 2050. Due to such growth in the global elderly population there seems to be a sharp rise in cognitive decline and dementia rates which are emerging to be one of the greatest public health problems faced by the world. Ageing is associated with memory issues and however sharp our memory skills might be during our younger years we tend to forget things, names and issues as we grow old. Its not a rarity to see our parents search for their reading glasses everywhere in the house while it is sitting right in their neck, grandmas often look around for their knitting needle while it is present right in the cloth and our grandpas keep repeatedly enquiring about their term deposits irrespective of the fact that its being handled well by their children. All these are not abnormal and I would call it part of the ageing process. Cognitive decline might include these things that are a regular part of normal ageing, mild cognitive impairment (MCI) or severe dementia with the last being the most excruciating experience by those undergoing the phase and those staying with the patient as well. Dementia rates have been steadily rising and the numbers are projected to be anywhere around 81.1 million by 2040. Dementia is a disease that not only affects the person involved but also places significant burden on the caretaker, affects the quality of life of both the individual affected and his/her families and above all, places significant burden on health care resources.
Despite such worldwide prevalence of dementia, we don’t have any cure for it until now and rely on pharmacological and non-pharmacological approaches to minimize symptoms and delay the progression of the disease. Coming up with effective preventive strategies that could delay dementia and identifying modifiable risk factors that could prevent cognitive decline and improve the lives of the elderly is the need of the hour. Diet is one of the most potential non-pharmacological approaches to ageing successfully and we do have a number of studies showing that nutrition plays a pivotal role in having a positive effect on dementia. Time and again we have seen positive data emerging on the association between nutrients such as antioxidants, folate, omega-3 and omega-6 fatty acids but not much studies have focused on the effect of dairy foods and milk in altering dementia risk. We are going to see analysis and studies that help us get a clearer picture on the impact of dairy on dementia risk. While dementia is the last stage of cognitive disability cognitive decline is the first stage and MCI exists in between these two. Many individuals experience subjective cognitive decline (SCD) before moving on to greater cognitive impairment. SCD is a preclinical sign of Alzheimer’s and can happen before cognitive impairment. Dementia Risk & Dairy Consumption: A Review A database search was done based on search terms such as dairy, milk, yogurt, food, intake, consumption, cognition, cognitive decline, cognitive performance, cognitive function, cognitive state, mild cognitive impairment, Alzheimer’s, depression and mental illness. While the search resulted in 216 studies only 30 of them were relevant. But 22 papers were omitted as they were either on soy, vitamin D or milk probiotics, they did not include cognitive measures, indicated only dairy intake and survival risk or were reviews. Finally, only 8 papers suited the study purpose all of them consisting of three cross-sectional and 5 prospective studies (study duration was 3.3 years to 30 years). Six studies included both males and females, 1 study included only males and 1 study included only females with sample sizes between 449 and 4,809 in all of them. While the participants were all middle-aged to elderly people some studies employed only those above the age of 60. One cross-sectional and five prospective studies used a food frequency questionnaire to assess dietary intake while the other cross-sectional studies used a 24-hour dietary recall. Two cross sectional and one prospective study reported benefits due to dairy consumption with respect to dementia risk. In cross-sectional studies, decreased dairy or milk intake was linked to poorer cognitive function in elderly women with no difference found in the case of men. Greater the cheese intake lower was the risk of cognitive impairment in the elderly population but 2 studies showed no link between milk intake and dementia risk. One prospective study showed that milk intake was linked to risk of vascular dementia in older age in both men and women. Three studies found a negative link between dairy and dementia risk. The CAIDE study showed that the fat intake from the milk and dairy products were linked to a greater risk of dementia, MCI, AD and other cognitive inabilities. It showed that higher fat intake was associated with increased risk of MCI and poorer cognitive function but not with dementia or AD risk. Another Australian study on elderly men showed that consumption of full-fat milk was associated with impaired cognitive function and the third study showed that increased consumption of dairy desserts and ice creams was linked with increased risk of cognitive decline among French women. In general, two studies found that whole-fat milk consumption was associated with poor mental health in elderly men whereas decreased milk intake was linked to depressive symptoms. While 3 studies suggest that dairy consumption has beneficial effects on cognitive function there are 4 studies that show that consumption of dairy products is associated with cognitive decline in the elderly which leaves us in an inconclusive state. Effect of Dairy Consumption on the People of North America Age-related cognitive decline is often seen in areas such as executive functioning, attention, processing speed, episodic memory and visuo-spatial functioning. Memory-related cognitive impairment increases with age affecting up to 50% adults aged 65-74 years compared to 88% of older adults aged 85 years and above. In the case of sematic and implicit memory cognitive function remains intact. Milk, cheese and yogurt are rich sources of vitamin B12, vitamin D and alpha-lactalbumin-this results in bioactive peptides when partially hydrolyzed and in tryptophan and cysteine when fully hydrolyzed. These components are what help in cognitive function directly or indirectly. Directly, they increase the production of ‘serotonin’ which helps in mood regulation and cognitive function and also to improve deficiencies and abnormalities in older adults’ cognitive function. Indirectly, dairy components work by mediating effects on cardiometabolic health. Dairy products and milk consumption help in improving cardiovascular health by negating any risk factors linked with metabolic syndrome. This change in cardiometabolic health imparted by high dairy intake might be the primary way through which dairy products impair cognitive decline. A study was conducted on 32 participants (8 males and 24 females) whose average age was 70.59 years. Dietary feedback was taken and disappointingly only 10 participants reported consumption of the recommended amount of dairy (3 servings per day) and the remaining 22 participants had only one or two servings per day. Almost 85% of all the participants took dietary supplements, most of them took 13% saturated fats which was way above recommendations (7%) and had their cholesterol level well within recommendations (<300 mg per day). All of them had normal cognitive function and were physically fit. Number of Dairy Product Servings & Cognitive Performance: Tests were done to find differences between those individuals consuming <3 and >3 servings of dairy per day but results showed no differences in any of the cognitive tests. Dairy Product Nutrient Intake & Effect on Cognitive Performance: Dairy products contain saturated fats, vitamin D and calcium and the effect of these nutrients on cognitive performance was assessed. While saturated fat was negatively associated with cognitive performance there was a positive correlation between vitamin D intake and performance on three cognitive tests. Calcium in dairy products showed no positive or negative correlation with any of the cognitive tests performed. Linear regression analyses showed that none of the nutrients were predictors on any of the cognitive tests. Nutrients from dietary intake including dairy were uniquely associated with specific cognitive functions in older men and women. A Meta-analysis on the Impact of Dairy Intake on Dementia Search was carried out on three different databases to pick out those studies that compared dairy consumption and its effect on cognitive function (including those in any stage of dementia and having any type of dementia). The database came up with 2407 results and after several elimination rounds only 8 articles (1 randomized control trial (RCT) and 7 prospective cohort studies) were included in the study. RCT: Participants in the RCT were fed a low-dairy (one serving of reduced-fat dairy food everyday) diet or a high-dairy diet (four servings of reduced-fat dairy food daily) for six months followed by an alternate diet for another 6 months without any washout period. Verbal memory, processing speed, working memory, visual attention, verbal fluency, abstract reasoning, selective reasoning, executive function and psychological well-being were used to measure cognitive performance among which only backward spatial spin working memory showed significant difference between high-dairy and low-dairy diet groups. Cohort Studies: Two studies analyzed dairy and milk intake and its effect on cognitive function among older individuals after 5-20 years of follow-up in France and US. One study analyzed milk intake using a food frequency questionnaire (FFQ) and another analyzed dairy and milk intake using a 24-h recall. Two studies analyzed the impact using tools that predict cognitive function and both of them showed mixed results. While the first study showed that higher milk intake was associated with poor memory performance the other study showed that higher milk intake was negatively associated with executive function with no effect on verbal learning, short-term memory, executive function or expressive language. One cohort study found that regular consumption of full-cream milk decreased successful mental health ageing compared to rare consumption group, two studies showed no impact of dairy or milk consumption on cognitive decline and meta-analysis results did not show significant differences in risk for cognitive decline or cognitive impairment by comparing highest milk intake to lowest intake groups. Two studies analyzed the impact of dairy on people with Alzheimer’s disease and their results were inconsistent. One study showed that consuming milk less than twice a week was not associated with the risk of developing Alzheimer’s compared to drinking milk daily or 2-4 times a week. The other study showed that higher consumption of milk and dairy intake significantly reduced the risk of Alzheimer’s disease. Two studies analyzed the risk of vascular dementia and just like the study on Alzheimer’s the results of these were inconsistent. One study analyzed the effect of dairy consumption on all-cause dementia and showed no significant link between dairy/milk consumption and risk for developing all-cause dementia. Overall, the evidences are inconsistent with each other and it is not enough to show that dairy and milk consumption does have an effect on cognitive decline/dementia. Still, dairy is an important food group that ought to be included in our daily meals for nutrients and good health. References Review of Dairy Consumption & Cognitive Performance in Adults: https://www.karger.com/Article/PDF/320987 The Relationship between Dairy Product Consumption & Cognitive Performance in a Group of Community-dwelling Healthy Older Adults: https://pdfs.semanticscholar.org/7c2b/39d304985a3deec6eaf11478df9df733d3b6.pdf Role of Milk & Dairy Intake in Cognitive Function in Older Adults: https://nutritionj.biomedcentral.com/articles/10.1186/s12937-018-0387-1 We see almost none without hypertension or sugar once individuals cross their 50s as these chronic diseases are extremely prevalent and common these days even in those in theirs 20, 30s and 40s. Any individual going for a diagnosis or health check up to the doctor is immediately checked for his/her BP levels and also questioned on medical history to gauge whether hypertension was the result of improper lifestyle habits or something beyond that-such as stress or genes. We live in a competitive world that offers us with ample opportunities to learn, enjoy and be happy in life as well as corners us with its overexposure and cut-throat competition that makes individuals treat each other as enemies or competitors rather than as fellow citizens who wish to succeed in life. Such attitudes and challenges increase stress levels which indeed affect blood pressure levels. Hypertension (HTN) is a global health problem existing as the foremost cardiovascular risk factor worldwide contributing to more than 50% of prevalent coronary heart disease and almost 2/3rd of cerebrovascular disease burden. There does exist the fact that hypertension is genetic but our lifestyle methodologies including diet such as too much of sugar and salt or too little of antioxidant vitamins play primary roles in deciding upon hypertension risk.
