|
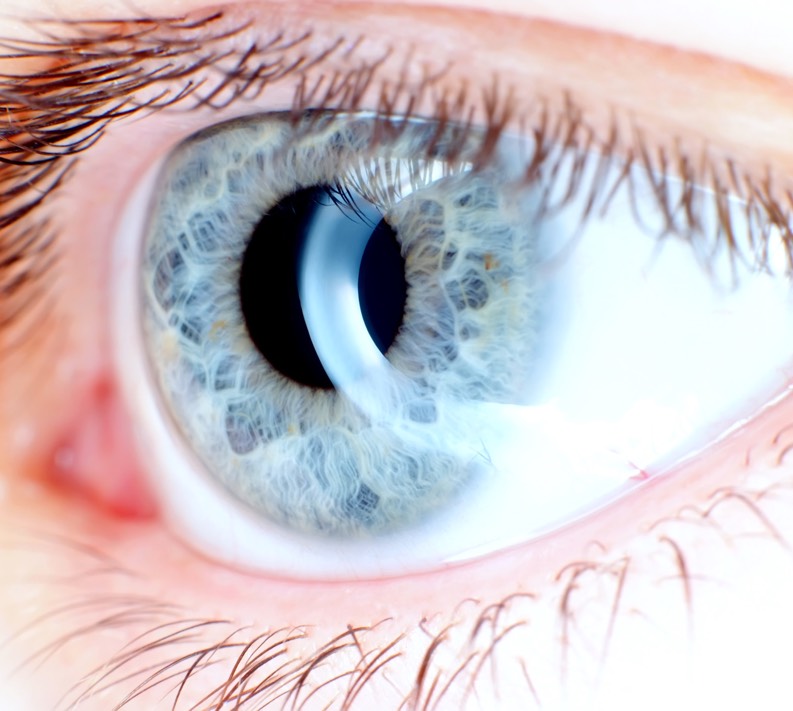
The shopping list is ready and you are at the supermarket to pick and choose the essentials for the month. Though you might be doing it on a weekend there isn’t much leisure time to shop at your desired pace. In such situations, it would be extremely helpful if the nutrition labels present in the pack is color-coded for quicker understanding, isn’t it? Nutrition labels on food products help us choose between various products and restrict our consumption of foods that’s high in fats, sugars and salt. The information provided is for 100 grams or per portion of the food and nowadays, due to increased interest in choosing healthier food options food manufacturers are highlighting fat, salt, sugar and energy content on the front of the packaging along with reference intake values. Some of these nutrition labels use colour codes such as red, amber and green and this helps us decode the fat, salt and sugar content of the food in a glance.
This color-coded labelling is also called as ‘traffic light’ labelling that has been proposed as a public health intervention to minimize obesity risk by attending to the dietary intake of individuals. These occur as a part of the front-of-pack (FOP) nutrition rating systems that clearly detail the calories and nutrients present within the food pack. We already have studies that have given a green signal to traffic light food labelling as an excellent initiative to fight against obesity and a modelling study in Australia found it to be a cost-effective method for preventing obesity. Studies of summary indicator FOP systems show that this system is in fact efficient enough to promote healthier product reformulations by manufacturers-this was seen in Canadian manufacturers where they successfully reduced sodium in foods by 80-150 grams. There are different studies that show that sodium, fat and sugar consumption could be reduced if individuals replaced their regular foods with those that follow the FOP system criteria. Canadian Study on Replacing ‘Red’ Label Foods with Healthier Options: A Nutrition Analysis Fat, energy, sodium and sugar intake of Canadian adults were calculated using data from the Canadian Community Health Survey, Cycle 2.2 Nutrition (CCHS 2.2)- a national survey that’s aimed at providing authentic data regarding food and nutrients intake of Canadians. The CCHS 2.2 included a sample of 35,107 individuals aged 0 years and above whose food and nutrients intake was calculated through a 24-hour dietary recall. The present research primary included Canadian adults aged 19 years and above, excluded pregnant and breastfeeding women and also those whose food intake data was not available. The different foods consumed by individuals were color-coded in red, amber or green depending on the criteria for food and drinks described in the UK’s ‘Guide to Creating a Front of Pack (FoP) Nutrition Label for Pre-packaged Products Sold Through Retail Outlets’. This was used as the measure to compare against the fat, sodium and sugar intake of foods and drinks. Those foods that had red color codes were replaced with similar foods that did not have the code for any of the nutrients. Whenever possible, the original food was replaced by the same food from a different brand that provided a healthier option and every effort was taken to ensure that the replaced food was as good as the original choice. For instance, lean ground beef was replaced with extra lean ground beef. There were also instances where some foods were replaced by the same foods but prepared in a much more nutritious manner. But when replacement was not possible the foods were not replaced. Results Totally, Canadian adults consumed 5655 unique foods and 495 unique beverages and it was found that 52% foods and 13% beverages contained at least one nutrient that qualified for a red traffic light. On analysis, it was seen that sodium was the nutrient associated with most (27%) red traffic lights while sugar was the nutrient that was least (14%) associated. For beverages, sugars was the nutrient that was mostly (10%) linked to red traffic lights while sodium and fats were least associated (2%). Though replacements for all foods were not possible, the percentage of foods and beverages that qualified for at least one red traffic light dropped to 40% and 2% respectively. The traffic light food labelling helped Canadian adults reduce their overall intake of energy, total fat, saturated fat and sodium compared to baseline-calorie intake reduced by 5%, total fat by 13%, saturated fat by 14% and sodium by 6% among Canadians. Men reaped maximum benefits as they consumed 122 fewer calories, 12 g less total fat, 4 g less saturated fat and 199 mg less sodium under this food labelling model. The only nutrient that did not show considerable change was sugar. It was amazing to find that total intake of calories and fat were reduced to below recommended Daily Values and this included women’s total intake of saturated fats as well. This study shows that the traffic light labelling system has a positive impact on the individuals’ total nutrient and calorie intake decreasing the consumption of fats, sugars and sodium. Sustenance of Dietary Changes Possible with Traffic Light Diet The Massachusetts General Hospital (MGH) studied the nutrient intake of their employees implementing the traffic light diet in their hospital cafeteria with simple ‘traffic-light’ symbols-the program was devised such that green labels indicated healthiest foods, yellow labels indicated less healthy foods and red labels the least healthy ones based on positive and negative criteria. Details whether the main ingredient was fruit, vegetable, whole grain and likewise with the amount of saturated fat was also mentioned. The food habits of 5,695 employees were tracked via the purchases made once after the labels were added and once again after product-placement changes made healthier choices accessible. This analysis remained in place for 2 years. Results showed that the purchases of red-labelled foods decreased while the proportion of green-labelled foods purchased increased. Such kind of labelling paved way for greater calorie reduction over the two-year period with the red-labelled foods contributing to major calorie reduction. On the whole, besides reducing total calorie intake the employees were also eating nutritious foods that contribute towards their total calorie intake. Some employees even lost up to 2 kg over time. This is not a weight loss program but one that aims at achieving a steady weight maintenance by individuals instead of allowing them to gain weight. This might be a good start for reversing the obesity epidemic. Organizations conduct wellness programs that help improve well-being of employees but such programs happen only for a short period. But this kind of an intervention is a continuing affair where people are exposed to it daily at work and in the long run it becomes a lifestyle practice. The traffic light labels could be implemented in all workplaces as employees love to eat well but don’t have enough time to read and decide. In such scenarios, the labelling helps them realize when they are about to make an unhealthy food choice and motivate them to choose a better option. Green, Amber & Red: What Do Each of the Colours Stand For? The colour codes depict whether a product is high (red), medium (amber) or low (green) in saturated fats, fat, salt and sugar and the total energy provided by it. Going by the color codes helps you choose the right food. For instance, if you would like to go for a veg roll read the color codes to decipher the nutrient content: Green: If the label is mostly green this is a clear indication that the food is low in that nutrient (fat, sodium or sugar) and you are about to make a great choice. Amber: This is an indication that the product is neither low nor high in that nutrient and it is always ok to eat foods that have amber on the labels any time. Red: This is not a declaration to avoid such foods totally but a warning sign that they are high in fats, sugar and sodium. It is always recommended to decrease consumption of red-labelled foods and if you wish to have them, eat them as rarely as possible in minimal quantities. References Traffic-light Labels Could Reduce Population Intakes of Calories, Total Fats, Saturated Fats and Sodium: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5300258/pdf/pone.0171188.pdf Traffic Light Food Labels Reduce Calories Purchased in Hospital Cafeteria: https://www.sciencedaily.com/releases/2019/07/190710134014.htm Helping You Eat Well: https://www.nutrition.org.uk/healthyliving/helpingyoueatwell/324-labels.html?start=3 An unmarried man is an eligible bachelor even during his late 30s or 40s while women don’t find themselves a suitable groom as easy as men once they cross early 30s as the society fears that a woman’s reproduction capability and the strength to bear a child decreases as she grows old. We even fear that the child might be born with disorders and complications. The health of the lady remained the sole priority even before conception to ensure a healthy baby but as our knowledge base is expanding, we seem to accept the fact that men play a vital role too. Their health before conception has a greater say in the healthy outcome of the offspring.
The dad’s age too is being considered as a risk factor for the offspring’s health. Advanced paternal age (APA) at conception has been linked to numerous negative outcomes such as low academic achievement, hyperactivity and suicide. Maternal and paternal age is linked to neurodevelopmental disorders and more prominently enhancing the risk of autism spectrum disorder (ASD). Men who father a child at an older age increase the risk of congenital disorders such as Apert syndrome, craniosynostosis, situs inversus, syndactyly, cleft lip or cleft palate and hydrocephalus. The major reason quoted behind the occurrence of diseases such as ASD and schizophrenia is the prevalence of the increased risk of mutations that occur in the germline of the dads. Hence, getting to understand the relationship between paternal age and ASD can help in shedding light on the biological pathways resulting in ASD. Advanced Paternal Age Increases ASD Risk in Offspring Associating paternal age with ASD risk started as early as during the 1970s and the study elaborated here is a population-based cohort study to test this theory. It includes a total of 3,78,891 individuals born during 6 consecutive years of whom only 3,18,506 of them had data on paternal age at birth. Information on maternal age at birth was obtained for 1,32,271 people using paternal age data. Paternal age was categorized into four groups: 15-29 years, 30-39 years, 40-49 years and above 50 years. Results for age was presented in terms of a 10-year increase in paternal age. Maternal age too was divided into 3 groups corresponding to paternal age categories: 15-29 years, 30-39 years and above 40 years. Results showed that the risk of ASD was around 8.4 cases per 10000 persons. It was observed that the risk of ASD increased with increase in paternal age. There were no signs of ASD risk in offspring of the youngest fathers as fathers younger than 20 years had no offspring with ASD. The risk of ASD almost doubled in men who were 10 years older. Researchers propose that this increase in risk of ASD with increasing age could be due to mutagenesis which was initially called as the ‘copy error’ hypothesis by Penrose according to which new mutations could arise, propagate and accumulate in successive generations of sperm-producing cells. These might be chromosomal abnormalities that could possibly link paternal age with autism. Another reason could be imprinting-a form of gene regulation where the gene expression depends on whether the allele was inherited from the male or female parent in the previous generation. Imprinted genes that are paternally expressed silence maternal gene expression. Only one parental allele is expressed while the other remains silent due to DNA methylation. While the methylation pattern is maintained in somatic cells it is erased and re-established late in spermatogenesis for paternally imprinted genes, a process that could become impaired as age advances-this stands to be considered in the case of autism. Effect of Paternal Age in Neurodevelopmental Disorders We repeatedly research and talk about the link between APA and ASD as autism is more common these days that earlier but it was schizophrenia that was the first neuropsychiatric disorder that was linked to APA. Various studies showed that the risk of the disorder increased with paternal age increase though the risk degree differed between the studies. Risk for the disorder was already high for offspring of fathers in their mid-to-late 30s increasing as the paternal age increased. Those in their 40s during conception were at a 2-3 times increased risk of becoming a dad to a schizophrenic child compared to those in their 20s during conception. The link between APA and autism was reported first by Reichenberg et al. The risk with increase in age was on similar lines as for schizophrenia-greater risk in those aged mid-30s and above during conception. Those studies focusing on the transgenerational persistence of APA-autism link showed conflicting results that the age of the maternal grandmother and maternal grandfather was linked to a higher risk of autism. Sullivan et al. reported that family history of schizophrenia and bipolar disorder was a risk factor for autism. Likewise, the presence of autism during early stages of life increases the risk of schizophrenia development during later stages. The reasons behind this link is usually attributed to genetic factors or genetic mutations in paternal gamates that arise as a consequence of ageing. The behaviour of men delaying fatherhood generally includes social withdrawal and social aloofness that’s greatly related to a higher genetic risk for autism or schizophrenia. Kids born to men with genetic variation are at an increased risk of such disorders irrespective of the father’s conception age. Though a study by Nilsen et al. showed that men who fathered their first child at an advanced age were surrounded by health problems and risky health behaviours other studies did not find any link between behavioural traits and paternal age. We have numerous debates surrounding the inherited vs de novo effects of APA. Comparison effects of delayed fatherhood and advancing paternal age many studies support that it’s delayed fatherhood that’s increasingly linked to risk of schizophrenia. But a study by Hultman et al. showed that the child with the disorder is generally born later in the father’s life showing that age-dependent factors and not men’s stable traits affect its prevalence. All of the published animal studies show that advanced paternal age at conception is related to behavioural changes relevant to autism and schizophrenia. Genetic Mutations An infant is born unto this world with around 60-80 genetic mutations but these are enhanced to a greater degree in individuals with autism and schizophrenia. Genetic mutations that multiply as the paternal age increases affect the APA effect to a greater extent. Research shows that mutation rates double every 16.5 years expressing the risks associated with delayed fatherhood from the age of 25 to 40. Age-related increase in genetic mutations is larger in male than in female by almost 3-fold times and most of the genetic mutations in offspring are primarily from the father. Selfish Spermatogonial Selection According to this hypothesis, stem cells with mutations at certain loci gain selective advantage over non-mutated spermatogonial stem cells expanding clonally and becoming prominent in the germline. Activating mutations involved in receptor tyrosine kinase pathway enhance growth processes leading to abnormal proliferation of spermatogonial stem cells that carry these mutations via a process called oncogenesis. The disease phenotypes linked to the mutations make it unlikely for the mutations to be passed over multiple generations making it mostly unsuccessful for extrapolating the hypothesis for complex disorders like autism and schizophrenia. A study by Goriely et al. showed that the genes that were responsible for the selfish behaviour of spermatogonial stem cells belong to the RTK/RAS/MAPK pathway-one of the molecular modules that’s rich in deleterious variants in neurodevelopmental disorders. It is a common opinion among researchers that analysing the selfish selection hypothesis plays an integral role in triggering genetic mutation origins of APA effects. APA and neuropsychiatric disorders also change based on epigenetic effects -the epigenetic markers regulate gene expression in offspring showing that paternally acquired factors affecting the offspring go beyond those proposed by the genome sequence alone. DNA Methylation: This is the commonly studied epigenetic modification playing integral role in gene regulation. DNA methylation marks are stable, modification acquired are maintained in daughter cells accumulating over paternal lifespan in a similar fashion as de novo genetic mutation. It is to be noted that epigenetic programming occurs twice during fertilization-once before birth in embryonic primordial germ cells and then followed by establishment of new methylation patterns that’s different in male and female embryos. The programming once again occurs at fertilization. Ageing brings about changes in epigenetics and DNA methylation levels help in predicting chronological age of humans. It was Malaspina in 2001 who first proposed that age-related epigenetic modifications mediated APA effects. But, age-related disruption of normal DNA methylation in gametes cannot account for the father-to-offspring transmission of the APA effect. Even before the blastocyst stage paternal methylation marks are erased with only those in the imprinted regions remaining in the embryo’s somatic cells. So, the time frame within which paternally acquired non-imprinted DNA methylation marks could affect offspring development is scarce. Genomic Imprinting: Imprinting is a complex phenomenon where differential DNA methylation in paternal gametes is linked to monoallelic gene expression in offspring. These imprints are seen in parental germline, inherited after fertilization, erased in fetal germline and later re-established in the offspring. The imprinting regions regulate gene expression which are found in both sexes and autosomal chromosomes characterized by age- and tissue-specific expression patterns. They also play a vital role in early development regulating placental formation and functioning and also early brain development. The parental imprints in the germline could be present in the somatic offspring cells conveying the message that imprinted genes could be involved in mediating APA effects. Various studies have shown a number of neurodevelopmental disorders (such as Prader-Willi syndrome or Angelman syndrome) that have resulted as an outcome of errors in imprinting. But we have no research in humans that supports the theory that imprinting errors affect APA effect. It is hence seen that inherited and de novo factors contribute to epidemiological observations. But the evidence does not suggest that older men should refrain from having a child. There is a low occurrence rate of these disorders at baseline and a 5-fold increase in odds ratio even under a strong de novo effect gives us a low probability that the offspring will suffer from autism or schizophrenia due to a high paternal age. Studying the Effects of Paternal Age on Twins The present study uses a population-based sample of twins (Twins Early Development Study [TEDS]) to test the effect of paternal age on offspring behaviour. A study by Lundstrom et al. proved that the effects of APA was observed in the offspring only when he/she was around 9 years. Sample size from the TEDS study-of more than 15000 twin pairs-were collected. These individuals were assessed of their social functioning skills at age 4, 7, 9, 14 and 16 respectively. Social development was measured using parent’s (mostly mothers) rating of the Strengths and Difficulties Questionnaire (SDQ) that helped in analysing both good and problematic aspects of childhood behaviour between 4 and 16 years. The questionnaire mainly focused on five subdomains including conduct problems, emotional symptoms, hyperactivity, peer problems and prosocial behaviour. The effect of paternal age on all five subdomains was checked through five questions scored from 0 to 2 such that the maximum score possible for the subdomain was 10. Contrary to other domains, high scores in the prosocial domain indicated less problematic behaviour. Results showed that there was a significant link between paternal age and differences in social development in the general population with no effect on behaviour domains. Some kids born to older fathers find it difficult in social settings and the challenges they face increase as they get older. Genetic influence on social development is most pronounced on offspring of the oldest group of fathers. References Advancing Paternal Age and Autism: https://jamanetwork.com/journals/jamapsychiatry/fullarticle/668208 Advanced Paternal Age Effects in Neurodevelopmental Disorders-Review of Potential Underlying Mechanisms: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5299396/pdf/tp2016294a.pdf Paternal Age Alters Social Development in Offspring: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5409803/ Movies are not spicy without a villain and life too seems to be bland when it goes on and on without some challenges to dethrone. So is the connection between free radicals and antioxidants. Our body is our recluse from which we garner energy for day-to-day functioning of all activities. This energy is acquired from the food that we eat. Free radicals are produced as a consequence of metabolic steps when food is converted into energy, as a result of normal cellular function and also as part of natural physiological process of all living beings. They might also be derived from external sources such as exposure to X-rays, ozone, cigarette smoking and industrial chemicals. There is a continuous formation of free radicals happening in our body as a result of enzymatic and nonenzymatic reactions. Until their production is normal there is no harm caused from them but once overproduction happens, they can become dangerous to even basic processes needed to keep individuals alive. In order to avoid such damages, the cells also produce free radical scavengers known as antioxidants.