Antioxidant-Reactive Oxygen Species-Hypertension Cardiovascular disease is seen along with enhanced oxidative stress (OS) in the vascular wall, heart, kidney and brain. OS induces inflammation, endothelial dysfunction and increased vascular tone resulting in vascular contractility, structural remodeling and hypertension. The process by which reactive oxygen species (ROS) are conveyed is not entirely clear and also the relationship between hypertension, antioxidants and oxidative stress is quite complex and not fully understood. We have several studies showing that hypertension may develop due to increase in reactive oxygen species and also that antioxidants definitely help in relieving hypertension burden. ROS paves way for vasoconstriction and increased vascular resistance by altering balance in the endothelium between vasoconstrictors such as thromboxane and isoprostanes and vasodilators such as nitric oxide. On the other hand, oxidative stress raises blood pressure by promoting nitric oxide deficiency, augmenting arachidonic acid oxidation and formation of vasoconstrictive prostaglandin. This oxidative stress which creates an imbalance between pro-oxidants and antioxidants thereby resulting in startling changes in the endothelial cells plays a critical role in the development of hypertension. Antioxidants have become very much popular these days as they seem to fight against free radicals and inhibit oxidation. Free radicals are unstable molecules formed during normal cell metabolism. They build up within cells and affect nearby molecules such as proteins and lipids thereby increasing the risk of diseases. Certain studies show that specific antioxidant vitamins such as vitamins C and E and pro-vitamins such as beta-carotene are majorly involved in preventing diseases but this approach seems ineffective rather harmful as it almost increases rather than decreasing the risk of cancer and cardiovascular events or mortality rates. This paved way for other studies that probed into the antioxidant potential of other food components including vegetables, specifically polyphenols and their impact on hypertension. Such contradictory results led to the assessment of total antioxidant capacity (TAC) of different foods or whole diets rather than analyzing individual dietary antioxidant nutrient intakes. This is made possible by the use of two methods-hydrogen atom transfer (HAT) and single electron transfer (SET). The total radical-trapping ability parameter (TRAP) is a HAT assay for measuring dietary TAC. Having a clear picture of mean daily TAC intake would greatly help us in getting a clearer picture of how dietary modifications can reduce the risk of health conditions such as colorectal cancer, gastric cancer, myocardial infarction, stroke, type 2 diabetes risk and mortality rates. But sadly, we don’t have any studies showing a definite link between dietary TAC and hypertension risk. A French cohort study tried to analyze this relationship by studying 98,995 women aged 40-65 years. French Cohort Study The E3N French study mainly wanted to analyze the risk factors of cancer and chronic diseases. Hence, filled questionnaires on lifestyle and disease occurrence were sent by participants every 2-3 years. The response rate for every cycle was almost 83% and the loss in follow-up rate was 3%. The study started in 1990 and in 1993, 74,520 participants responded to a questionnaire that probed into the diet history of the participants. Many women including those consuming high proportions of energy, those suffering from cancer, hypertension or cardiovascular diseases before or during the 1993 questionnaire were excluding thereby leaving the study team with only 40,576 women. The self-administered diet history two-prat questionnaire contained 208 items. The first part probed into the consumption frequency and portion sizes of 66 food groups and frequency was measures based on 11 different categorizations-never or less than once a month; 1,2 or 3 times a month and 1 to 7 times a week. There was a photo booklet attached to the questionnaire to help in evaluating portion sizes. The second part of the questionnaire helped in segregating the 208 food items or beverages into respectable food groups. For every food item present in the questionnaire an equivalent food item was identified in the TAC database. Four food items (apple, melon, beer and vinegar) had more than 2 values and hence the average of the values was considered. For any food whose match couldn’t be found in the database a similar food that has the same vitamin C and E, polyphenol content and botanical group were measured. TRAP helped to measure the TAC of foods and the database showed that TRAP from coffee represented 75% of overall dietary TRAP, 6% for fruit, 5% for wine, 5% for tea, 4% for vegetables and 3% each for chocolate and other sources. Just because coffee dominated the list, the study team split the model into two: coffee-TRAP and non-coffee TRAP. In the non-coffee TRAP group, the providers were as follows: fruits (22%), wine (20%), tea (18%), vegetables (16%), chocolate (12%) and other sources (12%). Participants were questioned on their daily intake of different nutrients and energy intake was calculated accordingly. Physical activity performed in terms of walking, cycling, swimming and performing light or vigorous household chores were noted down in the questionnaire. Metabolic equivalents (MET) per week were noted down by multiplying yearly average METs for every item based on values from the Compendium of Physical Activities by the reported activity duration. Height, weight and BMI measurements were calculated and energy intake and total antioxidant capacity was estimated from the dietary questionnaire. Results After following up for almost 13 years and 4,93,895 person-years results showed that:
We do have other studies showing that increased intake of fruits and vegetables can reduce blood pressure in hypertensive and normotensive patients. In a study where the diet of hypertensive participants increased vegetable and fruits intake for the 6-month study period results showed a blood antioxidant capacity and decrease in systolic and diastolic blood pressure. But we do have studies showing that antioxidant supplements have no effect in improving hypertension levels. One study carried on for 5 years showed that blood pressure levels did not improve even after the participants were treated with a mix of vitamin C, vitamin E and beta-carotene versus placebo. Consuming fresh fruits and vegetables is an excellent way to improve antioxidant capacity. Choosing supplements prove to be ineffective. References High Dietary Total Antioxidant Capacity is Associated with a Reduced Risk of Hypertension in French Women: https://nutritionj.biomedcentral.com/articles/10.1186/s12937-019-0456-0 Antioxidant Supplementation in Hypertension: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4206049/ Diabetes mellitus remains very famous and prevalent across the world. People are advised to take a blood sugar test every once a while to check for their glucose levels and ensure that it is well within normal limits. This is usually done in a laboratory where the technician gives you the results in quite some time. But if you are a diabetic person who suffers from vagaries in blood glucose levels often you might be used to carrying a self-monitoring blood glucose (SMBG) kit that requires you to prick your finger every time for blood samples for measurement. We don’t like to prick ourselves every now and then which restricts us from measuring the values to anywhere between 2 and 4 times a day. Diabetes is a disease in which the pancreas cannot create enough insulin (type 1) or the insulin created is not effective (type 2) and the patient suffers from high glucose levels that can cause an array of physiological damages such as kidney failure, skin ulcers or bleeding into the vitreous of the eye. When such high are the stakes of diabetes it is not possible to allow the user to measure his/her glucose levels only 2-4 times a day between which the patient could enter hypoglycemic or hyperglycemic condition that can cause dangerous side effects. So, apart from taking measurements only at certain times of the day the individual might remain unaware of the rise and falls in blood glucose levels while using conventional methods of measurement.