Free Radicals & Antioxidants Free radicals are molecules that contain one or many unpaired electrons in their outer orbit which become highly unstable when they try to react with other molecules to attain molecular stability. In this outreach, the free radical robs other molecules of their electrons creating a chain reaction leading to the damage of DNA and protein breakdown. But it is essential to known that not all free radicals are harmful and there are some of them which help to wipe out invading pathogenic microbes to protect the body’s defense mechanism. In science, we use the terms reactive oxygen species (ROS) and reactive nitrogen species (RNS) to describe free radicals and other non-radical reactive derivatives. The human body has its own tactical ways for self-defence. It has an excellent antioxidant network that plays the defense role helping to neutralize free radicals and maintain homeostasis. But the defense mechanism doesn’t work in favour of the individual all the time where an imbalance between free radical production and antioxidant defense is possible. Such imbalance leads to what we call ‘oxidative stress’. This oxidative stress is considered to be the starting point for the origin of numerous diseases, development of ageing and the onset of health problems such as arthritis, cardiovascular and neurodegenerative diseases, inflammation and cancer. Oxidative stress is also possible due to poor diet or disease. Nowadays, we read numerous articles that suggest the consumption of various foods for antioxidant benefits but there are also questions raised whether performance of exercise can alleviate the effects of free radicals. Exercise & its Effect on Free Radicals Physical activity has been proposed as a solution to remove the harmful effects caused by free radicals on the human body. Various studies these days show evidence that ROS are generated during exercise but physical activity helps in improving antioxidant defense. Physical activity is different from exercise. We define physical activity as some body movement produced by skeletal muscles resulting in energy consumption and examples include everyday life activities and exercises such as walking and cycling. Moderate exercise and an active lifestyle have been proposed as good ways to reduce oxidative stress. It finally depends on the exercise duration, intensity, fitness condition and nutritional status as to whether the reactive species are helpful or harmful. On the other hand, we also have research showing that exercise-induced free radical production promotes insulin sensitivity in humans thereby acting as a catalyst for type 2 diabetes prevention. Regular practise of moderate-intensity exercise helps to stay away from oxidative stress while acute bodily exercises can cause oxidative stress and increase the production of free radicals. Overperformance of exercise increases the amount of reactive and nitrogen species which increase ROS production and RNS might cause imbalance among RONS and antioxidants. Hence, exercise-an activity that must benefit the body-becomes the cause for exhaustion and injury. Effect of Low-intensity Exercise on Antioxidants & Oxidative Stress The study included 2 groups: one group of low-intensity exercise performers (EXG) and another one performing no exercises called the control group (CG) with each group consisting of 20 participants. Low-intensity exercise is that which gets you to about 40-50% of your maximum heart rate (MHR) such as jogging and walking. Those individuals above the age of 30, suffering from chronic diseases or taking long-term medications were excluded from the study. Blood samples of all the participants were collected and antioxidant capacity of the samples was estimated using the Benzie and strain method. A comparison between the two groups was made regarding body mass index (BMI), alanine transferase (ALT), alkaline phosphate (ALP), aspartate (AST) and FRAP. Significant difference in BMI values was found in both groups with BMI of CG less than the BMI of EXG. ALT of CG was less than that of EXG; ALP of CG was high than the ALP of EXG; AST of CG was less than the AST of EXG. The study concluded that low-intensity exercise had no effect on liver enzymes but improved blood life quality by reducing various health problems related to oxidative damage of cells and muscles fatigue. Physical Activity Improves Antioxidant Capacity in Individuals with Type 2 Diabetes Mellitus We have numerous evidences pointing to the fact that free radicals and oxidative stress contribute towards Type 2 diabetes mellitus (T2DM) and its related complications. Some of the causes of oxidative stress during diabetes include overproduction of ROS by mitochondria and nonenzymatic glycation. Physical activity or exercise helps to improve insulin resistance by improving insulin action and vascular function while decreasing ROS generation. Animal studies were conducted to bring about the effect of exercise on T2DM. Regular and moderate-intensity aerobic exercise that consisted of 12 weeks of swimming was conducted for both diabetic and lean rats which were between 8 and 20 weeks of age. The animals performed the exercise in a cylindrical tank that contained water in a controlled temperature. The animals were placed in the tank everyday at the same time. While the duration was for 15 min/d initially it was increased to 60 min/d by the end of the first week and the schedule was followed thrice every week. The sedentary rats were placed in similar containers where the swimming session was held for all the 60 min to ensure that rats in both groups underwent the same amount of stress. The research team observed an amelioration of insulin resistance and diabetic dysmetabolism. A decrease in systolic and mean blood pressure and heart rate, decrease in oxidative stress and increase in NO production was observed. Antioxidants came to the defense of animals with T2DM in yet another study by Nishida et al. which reported increased Cu/Zn-SOD protein production as a result of low-intensity exercise in contrast with increased Mn-SOD after moderate-intensity exercise. Studies from other researchers on a six-month moderate-intensity aerobic exercise training showed decrease in lipid peroxidation, increase in GSH and catalase activity in T2DM and obese individuals. Oliveira et al. compared the effects of 12 weeks of training on 3 different exercises (aerobic, strength and combined training) on T2DM male and female human participants showing that aerobic training program provided important upregulation in antioxidant enzymes and increased NO bioavailability which helps to minimize oxidative stress and chronic complications of diabetes. Hence, regular and moderate exercise can have antioxidant and anti-inflammatory effect in individuals with type 2 diabetes. Both aerobic and anaerobic exercise can produce free radicals but oxidative stress always doesn’t occur because ROS production is dependent on the exercise intensity. While high ROS production due to acute exercise performance is harmful to the immune system chronic exercise produces physiological adaptations that can empower a person’s antioxidant system. References Regular Physical Exercise as a Strategy to Improve Antioxidant & Anti-inflammatory Status: Benefits in Type 2 Diabetes Mellitus: https://www.hindawi.com/journals/omcl/2012/741545/ Oxidants, Antioxidants & the Beneficial Roles of Exercise-induced Production o Reactive Species: https://www.hindawi.com/journals/omcl/2012/756132/ Is Exercise the Best Antioxidant Supplement? https://www.unm.edu/~lkravitz/Article%20folder/Antioxidants.pdf Impact of Low-intensity Exercise on Liver Enzymes and Antioxidants Systems of the Body: https://www.unm.edu/~lkravitz/Article%20folder/Antioxidants.pdf  Oh Little One, Why Don’t You Go to Sleep & Decrease Your Risk of Obesity? Oh Little One, Why Don’t You Go to Sleep & Decrease Your Risk of Obesity? Obesity rates have become unjustifiable with more than 40% of adult population staying overweight and more than 14% of children existing in the obesity zone. Inappropriate environmental, biological and psychological factors have resulted in a situation where obesity rates have tripled since 1975. We have moved past the fact that adult obesity rates are inappropriately high and now researchers are mainly focusing on childhood obesity rates. 10% of the global population is obese and almost 15% of kids between 2 and 5 years old are obese. We have multiple research on the effect of early life factors and its effect on childhood obesity. Its also known that maternal and paternal obesity increase the risk of obesity in the offspring and most excess weight in childhood are gained during the preschool years. Some of the evident examples come from some of the most developed nations-U.S. has 69% adults and 32% kids either in the obese or overweight range; Western Europe exbibits some of the highest obesity/overweight rates and data from the ‘National Child Measurement programme’ (NCMP) shows that more than one in five kids in England are now obese/overweight by the time they are enrolled in primary school and the rates increase further to one in three by the age of 6. To make things worse, 8% of infants and toddlers display weight ranges above 95th percentile in the U.S.A. This is indeed a nightmare as obesity/overweight that’s prevalent in these tender years is sure to linger past adolescence and well into adulthood. Childhood Obesity Staying above recommended weight ranges since childhood puts the kid at a potential risk for comorbid conditions such as diabetes, cardiovascular problem and even cancer. We have a good number of research done on the risk factors of obesity during childhood years such as children’s eating habits, infant feeding practices and television viewing but what we need exactly is to understand the factors present in both parents and offspring that promote obesity across early life stages (right from preconception through prenatal period to infancy to the tender age of 2). Though researchers focus on risk of obesity through childhood and adolescent years we have evidence showing that the foundation for inappropriate weight gain is laid in early years of life by actions and interactions that can have biological and behavioural consequences. Such influences on obesity and risks for it are linked across generations-from parent to child. An understanding of various processes and sewing them together in the right order helps us focus on the generation link that’s evident. The intrauterine environment shapes the trajectory of weight gain and after birth the teachings of parents and families combined with the socioeconomic environment has greater impact on the weight trajectories of infants and toddlers. Obesity rates of kids greatly vary depending on where they live. Seeds of Obesity Sown Even Before Deciding to Plant Preconception: The risk of obesity in the next generation starts even before conceiving. Until sometime back most studies focused on maternal influence of obesity on the offspring but recently even the paternal involvement in determining offspring’s health has now been taken into consideration. The major factors affecting offspring include a mother’s birth weight, obesity and nutritional status throughout her life. Pre-pregnancy obesity rates have steadily increased since the last decade to the present one and statistics show that mothers who are overweight/obese before pregnancy are at an increased risk of having children who are large for gestational age at birth compared to their normal weight counterparts. A study by Whitaker et al. showed that maternal obesity during the first trimester of pregnancy doubled the risk of childhood obesity at 2 years of age. Fathers affect embryonic development through genetic and epigenetic mechanisms. Epigenetic changes affect the fetus’ metabolism which is primarily due to variations in the dad’s diet. This shows that paternal lifestyle behaviour definitely puts future kids at risk of obesity and obesity-related outcomes. These epigenetic changes could even be inherited by the developing sperm. All this clearly show one thing-the world that’s been monopolizing the attention to women who plan to conceive must also consider the health of men. A number of suggestions have been proposed for women in their reproductive years right from nutritional guidance to weight management. They are advised to take supplements that include multivitamins and folate to avoid deficiencies such as neural tube defects and likewise. A survey showed that 77% women opted for enrolling in a program that promoted effective lifestyle intervention before conceiving and this shows that women are on the right track. Men should also be encouraged to take care of their health. Actually, both men and women must be motivated to stay within normal weight ranges right from adolescence to help the future generation to stay at a minimal risk of obesity. Prenatal influence: The environment affects us in many a way. Environmental exposure and timing of exposure to different factors within the environments produce interactions that are biologically seeded in the developing child. Epigenetic influence do exist and the gene sequence cannot be modified but we can indeed change the gene expression in response to environmental cues. For instance, changes to the placenta made as a result of maternal stressors or nutritional status prevails as the mediator between the developing child and the environment. This prevails as the trailer for the fetus before the main picture is shown (when the fetus then becomes a newborn). The fetus becomes adapted to epigenetic changes which then regulate behaviour, obesity and glucose tolerance. But when the fetus is small for gestational age during development or there was restricted intrauterine growth the growing newborn is at a greater risk of suffering during later stages in life. When metabolic pathways, hormonal signalling and glucose metabolisms change by a greater margin during pregnancy it increases the risk of larger birth size and higher percentage of body fat at birth. The gut bacteria also play a critical role as researchers have come up with differences in the microbiome of overweight individuals compared to normal-weight people. The same is also seen in pregnant women and hence, might be transferred to the child too (as the child gets the microbiome composition from mother during birth through the birth canal and it’s also affected by the mode of delivery) thereby resulting in intergenerational transfer of obesity. Maternal Lifestyle: Time and again gynaecologists insist on a healthy maternal weight gain and lifestyle behaviours to deliver a healthy offspring. Eating, physical activity and smoking levels during pregnancy have a strong impact on the risk of obesity for the fetus developing inside the mother’s womb. Besides preconception obesity gestational weight gain (GWG) changes the pregnant woman’s metabolism leading to higher risk for dyslipidaemia, glucose intolerance and insulin resistance. Such GWG leads to a greater percentage of offspring born with higher birth weight, increased body fat during the neonatal period and greater adiposity all though childhood and adulthood as well. All this is due to increased nutrition transfer from overnourished mothers to the developing fetus. Moms pass on food likes and dislikes to the developing fetus. The food that she consumes, her tastes and smelling traits that are present during fetal development strongly influence a child’s preferences for food and flavour. Now we can understand why our little ones love sweets, hate certain vegetables and relish certain foods more than others. Performing physical activity regularly during pregnancy helps the woman deliver infants that are smaller than the ones born to women who don’t exercise. Different studies come up with different results and hence reviews are inconclusive. Another important factor affecting fetal weight is smoking status of the pregnant woman. Smoking, both maternal and paternal, during the prenatal period is strongly linked to obesity development in the offspring during childhood and adulthood. Numerous systemic reviews and meta-analysis of data show that maternal pre-pregnancy weight gain is linked to an increased risk of overweight/obesity in the offspring, children born to moms after weight loss were only at a 35% risk of overweight/obesity compared to 60% risk in kids born to moms who remained obese, according to a study. A recent systemic review showed that 19 of 21 studies supported increased risk of childhood overweight in kids when moms experienced GWG. Kids of women who gained excessive weight during pregnancy were at a 4-times higher risk of being overweight at age 3 compared to kids whose mothers gained inadequate weight according to a study by Oken et al. A population-based cohort study proved that compared to infants of women who gained 8-10 kg of weight during pregnancy those of women who gained more than 23 kg were about 2.5 kg heavier at birth. Factors Affecting Obesity Risk Up to 2 Years of Age: Infant birth weight is a strong determining factor of obesity/overweight risk in the child. Kids born either too small or big for gestational age are at an increased risk of overweight, obesity, metabolic disorders and cardiovascular diseases. The birth weight of the child is determined by the maternal weight at conception and GWG. As in adults, infants too should gain a definite weight in a definite period and accelerated weight gain occurring during the first 4 months of life are related to obesity at 7 years of age and a 60% increase in risk if weight gain happens within the first 2 years of life. but the reason behind rapid weight gain during this period is due to genetic factors, epigenetic processes, differences in placental leptin levels and the infant’s gut microbiome composition. Infant-feeding habits: Kids depend on their parents for making the right decisions up to a certain age and food habits are one of those. What and how much food parents feed their infants directly affect the weight gain and obesity risks of child during later stages in life. There are not any recommended dietary guidelines for kids younger than 2 years of age to help parents and caregivers choose the right portions and foods to feed the kids. Infants are blessed with the knowledge to know how much to eat, when to eat and when they are full. They self-regulate their needs even while breastfeeding choosing how much to drink how often. That’s why infants fed on formula by parents gain more weight maybe due to the amount and pattern of feeding and so do infants who start weaning early in life. The child’s ability to self-regulate narrows down when it is dominated more and more by parental intervention. Sometimes, parents feeding practices also depend on the child’s food choices which is affected greatly by its exposure to sweet and sour taste during prenatal exposure to the mother’s diet but they can be modified by repeated exposure to certain foods by the parents. Some parents also use feeding as a mechanism to soothe infants and such practices lead to unintentional weight gain in kids. Our lifestyle and sedentary behaviour also hold greater influence on obesity risks. The present world encourages the use of car seats and strollers that make the children idle, exposure to television starts right from their 3rd month sometimes and many suffer from lack of sleep due to increased screen time. A prospective cohort study on more than 900 infants showed that those who slept for less than 12 hours doubled their odds of becoming overweight by age 3 compared to others. An infant’s birth weight and rapid weight gain during the first months of life are clear cut indicators of future obesity risk. Hence, it does show that the way parents and caretakers feed infants and the steps that they take to engage children do affect the risk of long-term weight gain in these little ones. In recent years, more attention has been focused on interventions targeting parents and modifiable risk factors that prevent obesity and promote healthy growth in the first 1000 days of life. Lifestyle and nutrition practices followed through life-before conception, time spent in utero and the following months after birth greatly affect the child’s weight at birth, during childhood and well into adulthood. Women who take care before conceiving, while pregnant and even after childbirth have greater chances of giving birth to and nurturing kids who are at a minimum risk of obesity in life. Nutritional interventions by parents, the steps they take to ensure kids’ exposure to healthy food and their participation in physical activity plans with the children do indeed help in making the kids as healthy as possible. It would be beneficial for both the kid and the mother when the woman strives for a healthy weight before pregnancy, abstains from smoking, strives for a normal weight gain during pregnancy, breastfeeds unless there is some health issue linked and takes care that infants get the desired sleep time during the first few years of life. References Preventing Obesity Across Generations: Evidence for Early Life Intervention: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5305001/ Prevention of Overweight & Obesity in Early Life: https://www.cambridge.org/core/journals/proceedings-of-the-nutrition-society/article/prevention-of-overweight-and-obesity-in-early-life/F9BB50517A0A0F9D4F542276A30926D5/core-reader The Effect of Early Life Factors & Early Interventions on Childhood Overweight & Obesity: https://www.cambridge.org/core/journals/proceedings-of-the-nutrition-society/article/prevention-of-overweight-and-obesity-in-early-life/F9BB50517A0A0F9D4F542276A30926D5/core-reader Preventing Childhood Obesity: Early Life Messages & Epidemiology: https://onlinelibrary.wiley.com/doi/full/10.1111/nbu.12277 Prenatal & Early Life Influences: https://www.hsph.harvard.edu/obesity-prevention-source/obesity-causes/prenatal-postnatal-obesity/ Despite our food being an enriching source of nutrients and full of goodness we don’t make utmost use of this naturally available health source but try to achieve the same through other means such as supplements and likewise. Fruits, vegetables and whole grains-authentic nutrient source-have been taken for granted and now, we are victims of serious nutrient deficiencies and health-related problems. Due to continuous breaching of these nutrient sources we have landed ourselves in a state where supplementation has become indispensable for a majority of individuals.