Apart from using SMBG for monitoring some diabetes patients use a continuous analyte sensor that measures the concentration of a specific analyte (in this case, its glucose) in the body and sends our raw signals that is shown as an output value in the display. This output value is expressed in a form that’s meaningful to the user, such as glucose expression in mg/dL. So, it now becomes a continuous glucose monitor (CGM) and some of these monitors cautions the user with alerts and messages when there is a deviation in glucose values going into hypoglycemia or hyperglycemia. Though this sounds useful, there are many times during which the user starts ignoring the alarm or goes into ‘alert fatigue’ thereby disregarding the alert or turning it off without thinking about the consequences. For instance, after meals these devices might send out high glucose alerts. The user is already aware of the fact that glucose levels increase post-meals and hence, they tend to ignore these alerts or even turn off the alert option. Such measures can cause the user to miss out on further important alerts that come their way when glucose levels rise! There are problems with ‘low alerts’ too as the user might set a higher low alert threshold such that they get ample time to prepare for a severe hypoglycemic event. This might trigger frequent alerts of low blood glucose levels that are actually not severe enough to cause an event. Though the user expects an alert for severe lows the higher frequency of the alerts can cause the user to mistrust the device. The systems and methods patented here comes as a welcome change to the other ones mentioned here as it corrects all the flaws of these systems and alerts the user only when it makes sense to do so. The systems and methods designed here alerts the user only after ensuring that the user is not already aware of their condition-such as when they are in a diabetic state that needs attention. The systems and methods alert the user when action is necessary such as a bolus or temporal base rate change but do not alert in times when there is no action required such as when the user is already aware of the rise in glucose levels or when a corrective action was already taken to keep it under control. Here, the alert system is optimized to provide fewer alarms than usually given when the system is unaware of the user’s cognitive awareness. The monitoring device might be a smart phone, a tablet computer, a smart watch or a dedicated monitoring device. The system predicts the cognitive awareness of the user by identifying whether the user has previously taken some action (such as eating a meal, consuming required medications or exercising) when there was a suspected risk of changes in blood sugar levels without any prompting or a clue. In order to alert the user, the system might include determining a clinical value of a glucose concentration to predict future diabetes state. When the user is not cognitively aware of the diabetic state needing attention, the system might alert the user with a user prompt after a certain delay not based on time but based on the emergency of the diabetic state needing attention. The systems and methods described here provide ways to incorporate ‘smart alerts’ in analyte monitoring systems especially in continuous glucose monitoring systems. Once an alert is given the user might be requested to comment on the usefulness of the alert with buttons such as ‘Thank You’ and ‘Go Away’. The response from the user can in turn be used to predict future alerts for example, if an alert was provided two hours after a meal but was considered by the user as not being helpful the next alert could be given 2.5 hours after the meal. The user can also help to improve data efficiency-for instance, when a user would be performing a heavy working session he/she would be aware that their glucose would be outside normal ranges. Hence, the user can activate a setting on their monitor maybe click a button on the smartphone to activate a special ‘work out’ alert schedule. The patent was published on Nov 2nd, 2017 and for more information on the patent please visit: United States Patent & Treaty Office: http://patft.uspto.gov/netacgi/nph-Parser?Sect1=PTO2&Sect2=HITOFF&p=1&u=%2Fnetahtml%2FPTO%2Fsearch-bool.html&r=4&f=G&l=50&co1=AND&d=PTXT&s1=%22alerts+optimized%22&s2=Dexcom&OS=%22alerts+optimized%22+AND+Dexcom&RS=%22alerts+optimized%22+AND+Dexcom European Patent Office: https://worldwide.espacenet.com/publicationDetails/biblio?II=0&ND=3&adjacent=true&locale=en_EP&FT=D&date=20181221&CC=CN&NR=109069073A&KC=A World Intellectual Property Organization: https://patentscope.wipo.int/search/en/detail.jsf?docId=US205407982&_cid=P20-JZXWZO-24775-1 Nuts have a rich history of being one of the healthiest and tastiest foods available for human consumption. Numerous debates exist regarding their high calorie values and there are conflicting views on their effect on weight loss but beyond all such misconceptions nuts have surely sought a place for themselves in the ‘good’ food list for their valuable ‘good’ fat content (unsaturated fat). Though nuts mostly remind us of our very own cashew nut, almonds, pistachios and walnuts the latest favorites are the hazelnuts (HNs). I’m sure most of you would be familiar with this nut if not for the nut as a standalone food but as an important addition in Nutella alongside chocolate. There are many of those who were introduced to the healthy Hazelnut through the calorie-rich Nutella which is a chocolate-hazelnut spread. A study about cashews or almonds might be a repeat but there are many of those who are unaware of the goodness of this delicious ‘Hazelnut’.
Possible to Stay Unfazed by the Hazelnut? Nuts have been boasted of numerous health benefits right from reducing the risk of cardiovascular disease (CVD) to improving HDL (good) cholesterol levels. Hazelnut containing healthy fats, vitamin E, proteins and dietary fibers exists as the second most popular nut worldwide only next to almonds. Also known as filberts from European folklore the top three producers of this nut include Turkey, Italy and the United States of America. Almost 80% of hazelnut is comprised of monounsaturated fat with less than 4% composed of saturated fat. Any food that contains fat in such proportions helps in reducing total blood and ‘LDL’ cholesterol levels. While this makes HN a healthy snack it is used very frequently while manufacturing foods such as chocolate spread, nougat, cookie, cereal bar, pastry and ice creams. Apart from this, HN is also used as a prominent cooking oil or consumed raw, roasted, chopped, powered or processed into a praline paste. All the nuts have their own individuality and health benefits but hazelnut plays an extremely prominent role in promoting human nutrition as it has a combination of nutrients-macronutrients (lipids, fiber), micronutrients (minerals, vitamins), fat-soluble bioactives and phytochemicals (flavonoids). Let us look at each of the nutrients closely: Lipids & Fatty Acids Lipids form a greater part of the nut providing the kernel flavor that’s quite evident after roasting. This nutrient constitutes more than 60% of the kernel’s dry weight and is composed of 98% triacylglycerols (TAG). Oleic acid is the most prominent fatty acid present (76-82%) in the nut followed by linolenic acid, palmitic, stearic and vaccenic acid. HN also contains high levels of polyunsaturated fatty acids (PUFAs) and monounsaturated fatty acids (MUFAs) that are helpful in eliminating the risk of coronary heart disease by mending blood lipid levels and blood pressure levels keeping away metabolic syndrome and insulin sensitivity. Dietary Fiber Fiber is nothing but the roughage that’s resistant to small intestine digestion and requires microbiota fermentation that’s available in the large intestine. Almonds top the list (9%) in highest dietary fiber levels followed by HNs, walnuts, macadamia nuts and pistachios. A normal adult is recommended to eat 25 g/day of fiber for good health and for the prevention of problems such as colon cancer, heart disease and type 2 diabetes mellitus. Minerals Minerals might be macro or micro minerals that include calcium, sodium, magnesium, potassium, chlorine, phosphorus and sulfur as macro minerals. Micro minerals include iodine, zinc, selenium, iron, manganese, copper, chromium, bromine and molybdenum. While each of the minerals are important for different functionality selenium is the most important of all as it is required for the production of a class of protein which helps with important functions such as skeletal and cardiac muscle function, T-cell immunity, thyroid hormone metabolism and antioxidant defense. Tocols Tocopherols and tocotrienols are monophenols that are present in various nuts from macadamia to black walnut. HN oil contains high quantities of Vitamin E whose content depends on the geographic location of its growth. Peeling and roasting the nut also further removes tocopherol content to a greater extent. α- and γ-tocopherol are the most prevalent forms of isomers among which α-tocopherol contains high antioxidant activity. Vitamin E is also responsible for prevention of various diseases like cardiovascular, neurodegenerative, non-alcoholic fatty liver disease and certain kinds of cancer. Phytosterols and Phytostanols Plant sterols such as phytosterols and Phytostanols are eminently present in hazelnut. Phytosterols have the ability to reduce blood cholesterol levels by reducing low-density lipoprotein cholesterol (LDL-C) levels. These plant sterols do it by disabling cholesterol absorption at the intestinal level. The presence of phytosterols in diet decreases the chances of cancers such as colon, breast and prostate cancer. Phenols We need nutrients such as minerals, vitamins and fibers for good health but the fruits and veggies that we eat contain plant secondary metabolites called as polyphenols that play a vital role in designing human health. Compared to the raw form, roasting the nut releases more phenolic content that are critical for protecting individuals against cancer. Impact of Hazelnut Consumption on Blood Lipid Levels In general, almonds, walnuts, pecans and peanuts have been shown to reduce total serum cholesterol levels (TC) and LDL levels. When researchers tried to find whether hazelnut also had such potential benefits their research was rewarded with equally beneficial effects. When all nuts could be tried and tested for their effect on heart health the reason why researchers went behind hazelnut was because of their high MUFA composition, intense presence of bioactive substances such as tocopherols and phytosterols, selenium, caffeic acid, fibers, gallic acid and p-hydroxy benzoic acid that have anti-atherogenic effect by means of biological mechanisms that act on various pathways in CVD development. The study was conducted in accordance with PRISMA statement and the search included databases such as Medline and Google Scholar. Search criteria included various associated keywords, studies were eliminated based on various criteria and two authors reviewed each report independently. Weight, height, BMI, age and gender values were noted, the number of hazelnuts consumed per day, on the number of patients, on the number of supplementation days and on the type of control diet were all noted. Though the search came up with 779 papers only 385 of them were included for full-text review. After imposing selection criteria, the researchers were finally left with only 9 clinical trials for the study. A total of 425 individuals were involved of which 195 (46%) were males and 230 (54%) were females aged between 18 and 55 years. Of the 9 studies, 5 were randomized trials and the other 4 were non-randomized trials. Six studies had only healthy participants, 2 had hypercholesterolemic subjects and one study had subjects with type 2 diabetes. Apart from systemic review a Bayesian random effect meta-analyses was performed. Results showed that of the nine studies, only 4 showed a significant decrease in mean total serum cholesterol levels (TC) and LDL cholesterol levels. Four studies saw a significant increase in HDL cholesterol levels, two studies found a significant decrease in TG and one study reported an increase in TG. Of the 8 studies with BMI data six studies showed no difference, one study showed a decrease in weight and one study showed an increase in BMI and body weight. The Bayesian meta-analysis reported that hazelnut consumption