A majority of the population are regular consumers of multivitamin supplements on a daily basis. Vitamin D and vitamin B deficiencies are on a rise for which supplements have once again become mandatory otherwise this can result in serious health consequences. Another group of supplements that’s especially crucial for vegetarians and vegans are fish oil supplements that have been steadily used for lowering blood triglyceride levels in all individuals including athletes. So, what’s so special about these supplements that makes it a favourite of athletes too? The very fact that they contain omega-3 fatty acids which cannot be produced by our body but must be added via the food that we consume. Omega-3 fatty acids have been proposed for protecting the heart, improving mental life, easing inflammation and lengthening life and deficiencies have created innumerable problems right from arthritis and mood disorders to cancers, cardiovascular diseases and more. The most recent fascination on omega-3 supplementation is the fact that these have been proudly presented as an ergogenic aid for athletes for improved athletic performance. Omega-3 Fatty Acids Sharks, swordfish, tilefish and albacore tuna are rich sources of omega-3 fatty acids but they come with a statutory warning that these might be loaded with toxic substances. Hence, controlling the consumption of these fish is always recommended to avoid effects due to mercury overload and so. Fish oils are made from the tissues of oily fish and are overloaded with eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), both of which are forms of omega-3 fatty acids. Omega-3s are polyunsaturated fatty acids (PUFAs) which exert anti-inflammatory properties. Interestingly, though fish is the best source for omega-3 they too don’t produce it but acquire it by consuming microalgae or fish that’s enriched in omega-3 fatty acids. Sometimes called as vitamin F due to its presence in ‘fatty fish’ sea creatures such as krill, algae, microalgae and crustaceans are also excellent sources of n-3 PUFAs. Alpha-linolenic fatty acid (ALA) is also a form of omega-3 but primarily found in soybeans, pumpkin seeds, perilla seed oil, walnuts, flaxseed and canola. But sadly, ALA from food sources must be converted into DHA and EPA before reaping benefits. DHA and EPA have even been named as ‘brain food’ because of their prime participation in cognitive health. So, fish oil supplements are indeed helpful in preventing illnesses and promoting health but they are not a one-stop solution for all the problems and illnesses as advertised by marketing individuals. With this in mind, let’s look at where we stand with respect to fish oil supplementation and athletic performance. Fish Oil Supplements & Athletic Performance Athletes need greater sustenance capacity and energy for maximized performance. Because of this, we have seen that most of them use dietary supplements to increase metabolic capability, delay fatigue, improve muscle hypertrophy and shorted recovery period. Any athletic performance requires a strict exercising routine that exerts physiological stress on the body. The body tries to counter this by going for a joint response by the cardiovascular, pulmonary and nervous system as this increases blood flow and oxygen supply to skeletal muscles. There is a tremendous change in blood flow during rest and exercise-while muscles receive 20% of total blood flow during rest, they receive more than 80% during exercise. In such scenarios ergogenic aids are of utmost use as they aid in improving exercise efficiency and also enhance recovery. Omega-3 are considered as an ergogenic aid here as they are helpful in restricting exercise-induced inflammation and enhancing health of muscle and energy availability. Intense exercise can lead to oxidative stress and reactive oxygen species (ROS) production occurs due to muscle contraction. This is greater than antioxidant capacity of the muscles and might lead to fatigue development in athletes. There are various experimental studies showing that dietary intake of PUFAs could optimize immune and inflammatory response. The consumption of omega-3 decreases interleukin IL-1 and IL-6 prevents inflammation. Daily prescription of 4 g of n-3 PUFA on young and old subjects for 8 weeks showed significant increase in muscle protein synthesis; another study that administered the supplement for six months showed improved muscle mass and strength in elderly adults. Seven days of 3 g/day of PUFA supplementation decreased post-exercise muscle damage and soreness in individuals who performed eccentric biceps curls. Chronic supplementation of n-3 PUFAs improves neuromuscular activity in animal studies and they are indeed an excellent supplementation for athletes given the fact that they are helpful in recovery during training or competition. A study was conducted on 20 international rugby players for 5 weeks of pre-season training. These players were made to consume a protein-based supplement consisting of n-3 PUFA twice a day or a protein-based placebo to check on muscle soreness, countermovement jump performance and psychological well-being. All the players filled a questionnaire assessing their fatigue, sleep, stress and mood levels every day during the training period. Results showed that PUFA supplement improved better maintenance of explosive power in the rugby players during pre-season training. Immune-related Effects Exercise provides a platform for infectious agents to enter the body and cause diseases due to alterations in immune functions (this is the work of pro-inflammatory cytokine production, decreased neutrophil function and NK cell cytotoxicity). Studies show that n-3 PUFA supplementation decreased IL-6 production in athletes. A study focused on the immune functionality of fish oil supplementation on athletes who underwent endurance training-16 male subjects underwent a six-week double blind placebo supplementation trial involving two groups (fish oil or placebo oil). Each of them visited the research team twice-during the first visit they underwent a maximal exercise test and during the second they performed 1-h of endurance exercise on a cycle ergometer. Results showed that fish oil supplements reduce increase in peripheral blood mononuclear cell production. Immune levels are suppressed after performing high-intensity exercises and such decline in immunity levels increases the risk for upper respiratory tract infections. There are several studies that support the fact that n-3 PUFA supplementation can combat such infection risk. Asthma-related Effects A study defined asthma in elite athletes as ‘sport asthma’ that’s nothing but respiratory symptoms and bronchial hyperresponsiveness without allergic features. Some athletes, such as those involved in sports such as skiing and long-distance running/cycling that require intense breathing. Likewise, swimmers too face this issue due to inhalation of chlorine derivatives in the swimming pool. Eskimos exhibit low asthma rates as they consume more of omega-3 fatty fish. Studies show that n-3 PUFA intake reduces asthma rates because of its anti-inflammatory mechanism: Supplying asthmatic patients with 3.2 g of EPA and 2.0 g of DHA daily for 3 weeks reduces eicosanoids and pro-inflammatory cytokines concentration. Yet another study that supplied the same supplement combination and an anti-LT medication showed that both the supplement and the medication were independently effective in attenuating airway inflammation and bronchoconstriction. Exercise-induced bronchoconstriction improved when individuals were supplied with n-3 PUFAs. Effects on Joint Pain Joint pain is a common complaint for athletes especially those participating in sport with joint torsional movement such as football, volleyball and tennis or increased articular impact loading such as football, running and basketball. There is an increased chance of developing osteoarthritis in athletes when they are involved in playing a sport that has rapid acceleration/deceleration or causes high impact on joints continuously. Joint pain is the result of infiltration of inflammatory cells and n-3 PUFAs could help preserve joint health. A New Zealand study reported reduced inflammation in animal and human trials with 89% decrease in pain symptoms and 91% increase in quality of life. Studies & their Supporting Evidences for Fish Oil Supplementation Nieman et al. supplied 23 cyclists with 6 weeks of fish oil supplementation to check their effect on exercise performance, inflammation and immune measures. Results showed that the supplement increased blood levels of EPA and DHA but had no impact on exercise performance, inflammation and immune response. Poprzecki et al. showed that supplementing men with omega-3 for 6 weeks increased antioxidant activity. Omega-3 supplementation improves muscle flexibility in endurance athletes and in younger adult athletes it contributes to lower peak heart rate, reduces resting heart rate variability and oxygen consumption required while exercising. But there are several other studies showing not much improvements in markers of inflammation, performance and immunity. Another study on young men and women performing endurance exercise showed that supplementing with krill oil did not impact immune function nor affect markers of exercise performance. Though fish oil supplements decrease triglyceride levels in athletes and nonathletes we need more concrete studies to show that they are an effective ergogenic aid for exercise performance. For those consuming fish, it is advantageous as it increases fish oil intake but too much of it is also hazardous to health. Get in touch with your physician for the recommended dosages of the supplements. References Omega-3 Polyunsaturated Fatty Acids: Benefits & Endpoints in Sport: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6357022/ Omega-3 Fatty Acid Supplementation: Helpful for Exercise? https://www.uws.edu/omega-3-fatty-acid-supplementation-helpful-for-exercise/ Fish Oil Supplementation & Athletic Performance: https://journals.lww.com/acsm-healthfitness/Fulltext/2012/09000/Fish_Oil_Supplementation_and_Athletic_Performance.9.aspx?WT.mc_id=HPxADx20100319xMP Fish Oil: Friend or Foe? https://www.health.harvard.edu/blog/fish-oil-friend-or-foe-201307126467 Osteoporosis is a concern for each of us as there are millions of individuals around the world suffering from this debilitating condition. As the world’s ageing population seems to increase the prevalence of osteoporosis and osteopenia also increases characterized by decreased bone mass and increased fragility risk. According to the Osteoporosis Consensus Development osteoporosis is a metabolic bone disease characterized by low bone mass and microarchitectural deterioration of bone tissue leading to enhanced bone fragility and a consequent increase in fracture risk. When the condition is not prevented it progresses until the bone is fractured (mostly includes regions of the hip, wrist and lumbar spine). Menopause brings about numerous hormonal changes in women and they can lose around 20% of bone mass in the initial 5-7 years which finally can result in osteoporosis. Its been shown that 50% of women and 25% of men over the age of 50 will suffer from fracture due to osteoporosis in their lifetime.
Bone is a living tissue that constantly breaks down and rebuilds but with the advent of diseases such as osteoporosis there is more breakdown than building up. But this is not irreversible and exercising helps in rebuilding bones and reducing the likelihood of fracture. Exercising has been recommended as an inexpensive and safe intervention technique for preserving musculoskeletal health but all types of exercises don’t have the same beneficial effect on bone mineral density (BMD). According to the World Health Organization (WHO) osteoporosis and osteopenia are defined as the lowest BMD T-score of ≤-2.5 and -2.5 to 1.0 measured at the lumbar hip or spine. Present guidelines include resistance training and weight-bearing exercises for preventing bone loss and preserving bone mass in patients with osteoporosis. BEST Study Strength training helps to maintain or rather improve BMD, promote increased levels of bone formation markers (such as type 1 collagen amino-terminal propeptide (P1NP)) and decrease levels of bone resorption markers (such as type 1 collagen C breakdown products (CTX)) in the blood. We have reports on a positive association between maximal muscle strength measured as 1-repetition maximum (1RM) and bone mass. We have strength training programs that focus on 1RM improvements to be helpful in improving BMD and bone mineral content (BMC), especially in postmenopausal women. A study focused on 1-year and 4-year results from the Bone Estrogen Strength Training (BEST) Study was the most extensive study in United States that began in 1995 focusing mainly on how strength training combined with calcium intake impacts BMD in two groups of postmenopausal women. Anyone whether or not they were undergoing hormone replacement therapy (HRT) were allowed to participate in the study which meant a total of 266 women aged 45-65 years completed the first year of study. Sedentary (<120 minutes of exercise per week) postmenopausal women were selected and were randomly assigned to either control or exercise group and all participants took 800mg of calcium citrate supplements daily. Each of the participants’ dietary intake through the first year was assessed using 8 randomized days of dietary recall (DR) collected at baseline, 6 months and 12 months of study. While those in the control group continued with their sedentary lifestyle those in the exercise group performed weight bearing and resistance exercises 30 days per week on non-consecutive days. These exercise sessions lasted for 60-75 minutes and included weight-bearing activities for warm up, strength training and cardio weight bearing circuit of moderate impact activities at 70-80% of maximum heart rate such as stair climbing on step boxes wearing weight-bearing vests and small muscle exercises including stretching and balancing ones. All types of exercises and its duration was regularly monitored and the data entered by BEST trainers. The participants performed strength training exercises using free weights and machines focusing on major muscle groups. 8 different exercises were performed that included seated leg press, weighted march, lat pull down, seated row, back extension, one-arm military press, squats and rotary torso machine. All the subjects completed two sets of 6-8 repetitions at 70% (twice a week) and 80% (once per week) of the one-repetition maximum. 1-Year Impact Results were positive for those who exercised as exercise group participants witnessed improved BMD compared to the control group. In those who used HRT, the use of calcium, HRT supplements and exercising increased hip, neck and femoral BMD by 1-2% while the use of supplements with no exercise performance had a non-significant effect on BMD. In those participants who did not undergo HRT, the performance of regular exercise improved BMD by almost 1% whereas abstinence from exercising decreased their BMD to a great extent. The study clearly proves increased advantage for those women who use HRT. Besides BMD, BEST intervention also had positive effects on soft tissue composition-inclusion of all body components except bone. DXA measurements showed that women who exercised regularly displayed whole body and regional (arms and legs) lean soft tissue (LST). Though there was no improvement in LST in those who used HRT the use of HRT did prevent loss of LST in those women who did not exercise. There was significant fat mass loss in those women who used HRT and also exercised. Nutrition intake also had a significant effect on BMD-a greater intake of calcium, iron, zinc, magnesium, phosphorus and vitamin D was significantly linked to better BMD at the end of the first year of study. At baseline, a subsample of 242 women who completed DRs having dietary iron intake levels greater than 20 mg/day was linked to greater BMD at several bone sites when the participant’s daily calcium intake was from 800-1200 mg/day only. At the end of the first year of study 228 women had complete DR data. Among the 228 women, those who took HRT and consumed lowest amount of calcium showed increase in BMD as iron intake levels increased from 7 mg/day to 32 mg/day. In those who did not take HRT there was BMD increase only in those who took highest calcium intake with no changes due to iron intake levels. The study showed that when women lifted more weights, they experienced greatest improvements in BMD, more specifically at the hips. Bone loss is not a short-term effect but something that takes place for many years after menopause and performing exercise meanwhile can definitely curb this effect. There are many studies dealing with the effects of exercise only on short-term advantages-one that happens within 1-2 years of exercising. The BEST study focused on long-term results and found that two sets of exercise was sufficient to increase BMD and the initiate to lift weights was necessary to further improve BMD levels. To help participants continue with the BEST exercise program the duration of exercising was reduced to 45 minutes and 6 strength training exercises that excluded rotary torso machine and weighted march. Some of them were also involved in doing yoga, spinning and Pilates to break the monotony and bring in variety to their exercising schedule. 4-Year Impact It was only 167 women who completed 4 years of participation in the BEST study. At the end of the first year all of them were encouraged to exercise on their own and also have yearly DXA assessments conducted by the study group. At the end of the second year, supervision was reduced in the facilities, in the other years trainers were there in the facility only once a month. After 4 years the participants’ exercise frequency varied from 0-94% of the various exercises mentioned above. those participants who were actively engaged in exercising maintained or improved BMD at the hip and lumbar spine (LS). Those who showed maximum exercising efficiency experienced greatest BMD improvements at all bone sites than those who exercised less often. But it was observed that greatest increase in LST and BMD occurred in the first year of the BEST study regardless of HRT use. While LST increased during first year the effect was lost for years 2-4 yet the overall gain remained well above normal ranges. It was the LS BMD that continued to improve consistently for 4 years of participation in the BEST study program. Those women who completed 4 years of the study taking 800 mg/day of calcium supplements but who were not on HRT showed maximized improvements in BMD than those taking less calcium supplements. Those women not on HRT and following BEST exercise schedule need at least 1700mg/day (this is 500 mg more than recommended DRI values for women aged 50+) of calcium supplements to preserve BMD. This shows that calcium too apart from exercising plays a pivotal role in determining BMD in individuals. At the end of the 4-year period it was noticed that women who attended maximum exercise sessions and lifted greatest amount of weights showed greatest gains in LS BMD compared to those women who attended minimum exercise sessions and lifted least amount of weights. At the end of 4 years training, there was a 2.5% difference in LS BMD between those women who lifted greatest amount of weight and those who lifted least. Those who lift the greatest weights reaped maximum BMD benefits. This study thus shows that physicians and health experts can use the BEST exercise program for improved bone density. Strength Training Effect on Postmenopausal Women We have one study reporting that power training focusing on high-speed contractions was more effective than conventional strength training for reducing bone loss while another study showed that neuromuscular performance (this makes rate of force development (RFD) capacity more important for skeletal adaptations) determined bone strength in postmenopausal women. Maximal strength training (MST) is characterized by high loads and fewer repetitions and till date there are no studies that have applied interventions combining heavy loads with high concentric acceleration as in MST promoting both 1RM and RFD improvements. The study below focused on the effect of squat exercise on MST on 1RM, RFD and bone-related parameters in patients with osteoporosis and osteopenia. 21 participants all of whom were at least 2 years postmenopausal, <75 years and having a BMD score between -1.5 and -4.0 at the lumbar spine, hip or neck were randomly assigned to either the training group (TG, n=10) or control group (CG, n=11). Participants in the training group followed a training program that comprised of MST for 12 weeks with 3 exercise sessions per week amounting to 36 sessions totally. The training sessions consisted of one exercise which used the lower extremities in a squat exercise machine-it started with a warm up including 2 sets of 8-12 repetitions at approximately 50% of the participant’s training load followed by 4 sets of 3-5 repetitions at 85-90% of 1 RM. The training load was increased by 2.5 kg if the participants could perform >5 repetitions. Each of the participant’s vitamin D levels were measured and treadmill tests were performed to define aerobic capacity among participants. The research team was left with 16 participants with 8 of them in each group completing the study. Results showed that:
We have studies showing that performing resistance exercises (REs) 2-3 times per week for a year maintained or increased BMD at the lumbar spine and hip in postmenopausal women. Combining RE and weight-bearing aerobic exercises improves musculoskeletal outcomes including BMD, muscle mass and strength in older men as well as women. Another study with an 18-month RE and weight-bearing impact activity showed significant increase in bone strength and BMD in middle-aged men and women. A systemic review and meta-analysis on the effects of exercising on postmenopausal women suggested that exercise decreased bone mass loss. Performing exercises to build and maintain muscle mass and strength leads to stronger bones which in turn help in minimizing risk of fractures due to osteoporosis. References Preventing Osteoporosis the Bone Estrogen Strength Training Way: https://journals.lww.com/acsm-healthfitness/Fulltext/2007/01000/Preventing_Osteoporosis_the_Bone_Estrogen_Strength.8.aspx?WT.mc_id=HPxADx20100319xMP Maximal Strength Training in Postmenopausal Women with Osteoporosis or Osteopenia: https://journals.lww.com/nsca-jscr/Fulltext/2013/10000/Maximal_Strength_Training_in_Postmenopausal_Women.32.aspx Effects of Resistance Exercise on Bone Health: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6279907/pdf/enm-33-435.pdf Nutrient insufficiency is omnipresent. There are not many who have a healthy stock of all the required nutrients in the body and those suffering from deficiencies mostly rely on supplements to fulfil their needs. Physicians generally recommend patients to eat a well-balanced diet that’s replete with nutrients and even suggest a list of fruits, vegetables and other foods that are enriched with the nutrients missing in their body. But mankind has always been lazy to incorporate ideological ways depending mostly on shortcuts to fulfil most of their requirements. Even supplements came into existence only due to our inadept handling of our food habits.
Fruits and vegetables have always been our holy grail to health. We also depend on other foods such as dairy, fats, whole grains, nuts, seeds and legumes to fulfil all our nutrient needs. The list seems to be in total contrast of the junk food list that makes our mouth water even when we are simply reading it. So, how do legumes and pulses fare in our list of daily food recommendations? Make Some Room for Legumes in Your Diet Legumes in general, especially soybeans, are extremely rich in iron and ferritin content. They constitute a major portion of the diet for a large section of the human population and germination enhances the iron bioavailability of soybean. Iron is available as heme and non-heme iron in animal- and plant-based products respectively. While heme iron is easier to absorb non-heme iron is less readily absorbed by the body. Soybeans are a potent non-heme iron source that’s been increasingly consumed these days for its potent iron composition. Women in general suffer from anaemia problems and they mostly blame it on their menstruation cycle for this as they lose ample blood every month. Otherwise too the human population is not a big fan of iron adequacy as most people including infants, kids and the elderly suffer from iron deficiency. Suggesting such people to eat pomegranates, dates or beetroot is not something new but again have we ever followed any of the nutritional guidance given by others? Definitely not. Meta-analysis on the Effect of Fortified Soybeans on Infants Malnutrition and stunting are common problems in infants worldwide and China is no exception. Its been shown that infant malnutrition-related to stunting and anaemia are two of the commonest problems reported in infants and young children (IYC) in poor rural regions of China. Such unmatched nutrition levels elevate the risk of infectious diseases, cognitive disorder and chronic diseases as they grow. Statistics by the National Nutrition Survey show that anaemia rates in 0- to 6-, 6- to 12-, and 12- to 24-month-old IYC was 23.4%, 28.5% and 15.7% respectively with rates exceeding 40% in 6- to 24-month-old IYC in some regions of the country. Its saddening to see that some newborn babies suffer from such complications soon after birth. At the same time, we need to come up with effective solutions to end this problem. Complementary food feeding is the best way to tackle stunting and anaemia in YIC. WHO reviewed the effects of micronutrient powder (MNP) on IYC revealing that MNP did improve haemoglobin concentration but did not do anything with regard to stunting. Ying Yang Bao (YYB) is a soybean powder product enriched with vitamins and minerals often used as an MNP in China. It is commonly used as a complementary food containing protein and fat largely provided to infants in poor, rural regions of China. We have a number of studies probing into the effect of YYB on reducing infant malnutrition-related stunting and anaemia but results are contradictory. So, a group of researchers were determined to find the exact effect of the supplement on rural infants. They searched databases such as Central and Medline using several text terms such as Ying Yang Bao, anaemia, complementary food supplement, growth, development and so on to identify potential research materials. Different eligibility criteria were imposed, randomized and quasi randomized trials were included and all the participants were healthy boy and girl IYC anywhere between 6 and 24 months without any health problem at the time of intervention. The researchers defined anaemia as haemoglobin values lower than 110g/L and stunting as having a z score <-2.0 for height for age. Underweight is defined as having a z score <-2.0 for weight for height. Results The database came up with 17340 publications from which only 22 articles were selected after imposing all the eligibility criteria. Again, 5 studies were excluded due to incomplete information available and the remaining 17 studies were included in the meta-analysis. All the studies included YYB durations between 3 and 18 months, sample size was between 76 and 2183, 8 of them were parallel control trials and 16 were before-after control trials. Haemoglobin Concentration YYB vs No-intervention Studies There were 6 studies having 9 subgroups involved in this specific study containing a total of 4929 participants. YYB supplementation resulted in increased haemoglobin concentration when compared to the control group and the changes were significant across subgroups. Before-after Studies This included 10 studies with 15 subgroups with a total sample size of 15897 (8269 participants before and 7628 participants after study). Significant increase in haemoglobin concentration over baseline was visible in the studies after YYB supplementation. All the studies had a follow-up period either above or below 12 months and across these periods too the results remained significant. Anaemia Rate YYB vs No-intervention Studies This included 7 studies with 12 subgroups with a total sample size of 11027 and YYB supplementation decreased anaemia rates across the intervention group in all the study participants in comparison to the control group. Before-after Studies 13 studies with 20 subgroups were included here with a sample size of 26496. Subgroup analysis showed that anaemia rate was lower after YYB intervention compared to baseline and the results remained the same even after excluding two studies after they displayed low quality. Stunting YYB vs No-intervention Studies Four trials were included and they showed 47% reduction in stunting after the kids were fed with YYB. Before-after Studies 12 subgroups were included here with 7536 participants before and 7895 participants after the study. While stunting effects were significantly decreased after providing YYB supplementation there was no effect of the supplement found in the subgroup under 12 months. Underweight YYB vs No-intervention Studies Two trials with a sample size of 885 were included here where underweight prevalence decreased by as much as 46% compared to the no intervention group. Before-after Studies This analysis included 10 trials with a sample size of 7599 participants (3996 of them before study). Feeding the participants with YYB decreased underweight rates as much as by 51% and the results remained the same even after excluding 2 studies due to some reasons. Wasting YYB vs No-intervention Studies Two trials with a sample size of 885 were included here but the supplement had no effect on wasting prevalence rates. Before-after Studies 7 trials with a sample size of 5376 (2835 before and 2523 after) were included here and YYB supplementation showed significant decrease in wasting prevalence compared to baseline. Results showed no differences even after excluding a study. YYB is an effective means to reduce anaemia, stunting and underweight in IYC. A study conducted in Guatemala in kids 2 years and above showed that consuming a supplement with high protein and energy content helped the kids score more in reading, math and other cognitive skills compared to those who did not consume such nutrients. Pollitt et al. conducted a follow-up study on kids aged under 18 months and found that after their 8th birthday these children showed better memory capability that those in the control group. This clearly shows that giving food supplements during appropriate periods of the kid’s growth and development has a long-term impact on their intelligence. References Supplementing Fortified Soybean Powder Reduced Anaemia in Infants & Young Children Aged 6-24 Months: https://www.sciencedirect.com/science/article/pii/S0271531718307553 Ageing is inevitable marked by deterioration in the functioning of cells and tissues. All of us age but how we age and the event as such is genetically-based and greatly affected by the surrounding environment too. The outline is clear but what causes these irreversible changes remains a mystery and understanding the ageing process might help to modify its effects. Immunosenescence is the gradual decline in immune function with ageing which is affected greatly by the composition of the gut microbiota; it can also be changes in the function or proportion of leucocytes that are potential sources of inbuilt immunity to the body. Ageing or rather aged people comprise of a majority of the world population who are sometimes overloaded with diseases and infections probably due to compromised immune systems.
The gastrointestinal tract (GT) is composed of bacteria that propagate immune cell maturation. The gut microbiota safeguards the intestine against colonization by pathogen by modulating host immune response. The functioning of the gut microbiota depends on the composition of the gut and any reduction in its diversity that happens as a result of ageing is seriously linked to frailty, infection susceptibility, inflammatory disease and increased morbidity. Each of our immune systems undergo definite changes with ageing specifically related to polymorphonuclear (PMN) cell phagocytic capacity and natural killer (NK) cell function. The PMN cells that initiate immune response to infection clearly display decreased functionality in older adults. Quantity doesn’t matter everywhere and this is once again proved by the NK cells which increase in numbers in the aged adults but their signalling efficiency and cytokine production decrease resulting in a net decrease in function. So, reinstating PMN and NK cell functionality is a sure-shot way to fight age-related immune function decline. Probiotics: The Key to the Immunity ‘Cell’ We are all smart enough to understand that each of us grow old and die but what we strive to achieve is to make the ageing process as comfortable as possible optimizing quality of life. With ageing comes the risk of osteoarthritis, dementia, emphysema and heart problems; the gut too contributes to numerous problems many of which can increase morbidity rates. The ageing gut leads to overexpression of proinflammatory cytokine IL-6 that impacts performance of the immune system and intestinal barrier function also increasing the risk of cancer development and progression. Changes in intestinal permeability results in the progress of local (celiac disease, cancer and inflammatory bowel syndrome) and systemic diseases (obesity, diabetes, heart disease, etc.) which shows that protecting the intestine and preserving its health helps to improve quality of life in ageing adults. One of the effective means to restore immune system functioning is through dietary intervention. Dietary restriction exists as one of the most researched and promoted nongenetic intervention in the ageing process, specifically its impact on the gut microbiota composition and inflammation. Taking up a healthy lifestyle with diets customized for the aging population that includes a good share of probiotics helps in decreasing inflammation and other age-related changes. Probiotics are live microorganisms which on administering in appropriate doses shower the host with benefits. If you notice, many of the probiotic bacteria are of the intestinal type introduced into the body through foods to improve gut health. Avoiding diarrheal diseases, increasing intestinal barrier function and improving inflammatory intestinal disorder and age-related immunological functions are some of the commonest advantages of consuming probiotics but we have not explored much about the effects of probiotics on intestinal barrier and immune function. Two of the commonest bacteria found in human gut as well as food supplements include lactic acid bacteria (LAB) and bifidobacterial whose immunomodulatory properties are fully utilized in severing age-related disorders. Various human studies showed the ability of participants to fight infections following probiotic consumption. Administration of certain strains of these bacteria increased cytotoxicity of NK cells in elderly women, reduced length of winter infections compared to control group and also nutritional and immunological status of subjects. Isoflavones, ageing and probiotic bacteria: Isoflavones found in foods such as soy offer protection against certain diseases. LAB and bifidobacteria transform naturally occurring isoflavones to their bioactive form. Lignans, ageing and probiotic bacteria: Though lignans are one of the major phytoestrogens occupying a major part of our diet plant lignans cannot be absorbed directly and must be metabolized to enterodiol and enterolactone before being absorbed. Deglycosylation of the secoisolariciresinol diglucoside (SDG) present in the lignan extracts into secoisolariciresinol (SECO) is the first step towards the formation of enterolignans. SDG hydrolysis that’s possible due to probiotic bacteria helps in the release of SECO. Meta-analysis of Controlled Studies to Evaluate the Effect of Probiotics on Immune Activity Databases such as Embase and Medline were checked using certain keywords for prospective studies on PMN cell phagocytic capacity or NK cell tumoricidal activity after consumption of probiotics in healthy older adults aged 60 and above. The team came up with 459 titles and abstracts but after imposing several other restriction criteria only 17 studies were included for analysis. There was a total of 733 subjects most of whom were healthy and predominantly females. There was a total of 13 different probiotic strains that was investigated in the studies. Of the 17 studies taken into account, 10 were randomized, 12 included patient blinding, phagocytic capacity was reported in 9 studies and NK cell activity was reported in 14 studies. Results showed that:
Effect of Bifidobacterium Lactis on Immune Functionality A dietary trial invited elderly people in which 30 (12 men and 18 women) of them aged 63-84 years enrolled. After imposing inclusion criteria such as good health, mobility and a willingness to follow trial guidelines, and exclusion criteria such as recent history of acute or chronic debilitating illness and intolerance to milk products each of the participants were given low-fat milk (LFM) low in lactose in powdered form. B. lactis strain was obtained and Lyophilized bacteria was mixed with the powder to come up with two different doses-a typical dose and a low dose. Each of the participants was randomly assigned into one of the two groups (each group contained 15 participants). The diet was packed into sachets containing either the LFM powder or the B. lactis HN019-supplemented LFM powder. All the participants consumed the entire contents of the sachet by mixing it in 200 mL of cool drinking water. The trial was split into three stages with the first stage supplementing the subjects with unsupplemented milk twice a day, during the second stage they consumed milk supplemented with B. lactis HN019 (6 men and 9 women consumed a typical dose while 7 men and 8 women consumed a lower dose). During the third stage all of them consumed unsupplemented milk. Each of them was also enquired on their general health every time their immune measurement was taken. All of them were subjected to blood sampling four times during the trial- at week 0, at the end of week 3, at the end of week 6 and at the end of week 9. Results Of the 30 participants one participant withdrew quoting dislike of the milk’s taste and other digestion-related problems. Between-group analysis showed not much difference between the low-dose and typical-dose group but there were time-dependent treatment effects within both groups. While no difference was recorded between time points 1 and 2 there was significant change recorded for immune variable between time points 1 and 2 and time point 3. While previous studies reported that dietary supplements were effective at increasing proportions of T lymphocyte subsets and enhancing NK cell functioning the present study clearly showed similar changes in cellular immunity after participants consumed the milk-based dietary supplement containing B. lactis HN019. Drinking B. lactis HN019 increased the presence of total, helper and activated T cells in the peripheral circulation and helped to significantly improve immune cells population that might facilitate health improvements in elderly. Maximum immune function due to B. lactis HN019 consumption occurred in those individuals who had poor pre-intervention immune responses revealing that B. lactis HN019 maximum benefited those with poorly functioning immune system even at a potentially low dose. B. lactis HN019 supplement is a good way to combat the effects of immunosenescence. How Do Probiotics Stimulate the Immune System? Probiotics deliver better health by inhibiting the growth of pathogenic bacteria. This is done by their active competition for nutrients (for growth and proliferation) which would otherwise be used by pathogens. Probiotics can withstand gastric juice and bile salt, multiply and function in the gut while some microbes that claim to be probiotics cannot withstand the acidity level of the gastric juice and bile salt. Another important trait for the probiotic to work properly is its ability to stick to epithelial cells. A study by Galdeano et al. showed that two microorganisms stick to intestinal epithelial cells (IECs) through toll-like receptors (TLRs) and mediate immune stimulation. Rather than the whole bacteria only fragments of the probiotic were internalized inside the IECs. The IECs in turn stimulate immune cells associated with the lamina propria, activate the innate response and cytokines released by T cells. There are several other studies that have shown positive effects of probiotics on reinstating intestinal barrier integrity through increased gene expression. Recently, there has been an increased interest shown over probiotic fermented milk (PFM). Fermentation helps in improving digestibility and nutritional quality of food. Probiotics also stimulate systemic immune response with an increase in specific antibiotic production. Our eating habits and lifestyles change as we grow old and age-related changes in microbial diversity makes the elderly population at a risk of diseases and infections. Enhancing immune response by incorporating beneficial microorganisms in the gut helps these people avoid some of the age-related diseases. References Short-term Probiotic Supplementation Enhances Cellular Immune Function in Healthy Elderly: Systematic Review & Meta-analysis of Controlled Studies: https://www.sciencedirect.com/science/article/pii/S0271531718307978 Enhancement of Immunity in the Elderly by Dietary Supplementation with the Probiotic Bifidobacterium Lactis HN019: https://pdfs.semanticscholar.org/82dd/ed8dd509a95dc7a8f26ef242ec802d292156.pdf Beneficial Effects of Probiotic Consumption on the Immune System: https://www.karger.com/Article/FullText/496426 Probiotic Bacteria for Healthier Ageing: Immunomodulation & Metabolism of Phytoestrogens: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5646295/ Old habits die hard, superstitions stay longer. Most individuals grow up having certain beliefs and sentiments that they strongly cling onto most times. Such sentiments are even stronger for sports personalities, celebrities and politicians who stick by certain principles believing it to bring about good luck. Common man too has a few ones on his own and the most common of them is to never allow a cat cross across your path! When it comes to health too, we have our own perceptions-some wear the same colour dress while going for a blood sugar test and some others believe that weather changes increase the degree of pain in individuals with osteoarthritis. They are even super confident about this, challenging physicians that they can predict the weather reports even better than the meteorological department but science has always doubted this belief and even research doesn’t support this.