showed beneficial effects on serum cholesterol levels, including hazelnut in diet routine was definitely better at lowering serum LDL cholesterol levels and total cholesterol levels with no major difference in HDL cholesterol levels. Such distinct advantageous effect on serum cholesterol levels could be due to the lipid content of hazelnut. All these are favorable for a positive effect on cardiovascular disease (CVD) prevention. Hazelnut as a Source of Micronutrient Hazelnut, as we know from above, is a key source of micronutrient and a study now has confirmed its beneficial effects on older adults. Older adults lead a systematic lifestyle consuming certain foods that’s possible for them to chew, digest and eat in limited quantities. Nuts inclusion is not evidently present in this age group largely but this study might be an eye opener for all such adults to consume nuts- a variety of them for added health benefits. A study included 32 people aged 55 and above who ate around 57 grams of hazelnuts (1/3rd cup) daily for 16 weeks. Results showed increased levels of magnesium and vitamin E (breakdown product of alpha tocopherol). The blood samples also showed decreased glucose and LDL levels besides increase in magnesium and vitamin E levels-two of the most under-consumed micronutrients in the US where the study was conducted-and also being a healthy source of copper, healthy fats and vitamin B6. We are all very much bothered about macronutrient intake, especially fats and carbohydrates (the third one being proteins) intake but don’t give much priority to micronutrient consumption. Such decreased micronutrient intake can lead to several health problems especially in older people who are at an increased risk of age-related conditions such as Alzheimer’s disease. Many take multivitamins to compensate for lost nutrients but eating hazelnut might be a multivitamin of its own as it has a combination of many of the nutrients that humans desire for good health. It’s good to know that hazelnut comes as a complete package with aplenty benefits but many individuals suffer from nut allergies and it is essential to ensure that you are not one of them! Also, when including nuts in dishes and shakes it is possible to overconsume them ignorant of the quantity. This can be dangerous as nuts are rich sources of calories and one must always be mindful of the quantity of nuts consumed anytime. Otherwise, it can lead to unnecessary weight gain. References Effects of Hazelnut Consumption on Blood Lipids & Body Weight: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5188407/ Hazelnuts as a Source of Bioactive Compounds & Health Value Underestimated Food: https://www.foodandnutritionjournal.org/volume7number1/hazelnuts-as-source-of-bioactive-compounds-and-a-health-value-underestimated-food/ Hazelnuts Improve Older Adults’ Micronutrient Levels, Study Shows: https://www.sciencedaily.com/releases/2018/12/181206135653.htm  Sleeping during the Day: Unusual for Others but a Daily Routine for Narcoleptics Sleeping during the Day: Unusual for Others but a Daily Routine for Narcoleptics History or Geography classes invoke sleep in most students, a post-lunch session by our professors is just like a lullaby song, office presentations sometimes transport us to a dream land and even while at work our eyes droop and we fall asleep for a minute or two in between. Such occurrences have happened in all of our lives sometime or the other and if in case you are one of those who hasn’t experienced it you must be a genius indeed. Sleep is a hobby for many, a passionate way to spend our time during weekends (getting up at 11 or 12 in the morning is not a rarity during holidays) and a relief from all the stress and anxiety we experience through the day. Sleep is an act that is dreaded by small kids, loved by teens and younger adults, wished for by middle-aged people and yearned for by older adults. The quality and duration of sleep decrease as we grow old in the case of most people. Are you one of those who goes to sleep as soon as you instantly hit the pillow? Of course, you are blessed! In this world where peace has become a rarity, happiness a commodity and good sleep a dream-come-true, getting to sleep in a matter of few minutes is never possible for most people-blame it on smartphones, television series or unending thoughts about life’s complications we keep staring at the ceiling or rolling back and forth in our beds wide awake without sleep. Amongst all this chaos, can you imagine that some people get to sleep during morning hours, while standing in a queue, while waiting for a bus or even in the middle of talking to someone about something important! Yes, these people are not blessed nor are they normal as they are characterized by a chronic debilitating sleep disorder narcolepsy, that’s characterized by excess daytime sleepiness, sleep paralysis, hallucinations and rarely by episodes of cataplexy (partial or total loss of muscle control occurring due to emotional triggers such as laughter, joke, surprise or anger). Narcolepsy Narcolepsy is a debilitating condition that ruins the quality of life of those individuals experiencing it. Occurring equally in both men and women it affects 1 in 2000 people as early as during childhood or adolescence but rarely diagnosed immediately. There is no definite boundary between awake and asleep state in these people which causes bouts of sleep in people while they are doing daily activities. Narcolepsy cataplexy (NC) is due to the absence of chemicals called hypocretin in the brain which is duly responsible for keeping us awake and regulating sleep-wake cycles. The cells responsible for producing the chemical is destroyed in narcolepsy and without this chemical the individual experiences troubles staying awake. NC is the muscle paralysis of REM sleep occurring during waking hours. REM Sleep Sleep has four phases of which the REM phase is the last one and the other three are non-REM phases. Rapid eye movement (REM) sleep typically happens some 90 minutes after you fall asleep with the first period lasting for about 10 minutes. Other successive stages last longer and the final one might last for as long as an hour. Most of our dreams occur in this stage of sleep and the brain becomes active. REM is critical to learning and memory as this is the time during which the brain processes information from our previous day storing what’s needed and discarding the rest. While non-REM stages occur early during the night it’s the REM stage that prolongs during the latter part of your sleep. Maybe that’s why we get up in the morning right out of a dream when woken up! Creativity and dreaming have always been interrelated to each other and we do have evidences supporting it-many people have reported scientific and artistic discoveries during dreams and one classic example is that of the periodic table of Mendeleev. Creativity ratio is linked to the number of dreams experiences and the complexity of the dream too. We have also had cases of finding solutions to problems in dreams when the individuals stored these problems in their brain right before falling asleep. There are studies supporting REM sleep’s advantage on anagram solving and creative problem solving and association between distant memories but their association with creativity isn’t proven completely. Are we saying here that naps and sleeps increase a person’s creativity? This is impractical and probably the development of creativity happens over the years over many sleep periods. So, when scientists wanted to examine the role of REM sleep over such long years their first pick was patients with narcolepsy as these individuals were often transported from wakefulness to a REM sleep termed as sleep onset in REM periods (SOREMs). These individuals experience frequent naps and more importantly, repeated periods of REM in comparison to normal individuals who rarely reach REM stage during their short naps. They remember their dreams better and also experience a greater number of dreams, lucid dreams that makes them excellent candidates for displaying versatile creative skills. So, a group of researchers tested upon the creative skills of people with narcolepsy to those of controls with the help of questionnaires and tests. Creativity-linked REM Study The study was carried out in two centers in Italy and France on individuals classified as suffering from narcolepsy based on different criteria. Each of them was categorized as suffering from type 1 or type 2 narcolepsy based on whether they had frank cataplexies and hypocretin-1 deficiency or not respectively. Though these participants had a brain MRI the results were normal as expected in patients suffering from this disorder. The team also picked 30 healthy controls from both countries who experienced no sleep disorders matched the sex, age and education of the participants. All the participants completed a formal test of creativity, a questionnaire asking questions on the participants’ sleep paralysis, hallucinations and presence of cataplexy, Epworth Sleepiness Scale and the Hospital Anxiety and Depression Rating scale. The participants filled 2 creative questionnaires that include the Test of Creative Profile (TCP) and the Creative Achievement Questionnaire (CAQ). TCP contained 57 yes/no questions that covered various types of creativity including innovation, imagination and researcher profiles. Each positive answer was normalized on a 100-point scale to come to conclusions. CAQ reports achievements across 10 domains including visual arts, music, dance, architectural design, creative writing, humor, inventions, scientific discovery, theatre/film and culinary arts whose scores were from 0 to 7 with 0 representing no expertise in the domain and 7 indicating tremendous expertise. The Evaluation of Potential Creativity (EPoC) is an objective test evaluating creative abilities containing 8 subsets assessing two models of creative thinking which includes divergent-exploratory thinking and convergent-integrative thinking. While participants were asked to generate multiple ideas based on a single stimulus in the former, they were asked to incorporate multiple elements to form a unique production (such as different characters to form a story) in the latter case. 10-15 minutes of time was given based on the task at hand and the total duration of the EPoC test was for 2.30 hours which included a 30-minute break which was used to sleep by 6 of the 30 subjects. Totally, 185 volunteers (71% had type 1 narcolepsy and 29% had narcolepsy type 2) participated in the study which included 118 from Paris and 67 from Bologna. 126 healthy controls were matched for age, sex and gender. Education levels were lower in the narcolepsy group compared to the control group. 30 subjects each from the narcolepsy and the control group who performed the EPoC test did not differ in age, gender and education while participants with narcolepsy experienced more frequent sleeps, higher levels of daytime sleepiness and depressive symptoms. Results showed that:
References Increased Creative Thinking in Narcolepsy: https://academic.oup.com/brain/article/142/7/1988/5506053 Narcolepsy: https://www.sleepfoundation.org/articles/narcolepsy George Church Ascribes his Visionary Ideas to Narcolepsy: https://www.statnews.com/2017/06/08/george-church-narcolepsy/ Extra leg space, extra-large dresses, extra cheese pizzas and extra seating space in aircrafts have become a normalcy these days. We can see a greater number of obese/overweight individuals compared to those with a normal weight. Eateries and restaurants selling buttery chicken wings and juicy cheeseburgers have only been rising in proportion. Humans today live in a world where leading life has become easier due to technological advancements and scientific discoveries, all of which have led to a greater increase in global inactivity. Such inactivity has paved way for more and more people to engage in a sedentary lifestyle that prevails as one of the biggest health problems in today’s world. That’s because, the body becomes weak due to continuous inactivity and this reduces the resistance to various diseases such as type 2 diabetes, obesity, hypertension and coronary heart disease. Time and again health experts have been insisting on the importance of physical activity to ensure leading a healthy and nutritious life but we don’t bother to pursue such advices to ensure well-being of our body until some disease or infection strikes us.
Cardiovascular disease is widespread worldwide and sadly, its not only the older generation but younger adults too who are becoming victims of this grave disease. Research shows that inactivity, rising obesity rates and lifestyle behaviors are serious threats to heart health and we do have positive research studies showing that cardiovascular risk factors greatly improve with heart-related changes that occur as a result of regular exercise sessions. Exercise is treated to be the nonpharmacological way of treating cardiovascular patients undergoing cardiac rehabilitation (CR) programs to improve their heart health and overall body fitness. Generally, all CR programs recommended heart patients to take up continuous moderate intensity aerobic training (CAT) such as walking and cycling as it is believed to reduce mortality rates, both cardia and other cause-mortalities. Generally, heart patients were always advised against performing strenuous exercise programs as it might be risky for the heart but of late, there have been more intense aerobic programs tested on cardiac patients that are proven to be safe and more effective than CAT in improving the patient’s overall cardiac outcomes. While aerobic training has been around for years, resistance training was not something that was a part of the exercise schedule of patients with heart conditions until the last two decades or so during which numerous advantages such as metabolic risk factors, functional capacity and psychological well-being were unraveled. Left Ventricle’s Prominent Place in Determining Heart Health Exercise training helps improving exercise capacity and cardiac output by increasing left ventricular functioning. There are studies that show that structural and functional changes in the left ventricle during exercise are prominently witnessed than changes in the other parts of the heart. Performing exercise elevates left ventricular stroke volume by increasing intrinsic cardiac contractility and improving left ventricular filling. The type of sport/exercise performed determines the framework adaptations in the left ventricle. Endurance training is one of the four types of exercises alongside strength, balance and flexibility that includes activities such as jogging, swimming, walking and cycling. Also known as aerobic training, practicing it regularly helps causing different changes in the structure and function of the heart and skeletal muscles. Resistance training helps in developing both left ventricular (LV) diastolic and systolic functions. Its been established that left ventricular training helps promote heart function but it would help further if we determine whether step-aerobic or core exercises help in improving left ventricular cardiac function development and also to minimize heart-related risk factors during middle age and beyond and the study below discusses this possibility. The study involved 45 healthy, sedentary women who were not involved in regular physical activity (more than 60 minutes a week), did not take any anti-pregnancy drugs, cigarettes or medications and were also devoid of diseases such as heart disease, respiratory, metabolic and inflammation disorders. Each of the participants were put into one of the two groups: step-up aerobic group (SAG) consisting of 25 participants and core exercise group (CEG) consisting of 20 participants. The study happened for four months and the exercise programs allocated for the two groups happened 4 days a week on all 16 weeks consecutively. Target heart rate (THR) was controlled using a heartbeat monitor and exercise intensity was also progressively increased every week from HR 60% to up to 70% (such as between 1st and 4th week it was HR 60%, between 5th and 8th week it was HR 65% and between 9th and 16th week it was HR 70%). Every exercise session happened for a full 60 minutes consisting of warm-up exercises (10 min), primary exercises (30-40 min, basic movements step-aerobic) and cool down exercises (10 min) in the case of SAG and for CEG warm up and cool down remained the same while primary exercises practiced for 40 minutes composed of core exercises that help in building more strength for lower and upper extremities that includes 3 sets/day, 10 repetitions/set with 1-2 minutes resting interval. Height and weight measurements were taken, BMI readings were calculated, waist circumference, hip circumference and waist-to-hip ratio were also measured. BP measurements were taken and blood samples were taken in the morning after an overnight fast before and after the study. Two-dimensional echocardiography was performed before and after the 16-week study period, and variables such as LV end-diastolic dimension (LVDD), end-systolic dimension (LVSD), interventricular septum thickness (IVS), left ventricular posterior wall (LVPW) MDT-mitral deceleration time, left ventricular ejection fraction (LVEF) and left ventricular fractional shortening (LVFS) were measured. Results showed that:
Improving Left Ventricular Systolic & Diastolic Function in Adolescents with Type 1 Diabetes Diabetes is one of the biggest public health problems that’s been attacking humanity inconsolably and the best means to curb this epidemic is to eat nutritious diets and exercise regularly. But what we lack is enough knowledge on whether exercise improves cardiac hemodynamics in adolescents with type 1 diabetes. Researchers have tried to analyze left ventricular volume at rest and also during exercise in individuals with type 1 diabetes compared to those without diabetes before and after a 20-week exercise training program. Adolescents aged between 14 and 18 years who were free of problems such as hypertension, neuropathy, retinopathy or microalbuminuria and suffered only from diabetes were involved in the study. 38 (20 males) participants with diabetes and 22 control participants were involved in the study. BMI, body composition, height, weight and abdominal obesity were measured. Exercise sessions lasted for 60 minutes each four times a week over a 20-week period. Exercises were modified to achieve 85% of the participant’s heart rate. During the 1st-12th week participants performed three days of aerobic exercises and one day of resistance training whereas from weeks 12-20 all of them were involved in 4 sessions of combined aerobic and resistance training. During the study period three participants dropped due to time commitments and finally only 72 participants remained: 37 of them with type 1 diabetes in exercise training group, 13 of them with type 1 diabetes in the control group and 22 adolescents without diabetes in the exercise training group. Though both groups with diabetes increased total body weight it was more of fat-free mass compared to the control group with type 1 diabetes that gained weight due to fat deposition. The exercise sessions had a positive impact on body composition and helped in reducing percentage body fat and increasing fat free mass and bone mineral density. Exercise training had no impact on the resting and maximal exercise systolic, diastolic and mean arterial pressure but there was an increase in arterial pressure in the control group with type 1 diabetes after 20 weeks. The study showed that exercise improved the left ventricular function of both training groups at rest and also the submaximal exercise cardiac output, stroke volume, end-diastolic volume and ejection fraction. While improvements were witnessed in both training groups maximal effects were seen in the group with diabetes. Also, left ventricular filling and contractility improved after exercise training in adolescents with diabetes proving that exercise helps in preventing/postponing left ventricular function impairment in those patients with diabetes. Hence, this study clearly shows that regular practice of exercise over a period of 20 weeks was associated with improvements in left ventricular function. In trained teens with diabetes the results were similar to that achieved in untrained controls without diabetes. References The Effect of