Sophisticated medical equipment and latest technological skills equip physicians to save as much life as possible but the common man finds it assuring and satisfying to rely upon his/her proposed theories finding comfort in their own assessment. The anecdotal link between weather and pain remain unaffected by these sophistications in technology but researchers continue to figure out the weather sensitivity in people with arthritis-results are still inconclusive till date. Weather & Knee Osteoarthritis Pain due to osteoarthritis is episodic and patients often complain that weather changes in terms of chillness, air humidity and barometric pressure have the capacity to increase it. Patients with other chronic conditions have reported in similar lines and has been even more dominant in those residing in places where climate changes are frequently experienced. We do have studies supporting the link between arthritis and climate change but the magnitude of association was not clearly stated and pain levels were decided only depending on self-reports rather than scientific measurements. A study by Timmermans et al. has shown a weak but significant link between humidity and joint pain but no positive relationship between temperature and pain in direct contrast to the study by McAlindon et al. who showed that changes in temperature and atmospheric pressure increases pain intensity in people with knee osteoarthritis. A research team in Australia conducted a web-based case-crossover study to study the increase in osteoarthritic pain due to weather changes. Online ads for participation was posted and individuals were also invited using database of participants of previous studies on knee arthritis. A total of 345 of them were recruited using inclusion criteria such as minimum age limit of 40 years, suffering from knee pain at least 5 times/week with fluctuating intensity, must meet at least one of the American College of Rheumatology criteria for knee osteoarthritis, suffer from tibiofemoral or patellofemoral osteoarthritis and should be able to access the internet. All the participants were clarified on the goal of the study-to be able to find out the trigger factors, specific weather factors, that could aggravate pain. Each participant was asked to fill an online questionnaire on demographic and clinical data at baseline and every 10 days up to 90 days of study. They were asked to quote when the knee pain was minimal, when it was moderate and when it soared to maximum before start of study. During study, each of them were asked to enter details in the study website whenever they experienced debilitating knee pain that lasted for more than 8 hours. Increase in pain levels were measured via a Pain Numeric Rating Scale (NRS 0-10) defined as an increase of ≥2 on a 0-10 NRS in comparison to the mildest pain at baseline. ‘Pain at its mildest’ was used as the basic platform for comparison and participants were asked to provide zip codes of their location when they experienced knee pain exacerbation. The team defined hazard and control periods based on their previous research of gout risk that changed with weather and index data was calculated based on them for making assessments. Climate data was procured not only for the specific period but for 3 days preceding the index data as exacerbations don’t occur instantly after exposure to a specific weather. Results Of the 345 included 174 of them did not experience any pain exacerbation during the study period and hence were excluded from the analysis. The effect was finally studied on the remaining 171 participants (aged around 60 years with 64% belonging to the female gender) who contributed to a total of 404 counts of pain exacerbation (hazard periods) and 1021 control periods. Each of those participating suffered from knee osteoarthritis for 10.5 years with the mean age of diagnosis around 51 years. It was mostly the right knee that frequently remained as the commonly symptomatic knee. At the start of study all the participants reported their pain intensity to be around 4.9 that increased to 8.3 when it was worse reducing to 2.9 when it was mildest. The average exacerbation intensity reported was 5.9 on the 10-point scale. Surprisingly, high temperatures 3 days before index date prompted increase in knee pain exacerbation. For instance, compared to 10-20-degree temperature measures the risk for increased knee pain increased, almost doubled, for temperature measures of 30 degree and above. But there was no link seen between other weather factors such as relative air humidity, precipitation and barometric pressure and knee pain increase risk. The study shows that despite repeated insistence by patients that weather changes affect pain intensity the results here show that weather factors don’t affect pain intensity in any way. Pressure & Temperature Changes Influence Osteoarthritis Pain A study on 205 participants with confirmed knee osteoarthritis focused on the relationship between arthritis pain and meteorological conditions. Each of them belonged to different parts of USA and also participated at different times of the year. The fact that weather influence was a part of the research was publicised to the participants only after the study to avoid any report bias. The studies focused on the relationship of pain with weather not only with ambient conditions but also with changes in conditions immediately before any pain report was delivered. Pain assessment was made using questionnaires given every 2 weeks amounting to 7 assessments with scores between 0 and 20 reporting different pain levels experienced during different daily activities. Meteorological data was also collected. After imposing inclusion criteria 200 individuals were eligible for participation, their mean age was around 60 and more than 60% were females. Baseline pain score was around 9 and they provided a total of 935 pain reports. Results showed that both, barometric pressure and ambient temperature had insignificant effect on pain exacerbations. For instance, a temperature of 10 °F decrease increased knee pain score of 0.1. The study also noted that increasing barometric pressure was associated with increased pain. A study by Wilder et al. on 154 individuals with osteoarthritis showed positive associations with days of rising barometric pressure in the participants. But another study by Strusberg et al. found a positive link between pain and low ambient temperature but observed no impact of pressure. The researchers of the present study found their results to be similar to that of another researcher, Hollander who suggested that increase in humidity following a decrease in barometric pressure increased pain, swelling and stiffness in those suffering from arthritis. Yet another study by Barrett et al. on participants aged 49 years and above also did not support the assumption that weather changes including barometric pressure, precipitation and temperature had any effect on pain intensity in patients with arthritis. All these contradictory results against weather impact on pain levels make us wonder whether people have got it wrong or if they are the exceptions. But I have seen my own mother suffering from increased pain in her joints during winter! Its hard to let go of this theory when there are thousands of people reporting changes in pain intensities linked to weather changes. Could they all be an exception? Hardly! So, have researches always excluded these exceptions while conducting their studies? Science is showing us with hard-core facts that there is no link between weather changes and pain intensity changes in those suffering from osteoarthritis. On one hand we believe in our people and on the other hand we definitely believe in scientific evidence. While trust makes us support these people with arthritis who blame weather on increased pain levels we cannot come to definite conclusions unless we have more compelling evidence scientifically. References The Influence of Weather on the Risk of Pain Exacerbation in Patients with Knee Osteoarthritis: https://www.sciencedirect.com/science/article/pii/S1063458416302059 Changes in Barometric Pressure and Ambient Temperature Influence Osteoarthritis Pain: https://www.amjmed.com/article/S0002-9343%2806%2901026-6/pdf Osteoarthritis Pain & Weather: https://academic.oup.com/rheumatology/article/42/8/955/1774101  Cortisol Levels Generally Rise after Exercise Cortisol Levels Generally Rise after Exercise For most, mornings are the busiest time of day and I feel today morning would have been no different. We are enveloped by stress and lack of time that’s become our daily routine almost every day. So, while all of us know about stress not many are aware of the science behind it. Our body releases cortisol, often known as the ‘stress hormone’ due to its connection to stress response, which helps in preparing the body for physical and mental stress by acting within the physiological processes. It also plays a critical role in the functioning of the body by affecting macronutrient metabolism, regulating water and electrolyte balance, blood pressure, body temperature and immune response. Your mood, behaviour, pain and appetite changes are the work of this hormone. All these functions make the cortisol hormone indispensable for good health and well-being. Maybe changes in the hormone levels can answer our lingering doubts why some people are always moody, anxious, stressed or even hungry! Cortisol is secreted in the body in the adrenal glands but is controlled/regulated by the hypothalamus, the pituitary gland and adrenal gland and their combination is often called the hypothalamus-pituitary-adrenal axis (HPA axis) which is involved in important functions such as regulating mood, sexuality, body temperature, digestion and energy use. The HPA axis is also one of the components of the fight-or-flight response. Triggering Agents for Cortisol Production Our food supplies us with the required nutrients and energy for proper functioning of the body but all this is possible only when we consume a well-balanced diet. Cholesterol helps in cortisol production through triple enzymatic hydroxylation. Liver is the primary source of cortisol metabolism and its secretion is affected by a variety of factors including circadian rhythm, negative external stimuli and feedback regulation. In times of stress the hypothalamus releases corticotropin-releasing hormone (CRH) and vasopressin (ADH, antidiuretic hormone). This in turn triggers the pituitary gland to produce the adrenocorticotropic hormone (ACTH). ACTH impacts StAR protein which helps in transporting cholesterol thereby encouraging cortisol formation in the adrenal cortex. Once cortisol is released its impact on the body and our response entirely depend on the concentration of the hormone, timing of cell cycle and presence of endocrine disorders. Important Functions Besides performing the above-mentioned functions cortisol also influences insulin resistance, dyslipidaemia, hypertension and obesity. Above all, it has a strong impact on appetite. A study by De Sa et al. showed that administering cortisol orally influenced the participants to be highly responsive to those foods presented with high glycemic index but the same response was not given when they were shown a couple of other normal non-food images. Presence of ghrelin, the hunger hormone, increased cortisol levels greatly. Abnormally high or low cortisol concentrations have been commonly linked to upper body fat leading to what’s known as Cushing Syndrome. This syndrome is characterized by rapid weight gain in the face, abdomen and chest besides causing a flushed face, high blood pressure and changes in the skin. Collagen synthesis stimulated by cortisol is inhibited when an individual is under too much stress or performs vigorous physical activity due to interruption of bone mineralization. Cortisol might enhance sensitivity of tissues of blood vessels and heart to noradrenaline, vasopressin and angiotensin II thereby leading to higher blood pressure levels. It also affects immune system in the form of hydrocortisone-it shows anti-inflammatory and immunosuppressive effects by disrupting the production of inflammatory cytokines, migration of WBCs to inflammatory sites and inducting cell apoptosis. By doing this, cortisol protects our body in times of injury being especially useful in the case of athletes involved in sports. Studies have shown that athletes who are highly motivated and successful show higher presence of the cortisol hormones in their body. Likewise, levels of cortisol hormone also influence the emotional feelings experienced during the start of a competition and also the degree of burden that they carry around before, during and after the competition. After completion of an athletic event or exercise, the cortisol levels vary depending on the fitness of the individual, his/her training duration and compliance to regular training. Effects of Dietary Intake on Cortisol Levels Our diet talks about our health. The food we eat, the nutrients we consume and the quantity of these influence the functioning of the body which includes the endocrine system as well. The type of carbohydrates we eat and how much of it we eat actively affect the endocrine system. Hence, before, during and after exercise or sports training it is imperative for individuals to replenish energy stores by taking appropriate carbohydrates. Many individuals these days take dietary supplements alongside a well-balanced diet to maintain the nutritional requirements of the body. We can see an increasing number of elderly people, athletes and heavy workload people using nutritional supplements to improve their overall efficiency and functioning. These are one of the groups of people who are highly susceptible to increased secretion and metabolism of hormones including cortisol. So, consuming dietary supplements helps them in stabilizing the effect of these hormones. For instance, cortisol levels might increase after exercising and supplementing the body with certain amino acids such as tryptophan decreases cortisol levels. One should carefully choose the supplements with the help of physician’s guidance-supplementing with amino acids such as glutamine and arginine have no impact on cortisol concentration. Phospholipids too regulate cortisol levels and the best of them include phosphatidylserine and phosphatidic acid. But studies have shown that supplement dosage plays a great role in bringing about changes- a 400mg/day dose administered for 6 weeks reduced cortisol levels incremented due to exercising while consuming a 200mg/day dose had no significant effects. Protein-enriched products such as egg yolk are great sources of these phospholipids, yet another reason why we are always suggested to consume a protein-enriched diet. Fermented milk products, sprouts of brown rice, barley and beans can be consumed generously as these help in controlling cortisol release with the help of a chemical compound called GABA (gama aminobutyric acid) present in each of them. Besides foods, yoga has been proclaimed as one of the best ways to increase GABA concentration in brain. Studies Supporting Supplement Intake We have had numerous studies trying to understand the effect of ascorbic acid (vitamin C) intake on cortisol synthesis. A study by Brody et al. showed that consuming 3000 mg of vitamin C daily helps in cortisol recovery after psychological stress but does not contribute towards lowering cortisol levels. We have other studies showing that consuming high dosages of ascorbic acid (1000-1500 mg/day) before the start of an athletic session helps in restricting increasing cortisol levels, decreases muscle pain and facilitates efficient regenerative processes. Similar effects were observed for supplementing the body with vitamin B1, B2 and niacin. Vitamin D has always been mysteries and in the case of cortisol too the results have been controversial. It has been well-known that exercise increases cortisol levels but a study by Golf et al. showed that supplementing our diet with magnesium inhibits exercise-induced increase in cortisol levels. But another study by Cinar et al. showed that magnesium supplements in combination with physical activity increased cortisol concentrations. Even vitamin E and omega-3 are proposed to be cortisol-lowering supplement aids but we don’t have authentic scientific evidence to support this. But a 3-week supplementation of fish oil helps in reducing cortisol and stress levels. Coffee and tea have been always consumed in times of energy needs. A study by Arent et al. showed that consumption of black tea extract enriched with theaflavin helps reducing cortisol levels caused by stress and so does oolong tea. Contrarily, black coffee stimulates hydrocortisone secretion. The presence of caffeine in coffee prevents decrease in cortisol levels. Having caffeine before a workout leads to dose-dependent increase in cortisol and testosterone concentrations. Studies on individuals who consume drinks containing carbohydrates and caffeine during workout shows that maximum increase in cortisol levels was seen in the group supplemented with caffeine without carbohydrates. Study by Miyake et al. showed that supplementation with L-ornithine reduced serum cholesterol levels besides reducing anger and improving sleep quality. A 4-week supplementation of extracts found in the roots of Eurycoma longifolia (Malaysia ginseng) helped in reducing cortisol levels by 16% and increasing testosterone levels by 37%. Intake of enzyme-treated asparagus extract prevents cortisol increase and also raises sleep quality. Vitamin D’s Impact on Cortisol Levels Vitamin D deficiency is prevalent worldwide right from youngsters to elderly people. Chronic stress prevents the body from accepting stress challenges and this is termed as allostatic load which impairs normal levels of stress mediators such as cortisol (CORT). Changes in cortisol levels have been associated with a number of factors and the recent has been links between vitamin D deficiency (VDD) and lifestyle stressors. There has been an inverse association noticed between serum 25 (OH) D and postpartum allostatic stress and another similar one seen in preeclampsia patients too. Studies dealing with VDD’s link with stress has been inconsistent. Vitamin D3 supplements suppressed HPA-axis activity. While it was positively linked to coffee consumption in Koran participants another study in Saudi Arabia excluded coffee consumption as a contributing factor for VDD. Though we have a few studies linking VDD with obesity biomarkers such as hip, waist, weight and BMI we don’t have definite results relating VDD to lifestyle stressors. A study tried to analyse the relationship between VDD and lifestyle stressors in healthy Jordanians. The study included male and female Jordanian Applied Science University students and their Anthropometric and lifestyle habits were noted with the help of a questionnaire. There were 371 participants who were eligible for analyses. Their serum 25(OH)D levels, serum CORT levels and serum PTH levels were measured using different techniques. All the participant were between 17 and 52 years of age and their mean serum 25(OH) levels was 12.2 ng/mL and this is classifiable under vitamin D deficiency. PTH, ionized calcium and phosphate besides serum morning cortisol were within physiological limits. 72% participants were females and some of the common positive traits observed among most of the participants in the study includes adequate sleeping hours during night, morning sun exposure, non-smokers and living with their family. Anthropometric parameters showed very weak positive correlation with VDD, a poor correlation was seen between vitamin D levels and exposure to sunlight, larger number of family members implied severe VDD levels, LDL-C and TC showed a weak correlation with VDD severity. Cortisol & Weight Changes Stress rules the world, it rules our actions and even the choice of our foods. Effect of stress varies depending on the type and duration of stressors. Acute stress (developed as a result of exposure to some traumatic event) supresses appetite while chronic stress increases hunger and intake of high-fat and energy-dense foods. Chronic stress has been linked with obesity/overweight issues in a number of studies. Effects of chronic stress has been linked to disturbances in the HPA axis due to which cortisol hormones are secreted. This secretion triggers hunger hormones and increases intake of high-fat foods. The clear link between food cravings, stress, cortisol and appetite-inducing hormones are not understood until now. A group of researchers tried to understand whether increased chronic stress, cortisol and appetite-related hormones triggered food cravings and weight gain. 339 participants aged between 18 and 50 years who were not pregnant, taking meds for any psychiatric disorders or suffering from chronic medical conditions were involved in the study. All of them underwent a biochemical evaluation after overnight fasting, psychological measures and a self-report questionnaire. Height and weight were measured at baseline. Chronic stress was measured using a 62-item questionnaire in which items were rated as not true, some to very true. Questions included those on relationship with family, difficulties in work and home environment, etc. Food cravings were measured using a 28-item questionnaire rating each food on a scale of 1 (never) to 5 (always/almost every day). Items were split into four sub-categories-sweets, high fats, carbohydrates/starches and fast-food fats. Results Among the 339 participants almost 57% were females. Males had increased cravings for high fats and had high glucose levels. Females had higher ghrelin, leptin, cortisol and chronic stress besides cravings for sweets. Baseline BMI was positively associated with total and specific food cravings. Total food cravings were positively associated with leptin, insulin and glucose. Morning cortisol was inversely linked to chronic stress, cravings for high-fat foods, leptin and insulin. Leptin was positively associated with total food cravings. Cross-sectional model did not show any association between cortisol, chronic stress and weight. But cortisol, leptin, insulin and stress did not predict changes in food cravings over time. Of the total participants almost 50% of them gained weight over the 3-month study period. Individuals with higher baseline cortisol gained an average of 1.12±0.33 kgs while those with a lower baseline cortisol gained 0.530.37 kgs. It was observed that higher baseline cortisol, insulin and chronic stress implied greater weight gain from baseline to 6 months. Hence, it is imperative that each of take care and eat well to optimize cortisol levels in the body. It is an essential hormone which works wonders when the levels are balanced but which also has the ability to create tremors when the levels go too low or high. References The Effect of Diet Components on the Level of Cortisol: https://link.springer.com/article/10.1007/s00217-016-2772-3 Correlation of Selected Stress Associated Factors with Vitamin D Deficiency in Jordanian Men & Women: https://www.dovepress.com/correlation-of-selected-stress-associated-factors-with-vitamin-d-defic-peer-reviewed-fulltext-article-IJGM Stress, Cortisol and Other Appetite-related Hormones: Prospective Prediction of 6-Month Changes in Food Cravings & Weight: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5373497/ What is Cortisol? https://www.hormone.org/your-health-and-hormones/glands-and-hormones-a-to-z/hormones/cortisol Ageing is inevitable and remains the most familiar aspect of human biology. Almost 1/5th of the human population would be individuals aged above 60 by 2050 as the average life expectancy has drastically increased during the last couple of decades. How we age is a matter of concern here as ageing is often accompanied by metabolic disorders such as diabetes and health problems, atherosclerosis and neurodegenerations. Enormous research on ageing that has resulted in finding pharmacological agents that can extend lifespan and healthspan shows that ageing is malleable. The main issue that remains here is to live a longer life that’s devoid of age-related functional decline and fragility that includes diseases such as cancer. Cancer causes millions of deaths annually and in the future one in every eighth person would be a victim of this disease. Ageing can be delayed and so can cancer. Muscle atrophy is one definite side effect of cancer and cachexia (extreme weight loss and muscle wasting) is a positive sign of death in almost 22-40% cancer patients. Presently, cachexia is treated by improving the individual’s appetite with appetite stimulants and protein supplementation so as to supply the patient with nutrients. This, apart from improving chances of survival also improves the chances that the cancer patient withstands treatment procedures successfully. But these treatment procedures including physical rehabilitation and treatment for underlying diseases is not successful and what we need is an effective treatment protocol for correcting muscle wasting that helps in extending both, lifespan and healthspan.
We have always thought of procedures and treatments for inhibiting ageing in individuals which in turn helps to minimize the occurrence of diseases such as cancer. The invention patented here is of utmost use in each of our lives as it provides a method and system for extending healthspan and lifespan of humans as well as for preventing the onset of diseases such as cancer. Delaying ageing process delays/prevents the occurrence of debilitating illnesses such as cancer. The invention here looks at the large picture rather than its pieces in that rather than trying to deal with age-related pathologies one by one the invention tries to overcome age-related pathologies in general. By this, it focuses to bring an overall new approach to the current public health strategy which involves steps taken to prevent illnesses individually which can sometimes leave the patient susceptible to other illnesses in the treatment period. Tomato fruit is mostly consumed by individuals in salads and curries and its consumption has greatly been associated with a reduced risk of inflammatory processes, cancer and non-communicable diseases that includes cardiovascular diseases (CVD such as heart disease, obesity and hypertension. One aspect of the invention uses a natural small molecule that’s been derived from tomato plants, tomatidine, that is associated with cell growth (majorly in skeletal muscle tissue). Basically, tomatidine is an inhibitor of muscle wasting and the invention here looks at providing cancer patients with bacteria that have been modified to produce tomatidine to address muscle atrophy linked to various cancers. Treatment for cancers are also linked to the production of p53, a tumor support factor. In one representation of the invention, cancer treatment was enabled by administering the microbiome of a subject with a bacterial combination that expresses p53 protein and tomatidine as in the case of breast, colorectal, kidney or bladder cancer. Particular agents and certain combinations are administered in various representation of the invention to lessen the occurrence of cancer which is due to the delay of ageing. One such agent is rapamycin (sirolimus), a bacteroid produced by the bacterium Streptomyces hygroscopicus. Administering rapamycin via microbiome helps in fighting against age-related diseases. Rapamycin is an inhibitor of mTOR complex (mammalian target of rapamycin) which is a serine threonine kinase and a regulator of protein synthesis, cell growth and cell metabolism. Excessive mTORC1 activity has been noticed in various types of cancers, inflammatory skin diseases, bowel disease and neurodegenerative diseases. Rapamycin is used in the invention to treat/prevent medical conditions by inhibiting the mTORC1 pathway. Tomatidine and rapamycin both are used to sort out cancer, ageing and cachexia as the former has the ability to preserve muscle mass while the latter reduces growth of muscles (basically prevents the growth of cancer cells). The modified bacteria used in the invention are administered directly though the mouth to deliver the therapeutic directly to the gastrointestinal tract. Shortening of telomers is associated with ageing but trying to rebuild shortened ends using telomerase often results in cancer. Ageing can cause telomer damage in the nucleus which in turn can trigger the activation of p53 that can have different effects on the individual. p53 is a gene that inhibits damaged cells to grow and this gene prevents cancer in younger people but at the same time, it can cause ageing by impairing the body’s ability to renew deteriorating tissues. Physical activity, diet modifications and addressing hormone signaling are all practical ways to extend human healthspan but the problem here is that most individuals don’t follow it. Shortening of telomers and using enzymes to rebuild telomers thereby lengthening the telomers at a risk of cancer is due to the effect of such enzymes on p53 mutation which deprives the individual of the cancer-inhibiting wild-type p53. One representation of the invention looks at producing resveratrol by using an individual’s microbiome to delay ageing as well as treat cancer as it has been viewed to possess antioxidant, anti-inflammatory, anti-apoptotic and anti-cancerous effects. Hence, the basic principle of this invention is to achieve cellular rejuvenation by modifying microbes such that the individual’s own microbiome generates desired combinations of chemicals that extend life and health spans without altering the human genes. The patent was published on December 7th, 2017 and for more details on the patent please visit: Untied States Patent & Trademark Office: http://patft.uspto.gov/netacgi/nph-Parser?Sect1=PTO2&Sect2=HITOFF&p=1&u=%2Fnetahtml%2FPTO%2Fsearch-adv.htm&r=32&f=G&l=50&d=PTXT&S1=(Kovarik+AND+cancer)&OS=Kovarik+AND+cancer&RS=(Kovarik+AND+cancer) World Intellectual Property Organization: https://patentscope.wipo.int/search/en/detail.jsf?docId=US206640361&_cid=P20-JYIL0P-06069-1 Irrespective of the type, duration and frequency of an activity performed any physical activity is sure to reap benefits for the person performing it. Each of us are struggling hard to squeeze in some time to fit in physical activity in our daily schedules somehow and the benefits incurred are regardless of whether it occurs as part of work, leisure, transport or housework. Walking was the only means of transport earlier and after the introduction of wheel, mankind progressed towards other means of transportation. Bicycle, an integral innovation has been also used as an excellent means of exercising since ages. But walking and cycling are activities that can be performed individually. Then how did the group fitness classes evolve? The origin of group fitness can be traced back to 1968 when Kenneth H. Cooper introduced the concept of aerobic exercise. Immediately the following year dance-based fitness classes focusing on cardio, strength and stretch movements were introduced and it was not until early 1970s that Sorensen took a bit of aerobic programs, added some music and made the world become an ardent fan of aerobic dance that now prevails as the basis for group fitness programs these days. Group fitness classes are exercises performed by a group of people in the presence of an instructor attracting people with its different formats available-yoga, aquatic activity, core conditioning, resistance exercise, kickboxing, boot camps and more. There are a number of health centres and fitness clubs that bank on people’s interest to do different activities and their eagerness to have fun that they have reshuffled the entire concept of fitness. Group activities are encouraged these days as they motivate people to be regular for workouts, follow a consistent exercise schedule and reap the benefits of a fun environment. The question now is whether group fitness offers more benefits than individually performed exercises, especially for the elderly. We are witnessing the fastest growth in the ageing population which brings with it a great burden on the society due to increased risk of mental and social health problems that grow alongside physical health problems as well. There is a dire need to promote physical activity among older people as its absence increases the risk of chronic degenerative diseases and disabilities. Ageing is by itself a risk factor for decline in daily functionality and mobility whose effect can be controlled with daily physical activity and exercise schedules. In such cases regular physical activity increases muscle strength, coordination and flexibility but to avail these benefits it must be performed regularly. But one requires knowledge, skills and perseverance for reaping the benefits of exercising. Don’t we see a group of elderly adults, men mostly, in parks going for a walk or a slow jog as well? These people enjoy each other’s company and have fun while exercising too. But the population of older adults is heterogenous as each of them have varying degrees of health, culture, attitudes and practices. Viewing them as one group might hamper us from providing the needed healthcare as it is essential to consider each of the elderly person’s individualized needs. How good can group exercising benefit older adults in such a scenario and what’s the impact of group exercising on the elderly population? Advantages of Regular Group Exercising in Elderly in Japan Japans prevails as the most rapidly aging country in the world where by 2035 one in every three adults will be aged 65 years and above. The study discussed here focuses on the experiences of older adults participating in regular group exercise and the effect of such activity on the person’s physical, mental and social changes. A community-wide intervention program named the ‘Fujisawa +10’ was created to spread the performance of physical activity among citizens based on the national physical activity recommendations made by the National Institute of Health and Nutrition of Japan. The Fujisawa+!0 exercise program was a community-wide intervention with exercise intensity at an extremely low level. Dynamic and static stretching exercises, knee-ups, squatting, knee exercises, arm circle exercises and body balance exercises done in standing or sitting positions are a regular part of the exercise routine programmed. These exercises were introduced to the elderly section of people who were voluntarily exercising together as a group at least once at the park (performed thrice a week) or community centre (performed once a week) in their community. All these adults were given a CD, DVD and manual instructions on how to exercise together as a group without an instructor. Participants selected were older adults who were participating in the ‘regular group exercise’ in community A and B. Only those community-dwelling older adults who were above the age of 60 participating in regular exercise in community A or B and those living independently without any elderly care assistance were included in the study. The research team conducted four focus group interviews including 26 participants (11 males and 15 females) whose mean age was 74.69 years. Community A had 15 older adults (7 males and 8 females) grouped into two focus groups with 7 (3 men and 4 women) and 8 (4 men and 4 women) respectively. Community B had 11 older adults (4 male and 7 females) who were grouped into two focus groups with 5 (2 men and 3 women) and 6 (2 men and 4 women) participants respectively. Each of the interviews lasted for 60-80 min, none of the participants suffered from disabilities or were diagnosed with dementia, no participant received any formal care, five were living alone and one used a stick due to joint pain. Investigators who had expertise in conducting focus group interviews (HK and KY) served as facilitators while two investigators (YO and YS) and two graduate students attended the focus group meetings as observers. Results The researchers could clearly confirm that ‘regular group exercise contributes to balanced health in older adults’ which consisted of seven themes (regular group exercise, functional health, active mind, enjoyment, social connectedness, mutual support and expanding communities) under its umbrella. It was observed that group exercise contributed to physical, mental and social well-being helping them improve on their functional health, peer interaction and their degree of enjoyment. People working out in groups cared for each other, felt connected and had a sense of security in the community. Older adults have aplenty free time after being done with their responsibilities towards their kids and hence, felt that regular exercise was critical in balancing overall health. Such regular exercises helped them lead an active life without succumbing to sedentary lifestyle habits that included getting up, sleeping or eating at haphazard timings. We also know that many elderly people live in isolation having lost their spouse or their kids stay away and they are forced to lead lives of their own. In such cases, gathering at one common place helped these people to interact with each other, prevent isolation and bring in a purpose to their living. When elderly individuals began their day with group exercises, they felt their body to be flexible, energized and fit while off days motivated them to exercise even stronger on other days. Exercises helped these participants to at least stay fit in their current level even if it did not help in improving their fitness quotient. Many participants felt that they were blessed to socialize and exercising individually at home could have never brought them this kind of an enjoyment. Group exercising also helped in expanding social connectedness and mutual support. The study clearly shows that group exercises benefit the overall development of the elderly individuals catering to their physical, social, emotional and mental needs. Combined Intervention Program While the advantages of group exercising seems to sound great there are also many downsides to it. It is not always possible for all the elderly individuals to commute as their health must permit and economic background should also support it; there is less attention paid to individual needs despite the fact that every ageing adults would be suffering from a different kind of body pain and finally, renting a place that’s close to many of the individuals participating and hiring an instructor for the same is not an easy job. Hence, merging a home-based intervention program with a group exercise program would be the best approach as it channelizes the individual’s exercising frequency, intensity and duration to the desired levels. A research team analysed the effects of a blended exercise program on adults in Europe. Participants were selected from a community-based program known as More Exercise for Seniors in which more than 3,00,000 older adults above the age of 55 years participated in a weekly group-based exercise class under the supervision of a trained instructor. The elderly individuals were asked to sign up for the focus group and instructors were contacted revealing the study’s intention. A total of 15 instructors were contacted and 8 focus groups were held (including two pilots) with 48 older adults. The focus-groups happened at locations where the weekly MBvO-class were held with each consisting of an average of 6 participants. All the participants in the group were asked about their opinion on an additional home-based exercise program. Results The two pilot groups and one focus group where data was lost weren’t included in the study and hence, the data from the other 30 participants were included in the analysis. Average age of the participants were 74 years, the individuals had almost been participating for around 9 years in the community-based program and all of them were female. Most participants took part in the weekly group exercise classes as they wanted to be physically fit and self-reliant without depending on others for their everyday chores and activities. Besides this, participants enjoyed being in the presence of others, felt motivated by each other, formed close friendship bonds and were delighted to have some quality fun. At the same time participants also revealed that home-based exercise programs brought about several benefits-it helped them fulfil their personal goals, could help them perform exercises that they were comfortable doing on that particular day owing to aggravated pain anywhere in the body and were also positive about the different levels of an exercise program that could be self-paced when performed individually. But many expressed motivation as a main concern while performing home-based exercises as group exercises are sure to be motivating and the presence of peers were a great support for regularity. Yet another Japanese study that analysed the benefits of exercising alone versus exercising with others found that though both had its own health benefits increased frequency of exercising with others had tremendous health benefits irrespective of the total frequency of exercise. References Regular Group Exercise Contributes to Balanced Health in Older Adults in Japan: A Qualitative Study: https://bmcgeriatr.biomedcentral.com/articles/10.1186/s12877-017-0584-3 Attitudes of Older Adults in a Group-based Exercise Program Toward a Blended Intervention: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5118593/ Exercising Alone Versus with Others & Associations with Subjective Health Status in Older Japanese: The JAGES Cohort Study: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5156899/ The Evolution of Group Fitness: Shaping the History of Fitness: https://journals.lww.com/acsm-healthfitness/Fulltext/2014/11000/The_Evolution_of_Group_Fitness__Shaping_the.4.aspx?WT.mc_id=HPxADx20100319xMP These days we hear a number of young girls and women complaining of irregular periods or prolonged absence of menstruation for even 3 months or so. Polycystic ovary syndrome (PCOS) is a common disorder among females characterized by hyperandrogenism, menstrual and ovulatory alterations and polycystic ovarian morphology. This is a condition that affects the woman’s ability to produce eggs causing a profound number of cysts to appear on the surface of the ovaries. The cysts are nothing but follicles that contain underdeveloped eggs which are often released at irregular intervals. In some, PCOS totally stops the release of eggs. Such conditions lead to irregular/loss of periods, weight gain, acne, thinning of hair, excessive hair growth in other parts of the body and fertility problems. But the effects of PCOS go beyond the reproductive boundary extending to insulin resistance, type 2 diabetes mellitus (T2DM) and cardiovascular disease. Insulin resistance has been proposed as one of the key effects of PCOS resulting in reproductive as well as metabolic disturbances besides increasing the risk of cardiometabolic risk for women with PCOS. PCOS has been declared as a nonmodifiable risk factor for diabetes by the International Diabetes Federation & by the American Diabetes Association with evidence from observational, retrospective and short-term prospective studies. We don’t have much long-term studies identifying increased risk of T2DM in women with PCOS.
Long-Term Prospective Study on Diabetes Risk in Women with PCOS PCOS is very common affecting 1 in every 5 women at some point of life. Though its cause remains unknown its believed that higher than normal androgen levels play an important part besides other risk factors such as excess weight and family history, both of which are also risk factors for insulin resistance. A long-term observational study on Italian women with PCOS was conducted for at least 10 years to evaluate the incidence rate of type 2 diabetes during the period. During the first examination between 1978 and 1999 every woman was screened for PCOS and in 2009, all of those having PCOS were asked to come for a follow-up examination during which the same set of tests as done during the first examination was performed. Even before the start of study those women with Cushing’s syndrome, androgen-secreting neoplasm, hyperprolactinemia, congenital adrenal hyperplasia, thyroid disease, or other causes of amenorrhea, including premature ovarian failure were excluded. All the women were questioned on their smoking, drug therapy and any history of diseases, their height, weight, waist circumference and blood pressure measurements were taken. Fasting blood samples were taken to measure levels of different hormones such as luteinizing and follicle-stimulating hormone, 17β-estradiol, testosterone, and sex hormone-binding globulin (SHBG). Blood samples were taken during the first week after start of menstruation and after withdrawal of bleeding and glucose tolerance test was performed too. Results After implementing various exclusion criteria, a total of 277 women were involved in the study from 1978 to 1999. All of them were once again contacted in 2009 for follow-up but 22 women were unavailable for data due to various reasons (death, some did not want to pursue further or had given birth to a child). The remaining 255 women were re-evaluated in 2009 and the information collected was used to compare between the rates of type 2 diabetes of women with PCOS and the general female population. 226 women with PCOS were regularly followed-up by the research team checking on their performance every 1-2 years. During the follow-up period 163 participants were on oral contraceptive treatment for at least a year, 72 were on metformin, 29 were on flutamide, 22 were on antihypertensive drugs and 4 were on statins. At baseline, there was no difference observed in any of the parameters with the exception of luteinizing hormone blood levels which was higher than normal in the participants. It was observed that 6 women were diabetic at baseline and 42 women developed type 2 diabetes during the follow-up. 39.3% of the population suffered from type 2 diabetes at the end of follow-up that’s higher than the general population. The follow-up period of diabetic women was much longer than that of nondiabetic women and, diabetic women were much older comparatively. They also had higher BMI and larger waist circumference, higher fasting glucose and insulin levels and higher glucose but lower sex hormone binding globulin (SHBG) levels. It was observed that a greater number of women with diabetes were under metformin treatment during follow-up compared to oral contraceptive treatment when compared to women free of disease. The incidence rate of type 2 diabetes increased with increasing BMI, fasting glucose and glucoseAUC rates at baseline. Whereas, a higher SHBG level at follow-up was linked to a lower risk of developing type 2 diabetes. When comparing the risk of T2DM with BMI levels it was seen that risk of diabetes steadily increased with BMI and was especially high when BMI≥30. Obesity is a common risk factor for PCOS, BMI values increase with increasing obesity rates and such high BMI levels and glucose rates contributed to increase in type 2 diabetes rates in women with PCOS. The study shows that risk of type 2 diabetes increased in women with PCOS during middle-age and hence it is required that women with PCOS are regularly screened for diabetes risk. Diabetes Risk for Women with PCOS based on CARDIA Study The coronary artery risk development in young adults (CARDIA) study was used for procuring study sample for diabetes risk in PCOS-affected women. The sample included 1127 women who were present both at Year 2 and Year 16 examinations with Year 2 examination considered to be the baseline for the study. Androgen values were obtained from Year 2 and Year 16; at year 16 the participants were queried about symptoms at two time frames, past (ages 20-30) and current (ages 34-46). All the women were questioned on the length and regularity of menstrual cycles. PCOS was reported by self-reporting symptoms such as oligomenorrhea, hirsutism and serum androgen measures. Participants having oligomenorrhea between 20-32 years of age and hirsutism between 20 and 30 years of age were classified as having PCOS. Women with PCOS were classified during two time frames: Year 2 (ages 20-32) and Year 16 (ages 34-46). Weight, height, BMI and waist circumference was measured. Participants were classified as ‘never PCOS’ when they did not fulfil the criteria for PCOS during both time frames, ‘early PCOS’ when they fulfilled Year 2 criteria only and ‘persistent PCOS’ when they fulfilled PCOS criteria at both time frames. Participants were branded as diabetic when fasting plasma glucose ≥126 or when they were using diabetes measurements. Of the 1127 women only 53 of them met PCOS criteria at ages 20-32. While PCOS-affected and normal participants did not differ in BMI, waist circumference, physical activity, alcohol use and tobacco use it was seen that women with PCOS had higher mean fasting insulin levels and had not given birth to babies. Both groups of women did not differ in terms of presence of hypertension and diabetes. Results showed that women with PCOS at ages 20-32 were likelier to develop diabetes by the time they reached 38-50 years of age and it doubled the risk of diabetes. PCOS increased the risk of diabetes by as much as 3-folds in normal weight women with PCOS compared to normal weight women without PCOS. Only 2% women met criteria for persistent PCOS while 3.5% were classified as having ‘early PCOS’. Those with persistent PCOS had a 7-fold risk of developing diabetes in the next 5 years compared to those without PCOS while those with early PCOS did not show such risks. Risk of Gestational Diabetes Due to PCOS Gestational diabetes mellitus (GDM) is a common concern in pregnant women whose rates can be anywhere from 9-25%. GDM and PCOS are one of the most common endocrine disorders in women of reproductive age both of which relate to overweight/obesity and insulin resistance and they are also clear indications of T2DM risk. A Finnish study tried to prove that PCOS is an independent risk factor for GDM. The Finnish Gestational Diabetes Study (FinnGeDi study) recruited a group of 1115 women with GDM and a singleton pregnancy who were about to deliver. Another set of 1125 women with no GDM giving birth in the same hospital were recruited as controls. After imposing exclusion criteria the research team was left with 1146 in the GDM group and 1066 women in the non-diabetic control group. All the participants were asked to fill a questionnaire about their medical and family history also involving questions on oligomenorrhoea, the presence of hirsutism and prior diagnosis of PCOS. A total of 1030 candidates with GDM and 935 non-diabetic women returned the questionnaire. GDM was diagnosed by a 2-h 75 g oral glucose tolerance test (OGTT) after overnight fasting. OGTT is generally performed between the 24th and 28th weeks of pregnancy but also can be done between 12th and 16th week when the woman is at a high risk of GDM. 521 women had irregular menses (oligomenorrhoea), 207 had hirsutism while 87 suffered from both. 124 of them reported prior diagnosis of PCOS and 37 reported prior diagnosis and two symptoms. This led to a total of 174 women with both symptoms and prior diagnosis to suffer from PCOS. The total study population of 1941 women were divided into four groups: GDM+PCOS (n=105), GDM+non PCOS (n=909), non-GDM+PCOS (n=69) and controls (n=858). Results