Exercises on Left Ventricular Systolic & Diastolic Heart Function in Sedentary Women: https://www.sciencedirect.com/science/article/pii/S1728869X17300953 Exercise Training Improves but does not Normalize Left Ventricular Systolic & Diastolic Function in Adolescents with Type 1 Diabetes: https://care.diabetesjournals.org/content/40/9/1264  A Diet Rich in Fiber is Good for Health Irrespective of Whether or Not it Has Impact on Cancer Risk A Diet Rich in Fiber is Good for Health Irrespective of Whether or Not it Has Impact on Cancer Risk Ovarian cancer prevails as the leading cause of death (1,50,000 deaths annually) in gynecological cancers worldwide and is the second most common female reproductive malignant tumor (240,000 cases erupt every year). Awareness about ovarian cancer has increased tremendously during recent times but still we lack the knowledge to get it diagnosed at an early stage. This disease often remains undiagnosed until later stages by which time it has 100% chances of spreading to the abdominal cavity. We boast of scientific advancements and research in the field of ovarian cancer in the past few decades but still lack a definite prognosis that could help treat patients in their early stages of ovarian cancer despite advances in treatment options. Though the cancer generally affects women who have been through menopause (mostly above the age of 50) there are chances of it affecting younger women too. While the exact causes of ovarian cancer remain unknown, we do know that age (above 50 years), family history of breast or ovarian cancer, endometriosis and being overweight are serious risk factors. We do have data supportive of the fact that dietary factors such as glycemic load, dietary phytoestrogen, fat, fruits and vegetables do play a role in impacting ovarian cancer risk. Fruits, vegetables and whole grains are excellent sources of fiber, a nutrient that has been inversely linked to the risk of several types of cancers such as colorectal, endometrial, gastric and ovarian cancer. But the role of diet, especially fiber has been greatly conflicting providing us with inconsistent results that prevent us from either supporting or denying the role played by fiber in affecting the risk of ovarian cancer. Some studies supported the fact that intake of dietary fiber was inversely proportional to ovarian cancer risk but some others failed to prove the connection and moreover, the effects varied depending on the type and source of fiber consumed. Systematic Review of Ovarian Cancer Risk The Women’s Health Initiative (WHI), a trial consisting of 48,835 postmenopausal women was the only primary prevention intervention trial that proved that eating a low-fat diet reduced the risk of ovarian cancer risk by 40%. But we do have descriptive data going as early as 1975 showing that there could be an association between dietary fat and ovarian cancer risk. There were also several results supporting that while veggies, whole grains and low-fat milk reduced ovarian cancer risk, meat intake increased the risk but still we did not get any conclusive results. To compare all the different study results and come to certain conclusions a systematic review following the recommendations of Preferred Reporting Items for Systematic Reviews & Meta-analysis Approach (PRISMA) with the help of search engines such as PubMed, MEDLINE, etc. were conducted and finally, 24 publications that met the inclusion criteria were included in the review. Many reviews supported that increased fat intake increased ovarian cancer risk while vegetables consumption decreased the risk significantly. A Canadian study tried looking into the perspective that fiber intake reduced the risk of ovarian cancer significantly but neither total fiber nor specific fiber types showed a significantly lower risk for ovarian cancer. The review clearly concluded that fiber did not have any impact on ovarian cancer risk in any way. Meta-analysis of Observational Studies Owing to inconclusive evidences in relation to the risk of ovarian cancer risk and fiber intake, two investigators searched databases such as PubMed and Web of Science using several word search criteria and inclusion criteria. They were left with 2784 publications that had a link between fiber intake and ovarian cancer risk. But it was only 17 studies that met the inclusion criteria of which four of them were cohort studies and the remaining 13 were case-controlled studies-10 of them were from United States, four from Europe and three from Asia. Results showed that:
Another meta-analysis followed the standard MOOSE and PRISMA to report the analysis and used databases such as PubMed and EMBASE to sort through the studies. Two investigators were involved here too who used specific search terms to narrow down study inclusions and finally were rewarded with 4665 articles of which 4641 were excluded as they did not meet the study criteria. Again 11 of them were excluded due to several criteria leaving the researchers with only 13 of them that contained 5,777 ovarian cancer cases and 1,42,189 participants. Of the 13 studies, 10 of them were case-controlled and 3 were cohort studies all of which measured dietary intake with the help of a food-frequency questionnaire. Results showed that:
Earlier identification of ovarian cancer paves way for better treatment and curing chances. But often we don’t recognize ovarian cancer until it has already spread. Even if treatment is successful there are greater chances that the cancer might recur in a few years’ time and in this case, there is no cure. It can only be controlled with the help of chemotherapy which can help in extending the patient’s life by several months or years. Hence, prevention is better than cure. While family history or age factor is not in our hands, we can do as much as we can to reduce the risk when it comes to dietary modifications and lifestyle factors. Results of fiber, vegetable and fruit intake and their association in reducing the risk of ovarian cancer might be inconclusive but we are sure that these foods are indeed good for our health and there is no harm in eating them. Consuming the right kind of foods, staying on a normal body weight and exercising regularly helps reduce the risk of ovarian cancer greatly. References Dietary Intake & Ovarian Cancer Risk: A Systematic Review: https://cebp.aacrjournals.org/content/23/2/255# Association between Dietary Fiber Intake & Risk of Ovarian Cancer: A Meta-analysis of Observational Studies: https://www.researchgate.net/publication/327215865_Association_between_dietary_fiber_intake_and_risk_of_ovarian_cancer_a_meta-analysis_of_observational_studies Dietary Fiber Intake & Reduced Risk of Ovarian Cancer: https://nutritionj.biomedcentral.com/articles/10.1186/s12937-018-0407-1 Heart, kidneys and liver are the ones that come to our mind at the mention of the word ’organ’. While the skin is present all over our body how many of you are aware that the skin is an organ let alone the fact that it is the largest organ in the human body. Each of us are blessed with a different skin type which doesn’t only include skin color but also its texture and a vast array of microorganisms that reside on it. These microbes don’t stay on the skin forever as the skin renews itself occasionally thereby shedding away these organisms. While most of them are not harmful, some of them are even beneficial helping in secreting antibacterial substances or preventing pathogen colonization and some others harmful causing diseases and infections. We do know that a newborn’s gastrointestinal tract contains millions of microbes that are initially acquired from the mother through breastfeeding and also environmental exposure and the same is true in the case of skin’s microbiome too. Once the initial colonization is complete, the microbiome composition keeps varying in response to factors intrinsic and extrinsic to the host. The host of microbiomes present varies from individual to individual and also from location to location on the individual.