References Polycystic Ovary Syndrome is a Risk Factor for Type 2 Diabetes: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3425413/ Polycystic Ovary Syndrome & Risk for Long-term Diabetes & Dyslipidaemia: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3060760/ Polycystic Ovary Syndrome & Risk Factors for Gestational Diabetes: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6026881/ The Link between Polycystic Ovary Syndrome & Type 2 Diabetes: What Do We Know Today? https://www.openaccessjournals.com/articles/the-link-between-polycystic-ovary-syndrome-and-type-2-diabetes-what-do-we-know-today.pdf  Oh Mom! I Love this Gripe Water Oh Mom! I Love this Gripe Water Crying is the only language known to newborn. They cry when they are hungry, when something is troubling them, if they are suffering from even mosquito bite or when their diaper is overfull. But it is the responsibility of the parents to find out the accurate source for the tears, correct it and help the infant resume sleep or movement of his/her hands and legs. While its often any of the above-quoted reasons sometimes when you notice keenly you can observe that the infant cries continuously during a particular period of the day some days of the week. If that’s the case your kid might be suffering from infantile colic. Infantile colic is defined as episodes of inconsolable crying in an otherwise healthy infant younger than three months of age that lasts at least 3 hours a day and occurs at least 3 days a week over the course of at least three weeks in a month-this is a definition proposed first by Wessel. But a recent definition conveys that colicky infants cry constantly during the evening at the same time every day for at least a week but otherwise they are healthy. I guess many of you are interested to read further about this condition as most have faced or are facing this problem in bringing up our munchkins. Existing as a common condition around the world infantile colic affects one in five infants younger than three months affecting almost 28% infants in the first month of life. The symptoms worsen around 6 weeks after childbirth and improve gradually thereon. But we do have a Canadian study showing that 6.4% infants suffered from persistent colic symptoms at 3 months of age. Breastfeeding is advised until the infant’s sixth month and in such breastfed infants colic episodes are more common during late evening or early morning hours. Such disruptions during such odd hours ultimately results in maternal exhaustion and tiredness. Its been proposed that colic is not a sign of worry and there is nothing dangerous about it but it does indeed exist as a major burden to family members as it many-a-time leads to maternal depression (owing to unrealistic parental feeding expectations, irregular sleep patterns and constant worry over the baby) and might also cause shaken baby syndrome. There are even chances that the baby might stop breastfeeding earlier than expected and colicky behaviour that continues beyond the expected three months or so paves way for later sleep problems, allergic disorders, family dysfunction and behavioural problems. At a Loss for the Cause behind Colic Problems Almost every child faces this problem of infantile colic and the reasons remain elusive but we have various theories proposed. Colic might simply be a part of the regular crying protocol followed by kids. There is even a hypothesis that it is due to the impact of abnormal gastrointestinal motility and pain signals from pathways in the gut. It has also been proposed that the absence of adequate lactobacilli in the gut and increased presence of coli in intestinal microbiota affect gut motor functions and gas production thereby leading to such a condition. Lactose intolerance, gut contractions, mistaken interpretation by parents when the child cries normally, lack of adequate parent-child interaction, family tension and parental anxiety are some of the assumed causes of infantile colic. Increased maternal age has also been proposed as a cause for colic action in infant. On a Hunt Against Colic Brunt If you notice, the very word ‘colic’ has an abdominal origin. But studies have failed to show a positive link between gastro-oesophageal reflux and crying in infants younger than three months old. A randomized control trial (RCT) in both breast-fed and formula-fed infants revealed that at two weeks of age the incidence of crying more than three hours a day was 43% in formula-fed infants and 16% in breast-fed infants. A recent trial proposed that one week of low allergen diet among exclusively breastfed infants (6 weeks old) with colic reduces the risk of colic symptoms by 37% and this brings upon hope that diet alterations in maternal women might bring about some positive changes. A herbal drug containing chamomile, vervain, liquorice, fennel and balm-mint given to infants suffering from colic thrice a day showed marked improvement after seven days. But above all this a mother’s intervention might provide the best possible results against colicky infants. The study below is about one such intervention by moms. Cross-sectional Study The cross-sectional study involved infants younger than three months of age who had been diagnosed being colicky by their paediatrician. It included both breast-fed and formula-fed infants while those with diarrhoea, vomiting and abdominal distention were excluded. This left the study team with 400 infants of whom 181 were male and 173 were female. Moms were around 27 years of age and the infants birth weight were around 3100-3500 grams. 34% of the infant’s family had history of colic, 48.5% had normal vaginal delivery (NVD) and 92.5% mothers received breastfeeding training at the hospital. 196 infants (49%) were colicky and 204 infants (51%) were not. All the mothers imposed behavioural, nutritional or medical types of intervention to control infantile colic. Behavioural approaches used included responding to the crying baby by feeding, hugging, carrying around, wrapping the child in clothes (swaddling), using a pacifier, giving him/her toys, playing music, putting the baby to sleep or giving the baby to someone else as the mother could not cope up with stress. Nutritional approaches followed by the moms included avoiding grains, cereals, dairy, vegetables and meat. Sometimes the mother consumed herbal tea, administered herbal tea to infants or both the mother and the baby consumed herbal tea. Chemical drugs were also consumed sometimes by the mother and some other times by the baby. Behavioural intervention showed that the researchers could find significant difference between the two groups because of two main factors that included family income and mother’s education. In nutritional intervention, a significant difference was found between the two groups in their avoidance of a specific kind of food in accordance with the type of feeding. If the mother breastfed, she was actually pursuing more nutritional interventions. The herbal intervention group did not find any difference depending on family income, mom’s education level, family history of colic, infant sex, type of feeding, breastfeeding training and mother’s job. Non-colic group showed that both moms and babies consumed more herbal tea than those in the colic group. Herbal tea consumption by mothers in the colic group was greater than those in the other group. When it came to comparing chemical drug intervention there was significant difference found between the two groups as a result of family income, mother’s education, infant’s birth order, mother’s age and previous breastfeeding training. Chemical intervention was mainly in the form of gripe water in these infants. Now, there would be a smile in many readers faces as this is one of the oldest solutions used to soothe a crying infant. Effect of Maternal Diet Intervention on Colicky Infants A randomized, control trial was performed by a study group to test whether elimination of allergic food proteins from the maternal diet helps to reduce crying and fussing in infants. The study included exclusively breastfed infants <6 weeks of age suffering from colic problem. The moms were informed that the study included two different diets that were proved to be beneficial in colic-affected infants which ultimately led to the elimination of strict vegan diets. One was a low-allergen diet that excluded major food allergens and the other was a control diet that included the excluded foods by the first diet group as well. None of the diets included those containing food preservatives, colours and additives. All the moms were randomly assigned to one of the two groups. Low-allergen diet: Moms were asked to exclude all foods containing dairy products, soy, wheat, eggs, peanuts, tree nuts and fish from their diet. The diet primarily included meats, a rice milk drink, vegetables, fruits and cereals (corn and rice). Calcium supplements were prescribed and moms were also subscribed a plant-based drink in powder form alongside a daily consumption of fresh rice bread. Control diet: This diet excluded all those foods excluded from the low-allergen diet. All moms were asked to eat 1 serving of peanuts, 1 serving of wheat and 1 chocolate muesli per day besides maintaining their intake of meats, rice, vegetables and cereals. All the mothers received soy and cow’s milk powder mixture to make 500mL of milk which was consumed every day for 7 days. Cry and fuss charts were recorded by the mothers on the study days. Results A total of 107 infants entered the study of which 90 (84%) completed the trial successfully. 47 of 53 from the low-allergen group and 43 of 54 from the control group completed the study successfully. Only those who experienced more than 25% reduction in crying/fussing rates were included in the results that showed that 35 of the 47 infants responded to the low-allergen diet program compared to 16 of the 43 infants on the control diet. Changing the cut-off to 20% did not show any changes in the results. When all non-completers were taken as non-responders, they witnessed a 36% risk reduction in the low-allergen diet group. At the end of the study 61 of 90 infants still suffered from colic crying or fussing for a prolonged period of time. But, the cry/fuss duration per 48 hours was reduced by a greater proportion in the low-allergen group. We also have studies showing that replacing cow’s milk with soy and other milk varieties helps in reducing occurrence of colic problems in infants. It is essential that the condition is treated and minimized in any authentic way to help families, reduce risk of depression in mother, ease the child out of the situation and also avoid early breastfeeding cessation. References Effective Interventions of Mothers in Colicky and Non-colicky Infants: https://www.omicsonline.org/open-access/effective-interventions-of-mothers-in-colicky-and-noncolicky-infants-2167-0846-1000305-96060.html Effect of a Low-Allergen Maternal Diet on Colic Among Breastfed Infants: A Randomized, Controlled Trial: https://pediatrics.aappublications.org/content/pediatrics/116/5/e709.full.pdf?origin=publication_detail Dietary Manipulations for Infantile Colic: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2791658/ Infantile Colic: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6091773/  A Quick Chat Refreshes Your Mind A Quick Chat Refreshes Your Mind Mankind is entitled to two official breaks during working hours at office- a snack/tea and a lunch break. All the other breaks that we take, even going to the cooler to fetch water, having a small chit-chat with a colleague, attending phones during working hours or surfing social media sites are all unofficial breaks that we take out of our own will during office hours. We have a new term for these kind of breaks – ‘microbreaks’. Microbreaks are brief recovery periods taken between work-related activities. They are rest breaks taken to protect oneself against stress or accumulated trauma while working in a computer-related environment. In simple words, these are gaps taken between work schedules to enable the individual to replenish his/her lost energy stores occurred from prolonged work schedules. This gap might last anywhere from several seconds to minutes depending on the type of break availed. Two types of strategies are usually followed- one that focuses on recovery and another that focuses on maintaining work productivity. The former is productive than the latter as it replenishes resources while productivity-based strategies continue to deplete employee resources. There is no stipulated time duration and frequency but with only two rules that it should be short and voluntary. The concept of ‘microbreaks’ was invented in the late 1980s by researchers from the National Institute of Occupational Safety and Health in Ohio and Purdue University in Indiana. Each of the participants were allowed to take 27 seconds break every 40 minutes during which they remained seated at their workstations doing nothing. Though there was no significant difference seen in productivity people who had taken longer microbreaks reaped better benefits. Advantage of Microbreaks for Surgeons Microbreaks are used mainly to reduce the risk of developing injuries in the workplace. Surgeons are one of the main professionals who reap benefits of microbreaks as their job involves standing and focusing for long hours during surgeries which can cause fatigue, musculoskeletal disorders (MSDs) and work-related pain mainly in the neck, back and shoulders. Though ergonomic aids are suggested and have been used by surgeons but they don’t provide as much comfort and relaxation as expected. Also, we cannot expect surgeons to take breaks while doing a procedure as the patient’s safety becomes the first priority. Microbreaks were one remedy that promised to offer better results in minimizing ergonomic risk. A focus group consisting of 10 users (6 males and 4 females) were considered to take up a study test on microbreaks with a series of stretch exercises that were to be performed in between surgeries. All the stretches were designed by a physical therapist in collaboration with an ergonomist to address major issues that include posture correction, normalization of tissue tension and soft tissue mobility/gliding and relaxation/stress reduction. All the participants performed the stretches giving feedbacks on the likes and dislikes about the stretches also mentioning the components that prevailed as a hindrance for their performance. Before doing any of the stretches they were all shown a pilot video for 90 seconds. With repeated discussions and demonstrations, the best combination of stretching exercises that could be used during surgery without any need to scrub out was identified. The results were implemented into another video where two persons performed stretches with two views (side and frontal) for better visualization of the movement. They occupied the middle and left portion of the screen as these are the two places where we divert most of our attention. The video also had an audio that came up with step-by-step instruction for improved demonstration of the task, lower cognitive load and better accessibility in a sterile environment when the computer screen is not visible to the user sometimes. Keeping in view that surgeons become absorbed in the surgery a web app was developed in two stages which reminds them to take a break and talks them through the stretching procedure. The reminder included an alarm sound that did not startle the staff in the middle of a surgery, had a snooze option to delay the microbreak when the surgeon was in the middle of an important phase and was also made available to all the staff outside the operation room as well to help in snoozing or stopping the alarm. Once done, 7 surgeons (3 males, 4 females) consented to test the stretching app pilot in their ORs. Each of them performed at least 70% of the surgery and operative days were included if the procedure lasted for at least 2.5 hours with at least 4 hours of total surgical duration per day. At the end of day, each of them filled a short online survey to give their feedback on the effectiveness of microbreaks. 4 metrics including ‘physical performance’, ‘mental focus’, ‘body pain/discomfort’ and ‘level of fatigue’ were measured using ratings including Better, No Change or Worse. Six other questions were rated on a scale of 0 (none) to 10 (maximum). Non-Routine Event (NRE) data was measured through observation for the participant’s operative procedure. NREs are events that are treated to be distracting, undesirable, unusual or atypical. Results showed that the participants found it difficult to understand and follow verbal instructions in the video due to vague descriptions, problems in viewing the stretches and coordination problems (syncing left and right hand/leg movements with that in the video). Keeping all this in mind the final video time was cut to 68 seconds. The 7 surgeons had 6 microbreaks and were observed for 12 surgical days. The four primary outcome questions that provided three options as answers showed that after surgical procedure better physical performance and lower fatigue was reported 91.67% surgical days. Better mental focus was reported on 83.33% of surgical days and less pain/discomfort was reported on 100% of surgical days. Frequency of NREs in procedures without microbreaks did not differ from those with microbreaks. The pilot study clearly shows that it is necessary to take microbreaks in between to prevent negative impact on patient care due to job demands. A study on call centre people (one of the most emotionally tiresome jobs) helping them with microbreak interventions showed excellent benefit-those who were not engaged with their jobs started benefitting from microbreaks with improved productivity and more positive feelings. Another study conducted on 28 employees in a meatpacking plant over a 4-week period showed that active microbreaks reduced the discomfort faced by employees during the work day. Yet another study conducted on employees working on computer terminals focused on four main muscle areas and results showed that it reduced discomfort in all four areas during computer work especially when breaks were taken every 20 minutes. So, don’t forget to take short breaks in between to stretch yourself, go to the washroom or get some fresh air. If you don’t have the habit of taking breaks or belong to the type of personality who would become immersed in the job at hand it is better to have a timer to remind you! Don’t feel guilty when you look at the phones often, engage in a funny video or call someone who would make you laugh. But also remember to engage in productive work without overdoing on the break timings. Else you cannot deliver what has been promised withing the stipulated time. Providing Diverse Advantages Hence microbreaks are proved to reduce stress, discomfort, keep workers engaged and make work more enjoyable. References Mini Breaks, Many Benefits: Development & Pilot Testing of An Intraoperative Microbreak Stretch Web-application for Surgeons: https://journals.sagepub.com/doi/pdf/10.1177/1541931218621240 Active Microbreak Effects on Musculoskeletal Comfort Ratings in Meatpacking Plants: https://www.tandfonline.com/doi/abs/10.1080/00140139508925107 Computer Terminal Work & the Benefit of Microbreaks: https://www.sciencedirect.com/science/article/abs/pii/S0003687000000715?via%3Dihub A Series of Microbreaks Can Also Have a Powerful Effect on Your Body & Your Mind: https://www.bbc.com/worklife/article/20190312-the-tiny-breaks-that-ease-your-body-and-reboot-your-brain Children born during earlier days were underweight or overweight, tall or short and fair or dark. It was rare that a child was born with defects. But now, we perform multiple scans on the pregnant mom to check on the health of the fetus due to fear of multiple health problems that crop up these days. Children born preterm are at an increased risk of autism spectrum disorder (ASD) with earlier deliveries garnering increased risks. Almost 5% of kids with a birth weight <2000 grams and 8% of those born <26 weeks of gestation are at a higher risk of ASD. ASDs are neurodevelopmental pathologies impairing social competencies and patterns of behaviour. Diagnosis is made purely based on observing the behaviour of the child and can be confirmed with any two of the following symptoms occurring repeatedly-repetitive patterns of behaviour, interest and activities, and lingering difficulties in social communication and interaction. Though we do come up with various proposals behind the occurrence of this condition none of them can justify the cause of the disorder on their own. It is widely accepted that both genetic and environmental factors contribute to the development of ASD but studies show that only 30% cases are clearly linked to these causes leaving the rest to assumption.