Probiotics and prebiotics are dominating the nutrition world right now for their good health. Probiotics are good microorganisms that are ingested by an individual to enable a healthy GI tract while prebiotics are ingredients that support the growth of these good microorganisms. Dietary requirements of microorganisms vary between species and an agent that exhibits prebiotic activity on a particular microorganism might not exhibit the same prebiotic effect on another one. We are in an advanced world where lifespan is rapidly growing and people are living well beyond 65 years. More than 566 million people are above the age of 65 presently and the population is estimated to be 1.5 billion by 2050. But within these individuals’ life duration they are expected to witness increased hospital times and repeated exposure to antibiotics. Infections are responsible for a third of the mortality rates in elderly population and this can be attributed to changes in immune system that become less effective in handling microbial infections. The microbiome of a person’s skin comes of use here as altering it and enhancing the good bacteria content has the potential to avoid infection, reduce their presence and effect. So, enhancing the health of an individual’s skin becomes a priority now and the invention in this patent provides a method for doing exactly the same. The invention here aims at using bacteria that are modified to enhance characteristics that we believe are advantageous for the skin microbiome and health of the individual which includes bacteria that have been modified using a CRISPR-Cas9 and/or Cpf1 system. Rather than altering the human genome the invention here tries to modify the skin microbiome to enhance health. The invention might include a method for altering the skin’s microbiome by administering an effective amount of bacterial formulation on the skin of the individual. For instance, if the subject is a newform the formulation which might be an ointment, lotion or gel is rubbed onto the newborn’s skin within 6 hours of birth to address certain concerns in the newborn. The bacteria added in the formulation depend on the diseases or concerns that are addressed. The formulation might be applied within 24 hours of birth, within 6 hours of birth, within 3 hours of birth or within even an hour of birth even in the form of a spray or mist. It depends on the mother to choose for her baby-either rely on chances to the presence of critical microbes that form the immune system or use a predetermined formulation that contains a specific combination of microbes which help the newborn’s immune system to react to the microbes in the predetermined formulation helping the baby get equipped with a more variant immune tolerance profile. A specific aspect of this invention relates to the treatment of acne-a common skin problem that accounts for a quarter of dermatologists’ patient volume. Acne has a tremendous impact on the person’s quality of life upsetting his/her emotional as well as social well-being. Bacteria selected in the formulation help relieve acne problem when applied onto the individual’s skin and these are generally ammonia oxidizing bacteria. The invention is also directed at incorporating bacteria into various skin-care products, deodorants, sunscreens, fragrances and those for oral or dental hygiene and hair care products. Generally, we use anti-bacterial agents to kill bacteria which also kills useful bacteria on the person’s skin in this process. But the present invention aims at intentionally exposing the skin to microbes (good bacteria) to treat skin infections, diaper rash and urinary/vaginal infections. All gram-negative bacteria are disease producing and one aspect of this invention is aimed at reducing the number of gram-negative bacteria on a person’s skin by adjusting the overall pH of the skin tissue region. We do joke that mosquitoes love certain people’s skins and this invention has proved it. In one embodiment the bacteria are modified to express certain compounds that deter mosquitoes from contacting human skin. The present invention plays a key role in our daily lives helping us enhance our quality of life by enhancing skin health. The patent was published on May 4th, 2017 and for more details on this invention please visit the following sites: Unites States Patent & Trademark Office: http://patft.uspto.gov/netacgi/nph-Parser?Sect1=PTO2&Sect2=HITOFF&u=%2Fnetahtml%2FPTO%2Fsearch-adv.htm&r=114&f=G&l=50&d=PTXT&p=3&S1=((health+AND+exercise)+AND+fitness)&OS=health+AND+exercise+AND+fitness&RS=((health+AND+exercise)+AND+fitness) World Intellectual Property Organization: https://patentscope.wipo.int/search/en/detail.jsf?docId=US195462458&_cid=P10-JYH7PR-65448-1  Neuropathy Signs are Verified Using Pinprick or Even Temperature Control Neuropathy Signs are Verified Using Pinprick or Even Temperature Control There are millions of people affected by diabetes, millions affected by hypertension and also million others who have a combination of diabetes and hypertension leading their lives. Hypertension is a comorbid condition very commonly seen in up to 75% diabetic patients depending on their obesity, age and lifestyle. It usually presents as a metabolic syndrome of insulin resistance that includes central obesity and dyslipidemia as well. Such comorbid presence of hypertension increases the risk of microvascular and macrovascular complications. Macrovascular complications include coronary artery disease, myocardial infarction, stroke, congestive heart failure and peripheral vascular disease and microvascular complications generally include retinopathy, nephropathy and neuropathy. Microvascular conditions are generally linked to hyperglycemia but hypertension too is a valuable risk factor for these conditions. Diabetic Peripheral Neuropathy (DPN) Diabetic Peripheral Neuropathy (DPN) is damage to nerves that sit near the skin and is a very common effect of diabetes that almost 50% people with type 2 diabetes and 20% people with type 1 diabetes suffer from it! It is most commonly nerve damage (to two types of nerves) caused to the hands and feet. While researchers still question how diabetes kills nerve cells, they have come up with other important causes such as high cholesterol, obesity and high blood pressure as major contributing factors. A British report in a study conducted more than a decade back on 37,000 people with type 2 diabetes for almost 9 years showed that high blood pressure increased risk of neuropathy by 11-65% in these participants. The explanation given here is that metabolic changes due to diabetes increases number of free radicals that attack cell DNA thereby killing antioxidant compounds that help in protecting the cell from free radicals and inflammation. Also, the nerve fibers rely on blood vessels for nutrients and oxygen supply and high blood sugar/blood pressure levels damage these blood vessels preventing any supply to the nerve fibers. DPN affects almost 70% people with diabetes and exists as the leading cause of foot amputation. It usually is the result of prolonged diabetes in individuals and is associated with metabolic derangements such as increased polyol flux, accumulation of advanced glycosylation end products, lipid derangements and oxidative stress. Extremely stringent measures to control blood sugar levels is recommended for controlling DPN but this also only helps in preventing progress of the disease in type 1 diabetes mellitus (T1DM) patients but shows no benefits in individuals with type 2 diabetes mellitus (T2DM). There are numerous clinical and experimental studies showing that hypertension exists as an independent risk factor for DPN in patients with T1DM or T2DM. Hypertension mostly affects the myelinated fibers and studies in hypertensive rats with diabetes show a reduction in sciatic nerve blood flow along with a reduction in motor and sensory nerve conduction velocity and myelinated fiber density but no loss of intraepidermal nerve fibers. In a hypertensive T2DM model a reduction in sensory nerve conduction velocity and increased matrix metalloproteinase was witnessed at sites of myelin thinning. In nondiabetic rats affected by hypertension impaired epineural arteriolar function led to reduced endoneurial perfusion and neuropathy. But a combination drug helped in preventing and reversing nerve conduction and nerve abnormalities in type 2 diabetes rats. Elaborated below is a detailed study helpful in exactly identifying the impact of hypertension on both large and small fiber measures of DPN in patients with T1DM. Effect of Blood Pressure on Type 1 Diabetes Patients with Neuropathy Participants with T1DM and controls without diabetes were chosen based on multiple exclusion criteria which included hypothyroidism, corneal surgery in the last 6 months or so, vitamin B12 deficiency, neuropathy from nondiabetic causes, corneal trauma and diabetes or impaired glucose tolerance in the control group. BP measurements were taken in sitting position after a rest period of 5 minutes on 2 occasions. Systolic blood pressure readings ≥140 mm Hg or subjects on antihypertensive treatment were defined as suffering from Hypertension. Each of the participants were measured for their body mass index (BMI), glycated hemoglobin (HbA1c), cholesterol and triglycerides. Each of the participants were declared to be suffering from DPN or not based on certain criteria such as neuropathy symptoms or neuropathy signs and an abnormality of NCS or some known measure of small fiber neuropathy. Neuropathy symptoms included unsteadiness in walking, neuropathic pain, paresthesia and numbness each of which was given scores up to 4. A score ≥1 indicated the presence of a neuropathic symptom. The signs of neuropathy were verified using a pinprick on the tip of the large toe, temperature perceptions in the dorsum of the feet and the presence or absence of ankle reflexes. Any score >2 of 10 was confirmed to be a sign of neuropathy. Corneal confocal microscopic images from the subbasal nerve plexus in the central cornea was noted for each eye. Corneal nerve fiber density (CNFD) and length of nerve fibers (CNFL) were measured. Skin biopsy was taken and cardiac autonomic neuropathy was evaluated. Assessment of Sural sensory nerve action potential (SNAP), sural nerve conduction velocity (SNCV), tibial compound motor action potential (TCMAP), tibial motor nerve conduction velocity (TMNCV), peroneal compound motor action potential (PCMAP) and peroneal motor nerve conduction velocity (PMNCV) was done in the right lower limb by a consultant neurophysiologist. On the whole, 58 normotensive controls, 20 hypertensive controls, 30 normotensive and 40 hypertensive T1DM participants were involved. Systolic and diastolic blood pressure were comparably higher in the hypertensive compared to the normotensive groups. While hypertensive controls exhibited higher blood cholesterol levels compared to normotension controls values of HbA1c, triglycerides and BMI were comparable. Hypertensive T1DM participants expressed higher triglycerides and BMI compared to normotensive T1DM participants but HbA1c and cholesterol were comparable. Results showed that:
In another study on 467 participants aged between 45 and 64 done by the University of Toronto in 2015 almost half of those with prediabetes or newly diagnosed type 2 diabetes showed early signs of peripheral neuropathy. Higher the blood sugar levels likelier are the chances of nerve damage. Diagnosis of patients with type 1 diabetes usually happens at an early stage and about 20% of them have peripheral neuropathy after 20 years. While age does seem to be a contributing factor for people with DPN there are cases of even small kids and young adults with type 1 and type 2 diabetes who show signs of peripheral neuropathy. Also, nerve damage is irreparable causing great loss in the ability to feel and move irrespective of however the nerves could get damaged. Damage Control You might suffer from any form of diabetes but if you don’t have nerve damage it is highly possible to avoid suffering from neuropathy if you control blood sugar levels and pursue other healthy steps. If you suffer from T1DM tight glucose control can eliminate DPN risk by 78% while for those with T2DM it reduces the risk by 5-9%. This vast variation in risk control might be due to the diagnosis stage. T1DM is usually diagnosed earlier preventing most nerve damages while T2DM patients might lead a life with the disease for years together before diagnosis. Such prolonged existence of T2DM without medications and sugar level control leads to nerve damage even from the prediabetes stage and this indicates ample irreparable nerve damage that is caused before a diagnosis is made. There is nothing that can be done about nerve damage that has already happened but we can prevent further damage by taking good care of our health. References Hypertension Contributes to Neuropathy in Patients with Type 1 Diabetes: https://academic.oup.com/ajh/article/32/8/796/5477297 The Comorbidities of Diabetes and Hypertension: Mechanisms and Approach to Target Organ Protection: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3746062/ Diabetic Neuropathy: Causes and Symptoms: https://www.endocrineweb.com/guides/diabetic-neuropathy/diabetic-neuropathy-causes Treatment of Hypertension in Adults with Diabetes: https://care.diabetesjournals.org/content/26/suppl_1/s80  It's Ok to Occasionally Indulge in a Cheat Meal which Keeps You Bonded & High Spirited It's Ok to Occasionally Indulge in a Cheat Meal which Keeps You Bonded & High Spirited Human mind is like a monkey that cannot help but keep jumping from one thing to another. Many times, our hearts rule our brains and we take decisions based on our interests and pleasures rather than focusing on goals and needs. Food occupies a major role in our lives and we face debilitating health consequences owing to the wrong types of foods that we choose to eat. Given a choice between French fries and salads most would pick French fries. Choices spoil us unless they are all good ones that promote health! Obesity in adults and kids is a worldwide epidemic and exists as one of the most important problems worldwide. Obesity in childhood heightens the risk of health problems in adulthood, even more in kids who have obese parents. We have more than 45 million children who are obese worldwide and there is a dire need to stop this obesity epidemic immediately. There have been multiple steps taken and strategies implemented to reduce weight gain but all of them have been from an individual perspective. Children are children and such approaches might result in weight loss but this is only temporary and for a short-term as they once again go back to their earlier eating routines and practices after some time. This is mainly due to the fact that our environment has now become one that promotes consumption of high-energy foods and sedentary behavior. We would define such an environment as an ‘obesogenic’ environment-in simple terms, its an environment that encourages people to eat unhealthy food and not do enough exercise, promotes sedentary behavior and contributes to everything that increases obesity risk. Individuals interact with the environment in different levels-homes, schools, neighborhoods and friends-and the fact is that, we don’t have much control over things that happen in the environment. Childhood obesity is the sum total of genetics, environment and behavioral response. Genetics is not in our hands and certain environmental factors too cannot be controlled but we can focus on changing the ones that can be influenced and also finetune behavioral response-for instance, the child’s eating behavior and family environment does affect obesity and this can be handled internally. Recently, there have been serious steps taken to alter ‘obesogenic’ behaviors and obesity development such as by modifying environmental factors. Environmental factors operate at micro (home, school, neighborhood) and macro (government, health system, food industry) levels. While macro environmental factors are not flexible to change, we can do bring about changes to the family food environment (FFE) that also seems to be the greatest contributor of obesity when compared to school and neighborhood. FFE also affect the eating behaviors of the kid greatly. When parents control eating habits of children it has been associated with increased body weight in kids and has also increased their inclination towards obesogenic eating behaviors. Even watching television and availability of fruits/veggies at home increase obesogenic eating behaviors in kids leading to overweight issues. Family Food Environment FFE is not something new and there are numerous FFE variables such as frequency of family meals, parental feeding strategies, viewing TV/electronic gadgets while having meals, parent’s food and nutrient beliefs, parent’s cooking and shopping skills and parent’s nutrition knowledge that have been analyzed individually for their impact on obesogenic eating behavior but we don’t have results on the collective impact of these variables. We also don’t have data on the impact caused by psycho-social factors such as income, parent’s marital status, depression status or parent’s BMI on FFE variables. An Australian study aimed at using factor analysis to derive composition of FFE variables and their effect in obesity and obesogenic eating behaviors. Also, the impact of psycho-social factors on FFE variables is dealt with. Australian parents of children aged 2-5 years were included in the study based on an advertisement posted on the social media platform Facebook. All the participants were recommended to calculate height and weight measures of themselves and their kids using household measures such as bathroom scales or tapes. Children’s eating behavior was measured using sub-scales of the Children’s Eating Behavior Questionnaire (CEBQ that focused on enjoyment of food, food responsiveness, satiety responsiveness, food fussiness and slowness in eating). The 8 Feeding Practice and Structure Questionnaire (FPSQ-28) included Reward for Behavior (4 items), Reward for Eating (4 items), Persuasive feeding (6 items), Covert Restriction (4 items), Overt Restriction (4 items), Structured Meal Setting (3 items), Structured Meal Timing (3 items) and Family Meal (single item). Family meal frequency was measured based on three items including breakfast, lunch and dinner, general nutrition knowledge score was created based on a general knowledge questionnaire and four nutrition belief items (Eating healthy is expensive, It takes too long to prepare a healthy meal, Healthy food doesn’t taste good and Nutrition is important to your family’) were also measured apart from measurements on parental stress, anxiety, cooking and shopping skills. A total of 977 participants were fetched of which 7.6% of them were underweight. The aim of the study was to reflect upon the impact of FFE variables on obesity and hence underweight children were excluded from the study leaving just 757 participants who were parents of children aged between 2 and 5 years. Results showed that:
Imposing SEM Concept on Obesogenic Behavior Another study aimed at introducing an integrated model based on three basic concepts (parental socioeconomic status, parental feeding behavior and child’s food intake) within the Structured Equation Modeling (SEM) framework. In order to figure out the major factors involved in determining childhood obesity relationship among child technology use, child’s average amount of sleep, child’s school grade, child’s physical activity, parent’s physical activity and the child’s weight was noted. Parental socioeconomic status was measured based on six indicators that included the mom’s education, dad’s education, mother’s income, father’s income, mother’s work experience and father’s work experience. The last was ‘How long have the parents been married?’ Parental feeding behavior that included restricting, monitoring, rewarding, pressurizing, controlling and modeling was measured on a 5-point scale with higher scores indicating a more frequent use of a specific feeding behavior. Child’s food intake was measured based on seven indicators including consumption of fruits, vegetables, whole grain products, sweets, chips, soft drinks and fast food where parents indicated on a six-point scale (never, seldom, sometimes, most of the time, always and several times a day) how often their kids ate certain foods. Control variables were measured: Parental physical activity was measured by categorizing parents into four categories based on their answers: none, 1 or 2 times a week, 3 or 4 times a week and more than 4 times a week. The kid’s average number of sleeping hours was categorized into ‘less than 7 h per day’, ‘7 to 8 h per day’, ‘8 to 9 h per day’ and ‘more than 9 h per day’. The child’s screen time was categorized into ‘less than an hour every day’, ‘1 to 2 h per day’, ‘3 to 4 h per day’ and ‘more than 4 h per day’. Child’s physical activity was sorted into ‘1 to 2 times per week’, ‘3 or 4 times per week’ and ‘more than 4 times per week’. BMI of 402 observers was in the normal range and 147 observers was overweight or obese. The study presents two structured models: one based on the normal BMI range (normal model) and one based on obesity BMI range (obesity model). Results showed that:
References Family food environment factors associated with obesity outcomes in early childhood: https://bmcobes.biomedcentral.com/articles/10.1186/s40608-019-0241-9 Family environment & childhood obesity: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5334735/ |
AVOID FRAUD. EAT SMART+91 7846 800 800
|
- Home
- Written Testimonials
- Consult
- Clinics
- Blogs
-
Diet & Nutrition
- Diabetes Reversal
- IVF IUI not needed for PCOS PCOD Infertility
-
Medical Nutrition
>
-
Disease & Conditions
>
- Infertility | PCOS
- Diabetes Mellitus
- Cholesterol
- Hypothyroid
- Kidney Problems
- Hypertension
- Cardiovascular Diseases
- Liver Diseases
- Gastro intestinal disorder
- Cancer
- Metabolic Disorders
- Orthopedic Disorders
- Eating Disorders
- Dietary Recall
- Weight Record Filled By Clients
- Online Payment Transaction Details
- Online Clients Weight Check Form
- Our Program Package Service Charges
- Weight Record 2017 Clients
- Measurements sent by Clients
- Terms & Conditions Of Payment
- Thanks. Your Form is Submitted
- Video Testimonials
- Lifestyle & Wellness
- Lifestyle & Wellness Blog
- Allergy & Intolerance
- Weight Loss / Gain
- Weight Loss / Slimming Blog
-
Disease & Conditions
>
- Life Cycle Nutrition >
- Sports Nutrition >
- Integrity in Nutrition
- Knowledge Centre
© COPYRIGHT 2022. ALL RIGHTS RESERVED. FRST HEALTHCARE PVT LTD.
Dr. Nafeesa Imteyaz of First Eat Right clinic, is the Best Dietitian Nutritionist in Bangalore. Best Dietitian Nutritionist in Pune. Best Dietitian Nutritionist in Hyderabad. Best Dietitian Nutritionist in Chennai. Best Dietitian Nutritionist in Mumbai. Best Dietitian Nutritionist in Delhi. Best Dietitian Nutritionist in Kolkata.