Worldwide, 0.76%-1.46% individuals suffer from ASD and over the past couple of decades the rates are steadily increasing for reasons unknown-some quote improved awareness in diagnostic criteria while some others propose changes in environmental factors to be potential contributors for this increase in rates. Despite advances in medicine and science we don’t have a proper curative treatment for ASD, a disorder that’s currently increasing at rapid rates. This has invoked many families (almost 28%) to rely on complementary and alternative medicine (CAM) to treat patients with ASD despite the long-standing fact that there is no scientific proof for this except in the case of melatonin. There have been many proposed diets, ingredients and foods that benefit kids with ASD but all of them without much proofs. Omega-3 fatty acids are one among these used by more than 28% kids with the disorder despite sufficient evidence to back up its benefits. Omega-3 fatty acids are polyunsaturated fatty acids (PUFA) found in three main types in the human diet-ALA (alpha-linolenic acid), DHA (docosahexaenoic acid), and EPA (eicosapentaenoic acid). DHA and EPA are found in seafood, while ALA is found in nut and plant oils. DHA and EPA can be synthesized from ALA by the human body but none of them can be synthesized from scratch. PUFAs have always occupied limelight when it comes to psychiatric diseases and evidences do show that PUFA deficiency is linked to neurodevelopmental problems such as schizophrenia, ASD and bipolar disorder. PUFA has an anti-inflammatory effect which has been proposed to be helpful in brain function but because they cannot be synthesized by the human body it can cause an imbalance in PUFA levels which might be one of the reasons why we see increasing number of ASD cases nowadays. Omega-6 and omega-3 fatty acids are the two main PUFAs whose consumption must be 1:1 to 4:1. But the lifestyle and dietary habits presently lead to increased intake of omega-6 fatty acids once again increasing the risk of psychiatric diseases. All these make one thing clear-omega-3 and omega-6 fatty acids might hold a bigger role in affecting psychiatric conditions in individuals when taken in the right quantities. Systematic Review of Clinical Studies Reporting Effective Treatment of Omega-3 Fatty Acids There have been studies reporting poor concentration of omega-3 fatty acids in kids with ASD compared to controls and also in those with schizophrenia and ADHD. Yet another recent study supported the positive effects of fatty acids on treating people with depression. A group of researchers conducted a systematic review to research on all prior clinical studies that reported effective treatment of this fatty acid on kids with ASD. Databases such as MEDLINE and EMBASE were searched using key terminologies and various exclusion criteria to pick the appropriate studies that would suit the needs of the researchers. The team used letters to provide consent whether or not the fatty acids could be used to treat patients with ASD. A or B was used to denote that treatment should be provided to patients, C grade indicates that treatment should not be offered routinely and D grade shows that treatment should never be given. Though the database came up with 143 articles only 6 of them satisfied the inclusion criteria. Of this, only 1 was a randomized control trial which included 13 children with autism who were either assigned to 1.5 grams of omega-3 fatty acids or a placebo for 6 weeks. The aberrant-behavior checklist which included items such as hyperactivity and sensitivity showed improvements in the group consuming fatty acids but none of them were statistically significant. 4 studies were uncontrolled and open-label ones that had kids or adults with autism as participants. A study was done by Politi et al. done on 19 adults with a mean age of 29 suffering from severe autism, moderate to greater mental retardation and maladaptive behaviors. They were given 0.93 grams of fatty acid (DHA+EPA) and a vitamin supplement (5 mg of vitamin E daily). There was no improvement seen in any of the problematic behaviours while there was improvement in both severity and frequency of symptoms in the post-treatment period. Meguid et al. treated 30 children with autism for over 3 months using both omega-3 and omega-6 fatty acids and vitamin E. While 20 of the 30 kids showed improvement in the Childhood Autism Rating Scale there was no mean change observed in the group of 30 children. Another study by Patrick et al. on 22 kids given a daily capsule of omega-3 acids for 3 months showed that there was a significant increase in subscale assessments of basic language and learning skills from day 0 to 90. Bell et al. who studied 9 kids with Autism or Asperger’s were given one of two different omega-3 fatty acids of varying doses for 6 months. Though specific values did not show tremendous improvement there was an overall improvement in general health and other measures. Another study on an 11-year-old boy with autism right from age 2.5 suffering from anxiety and agitation showed that supplementing fish oils at 3g/day proved that there was complete elimination of anxiety and agitation after 1 week and the improvements were stable after 8 months of follow-up. The different study results show that there is insufficient evidence backing the benefits of omega-3 fatty acids on treating autism. Omega-3 & Omega-6 Fatty Acids & Effects on Kids with Autism A study conducted for knowing the effects of both omega-3 and omega-6 fatty acids on kids with autism included 565 children with attention deficit hyperactivity disorder (ADHD, n=401), ASD (85) or controls (n=79) aged between 3 and 17 years. Those with ASD were younger than those with ADHD or the controls. All kids and parents underwent a series of tests and questionnaires that included: The tests of variables of attention (TOVA) version 7 that analysed attention and impulsivity, The Australian Twin Brother Rating Scale (ATBRS) which rated 20 items on a scale of 0-3 where 0 means not at all and 3 means very much/very often and, Childhood Autism Rating Scale (CARS) that comprises of 15 scales measuring various things such as anxiety reaction, verbal communication, activity level, etc. and fatty acid analysis. Results showed that kids with ADHD and ASD had lower erythrocyte DHA, lower EPA, lower AA, higher AA/EPA and lower n-3/n-6 ratio than controls. Kids with ASD had lower DHA, EPA and AA and higher n-3/n-6 ratio than kids with ADHD. Kids with ADHD and ASD had lower levels of n-3 PUFAs EPA and DHA. Such lower levels of DHA, EPA and n-3/n-6 ratio and higher AA/EPA ratio was linked to greater severity of symptoms. DHA levels in the study reported 2.28% for kids with ADHD, .85% for ASD and 4.72% for controls. It was evident that lower DHA levels showed poorer reading and greater ADHD-type behaviour. Another study by Brigandi et al. showed that DHA levels were 1.4% in the erythrocyte membranes in kids with autism compared to 1.76% in controls. This shows that a value of 0.85% in the ASD group is very low. There is an improvement in reading and ADHD-type symptoms observed in kids who do not have ADHD when treated with EPA plus DHA or DHA. There are various studies showing marked improvements in kids with ADHD when they were given a supplement containing a 3/1 ratio of EPA/DHA showing that EPA has stronger effects than DHA. A study by Milte et al. on kids supplemented with high DHA, EPA or omega-6 showed that increased EPA or DHA was linked to improved cognition and behaviour and this association was strongest for DHA. The DOLAB study that supplemented school children with poor reading performance with DHA showed improvement in parent-rated ADHD-type symptoms and reading performance too. Omega Supplementation in Toddlers Preterm infants are at a higher risk of ASD and finding the effectiveness of omega-3 and 6 fatty acids could help kids. A pilot trial and a full-scale trial supplementation was done on toddlers born preterm and showing ASD symptoms. Preemie Tots Trial: This is a randomized, placebo-controlled trial which included children aged between 18 and 38 months born ≤29 weeks of gestation. Those children who tool FA supplements, fatty fish or growth-promoting beverages with DHA ≥2 times/week were excluded apart from enforcing several other exclusion criteria. Parents of potentially eligible kids were asked to complete a questionnaire containing screening tools to assess early ASD symptoms which contained the Pervasive Developmental Disorder Screening Test II, Stage II (PDDST-II), the Brief Infant Toddler Social and Emotional Assessment (BITSEA) and another one from Ages and Stages Questionnaire-social emotional for assessing joint attention. All the kids were assigned to one of the two color coded groups (2 treatment and 2 placebo). The treatment group underwent 90 days of daily oral FA supplementation with lemon-oil-flavoured fish and borage oil and the placebo group was assigned to a daily intake of canola oil. All the 31 participants selected after imposing various exclusion criteria were born at a mean of 27 weeks of gestation, were at a mean of 27 months old at enrolment and were males comparatively. Their mean PDDST-II score was 6 and the cut-off for evaluation for ASD ≥5. Almost 74% of the participants scored in this range. At the end of the 3-month study parents reported improvement on the behaviour-rating scale in both treatment and placebo group. The treatment group showed greater improvement on the BITSEA ASD scale than the placebo group. The study team continued to observe the participants and by Jan 2017 all the kids were around 70 months old and 12 of them received a diagnosis for ASD (2 in the treatment group and 3 in the placebo group had diagnosis, 4 in the treatment group and 3 in the placebo group had symptoms noted). There was an increase in the concentration of EPA, DHA and total n-3 fatty acids. The treatment group experienced larger increase in erythrocyte EPA and DHA with decrease in LA, AA and docosapentaenoic acid (DPA) and the placebo group experienced no notable changes in FA concentrations. References Omega-3 Fatty Acids for Autism Spectrum Disorder: A Systematic Review: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2710498/ Omega-3 & Omega-6 Polyunsaturated Fatty Acid Levels & Correlation with Symptoms in Children with Attention Deficit Hyperactivity Disorder, Autism Spectrum Disorder & Typically Developing Controls: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0156432 Omega-3 and Omega-6 Fatty Acid Supplementation May Reduce Autism Symptoms Based on Parent Report in Preterm Toddlers: https://academic.oup.com/jn/article/148/2/227/4913038 Supplementation of Omega-3 Fatty Acids May Improve Hyperactivity, Lethargy & Stereotype in Children with Autism Spectrum Disorder : A Meta-analysis of Randomized Control Trials: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5634395/  Not only A Treat to the Eye but One to Our Body as Well Not only A Treat to the Eye but One to Our Body as Well Breakfast, the most important meal of the day, is still undervalued and given lesser prominence than deserved. Man lives by his own set of preferences and priorities in which eating a healthy morning breakfast exists down in the list for most people. We become our own nutritionists and dietitians dictating food intake practises and diet routines to achieve several goals including weight loss, fat loss and more. In this process, breakfast becomes the most affected meal of the day as we skip it based on multiple factors such as absence of time to prepare food and eat, weight loss strategies or calorie restrictions. We skip breakfast 1, 2, or even 3 times a week and for some others eating breakfast is a luxury indulgence when they have time. Such repeated instances of breakfast skipping have been associated with a number of health problems including cardiometabolic risks, obesity, insulin insensitivity and type 2 diabetes. Besides affecting the health of the individual skipping breakfast makes a person sluggish, lose concentration, lack focus and optimal memory skills and perform not up to the expected standard. Type 2 diabetes mellitus (T2DM) prevails as one of the leading causes of morbidity and mortality rates worldwide owing to our unhealthy lifestyle and dietary practises. Unbalanced blood sugar levels bring about microvascular (retinopathy, nephropathy and neuropathy) and macrovascular (coronary artery disease and cerebrovascular disease) complications that contributes to increased medical expenses and health degradation too. Aichi Workers’ Cohort Study Japan has a 10.2% diabetes rate in male workers aged between 40 and 69 years and a 4.7% rate in female workers in large-scale companies in 2008-2010 and 15.0% in men and 8.0% in women in the National Health and Nutrition Study in 2011. Almost 14.4% men and 11.1% women skip breakfast which is a modifiable risk factor for T2DM and finding out the reason behind this can help us correct the risk and lead a healthier life. This motivated a group of researchers to extract data from the Aichi workers’ cohort study that included 6648 Japanese civil servants in Aichi prefecture aged 35-66 years in 2002. All of them answered a questionnaire regarding their lifestyle and medical history and were followed up until 2011. T2DM prevalence in the participants were examined through two methods: One, by noting down the year when fasting blood glucose (FBG) levels reached ≥126 mg/dL and the date of onset was set as July 1st. Second, the answers from the questionnaires helped the researchers know the existence of diabetes in patients and the year of onset. All the participants were probed for their breakfast habits using yet another self-administered questionnaire and eating frequency was assessed using five categories-every day, almost every day with occasional skips, 3-5 days/week, 1-2 days/week and none. Using the frequency response all the participants were split into two groups-breakfast eaters (included those who reported eating breakfast every day and almost every day with occasional skips) and breakfast skippers (all the other categories). The brief-type dietary history questionnaire (BDHQ) included data on intake of fish, fruits, vegetables, whole-grains, cereals, coffee, sugar-sweetened beverages and snacks and also speed of eating classified as very fast, relatively fast, medium, relatively slow and slow. Height, weight, BMI, blood glucose levels and insulin concentration were noted down. The participants were analysed for their smoking habits classified as current, former and never; the number of days they were engaged in physical activity classified into two categories ≥3 days/week or <3 days/week. Work timings were noted and scheduled into 4 categories-shift work including night shifts, shiftwork but without night shifts, without shiftwork but with night work and without shiftwork or night work. Sleep duration was classified as <7h or ≥7h and stress was classified into 4 categories including very much, much, ordinary and little. Results Of the 4631 who participated 90.4% ate breakfast. On a comparative basis, those who skipped breakfast were following a worse lifestyle that included current smoking, alcohol consumption, increased intake of sugar-sweetened beverages and decreased intake of fruits and vegetables. Results showed that:
Chronotype as a Middle Man between Skipping Breakfast & Type 2 Diabetes Incidence Cross-sectional and longitudinal studies show increased cardiometabolic risk in kids and adults who skip breakfast. A long-term study spanning more than 20 years showed that those who skipped breakfast at childhood and adulthood showed greater waist circumference and higher fasting insulin, total cholesterol and LDL cholesterol than those who eat breakfast. A big-scale long-term study spanning more than 16 years on 29,206 participants showed that skipping breakfast was associated with a 21% increased risk of type 2 diabetes. But, a study on low-income Latino diabetic patients showed that breakfast skipping was linked to increased plasma glucose levels but not haemoglobin (HbA1C) levels that’s generally taken as the standard for diabetes measurement. The circadian cycle ensures regulation of a number of daily physiological rhythms including sleep/wake and feeding behaviour, peripheral tissue metabolism, energy expenditure and hormonal profiles. Each of us are at our peak energy levels at different times during the day-some during the early morning hours called as ‘morning lark’ and some during late nights called as ‘night owls’. The chronotype of the individual can be deduced from self-reported sleep times. We all love to stay late nights and get up even later but a study shows that those who do so are at a 2.5 times higher risk of type 2 diabetes which in turn indicates that a later chronotype keeps the individual at a higher risk of T2DM. Likewise, those with a later chronotype often eat less or skip eating altogether after waking up late in the morning. These individuals prefer to eat more of alcohol, fat and cholesterol, especially during dinner compared to those with an early chronotype. Maybe that’s why late risers probably suffer from poor glycemic control. A study focused on knowing more about the role of chronotype in patients with T2DM and skipping breakfast. The study team invited patients from the Rush University Medical Centre and once chosen all of them self-reported age and race, recorded height, weight, BMI and entered the recent Hb1Ac values. Bedtime, wakeup time, sleep onset latency and sleep duration both during weekdays and weekends during the previous month was recorded. Mid-sleep time as the midpoint between sleep onset and wake time was calculated and mid-sleep time on free days (MSF) was arrived at from mid-sleep time on weekend nights with adjustments for sleep duration on weekend nights was calculated. SDF is calculated sleep duration on weekend nights and SDw is calculated sleep duration on weekday nights. All the participants mentioned their perceived actual sleep duration and preferred sleep duration on weekdays. They answered a 24-h dietary recall to know about the content and timing of the meal over the previous day. Total calorie intake over the day was also calculated using this data. Results Comparison between breakfast eaters (n=172) and breakfast skippers (n=22) showed that those who skipped breakfast were significantly younger and had higher HbA1c levels and BMI but had no difference between groups in median diabetes duration, insulin use or number of diabetes complications. Those who skipped breakfast generally had a later chronotype as their bedtime routine was later than those who ate breakfast. More number of breakfast skippers complained of lack of appetite during morning hours and reported consuming fewer total calories during the previous day. These guys consumed a major portion of their calories during lunch and dinner compared to those who ate breakfast. It was seen that breakfast skipping was associated with significantly high HbA1c levels. To see the effect of chronotype on diabetes and breakfast skipping a series of regression models were performed. In the first model, skipping breakfast was linked to higher HbA1c levels and in the second model it was linked to later MSF. In the third model MSF was linked to HbA1c and the fourth model suggested that MSF and breakfast skipping was linked to higher HbA1c. Chronotype did not entirely have an impact on breakfast skipping and HbA1c levels but it was seen that both chronotype and breakfast skipping remained independently linked to poor glycemic control. Behavioral interventions in the form of eating breakfast or modifying sleep time could be considered strategies for improving glycemic control in the participants. Other Studies The meta-analysis results from 2015 showed a direct link between breakfast skipping and type 2 diabetes risk but we don’t have any dose-dependent studies until now that can confirm whether skipping once a week would be less destructive than skipping twice per week. It is also not right to categorize all those who skip breakfast into one single category without paying heed to the frequency of times as this does have an important impact on the results. A meta-analysis of studies on skipping breakfast and type 2 diabetes using two random-effects models was done-standard random-effects model meta-analyses and dose-dependent meta-analysis. Though six studies met the inclusion criteria only 4 had BMI data. The standard random effects meta-analysis showed a 32% increased type 2 diabetes risk before adjusting BMI and a 22% increased risk after adjusting for BMI. Pooled RR value was 1.06 suggesting an increased risk of 5% after adjusting for BMI. There was an increased risk of 55% seen for 4-5 days of skipping breakfast/week before adjusting BMI and an increased risk of 40% after adjusting for BMI. It was observed that prolonged periods of fasting including skipping breakfast led to an increased postprandial insulin resistance during the next meal and increased ghrelin (hunger hormone linked with weight gain) levels as well. But we also have data showing that intermittent fasting, alternate day fasting and daily calorie restriction helped reduce diabetes risk factors such as body weight, viscera fat, fasting insulin and insulin resistance and we need long-term trials to confirm anything. Glucose concentration and markers of insulin resistance (such as high cholesterol and inflammation) are higher after lunch on days when individuals skipped breakfast. This inflammation affects insulin sensitivity thereby increasing one’s risk for obesity and type 2 diabetes. It is always recommended to start the day on a healthy note with fruits, whole grains, milk, eggs and nuts while avoiding high-sugar and processed foods. References Breakfast Skipping is Positively Associated with Incidence of Type 2 Diabetes Mellitus: Evidence from Aichi Workers’ Cohort Study: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4411234/ The Relationship between Breakfast Skipping, Chronotype & Glycemic Control in Type 2 Diabetes: https://www.tandfonline.com/doi/abs/10.3109/07420528.2013.821614?journalCode=icbi20 Breakfast Skipping & Type 2 Diabetes: Where Do We Stand? https://academic.oup.com/jn/article/149/1/1/5280617  Eat all Fruits & Veggies Besides Green Leafy Vegetables for Maximized Lutein Absorption Eat all Fruits & Veggies Besides Green Leafy Vegetables for Maximized Lutein Absorption Some nutrients are synthesized by the human body while some aren’t and must be acquired by consuming those foods that are rich sources of these nutrients. These are called as essential nutrients which includes vitamins, minerals, proteins, fats, water and carbohydrates. Nutrition is integral for human health which includes proper functioning of all body parts and organs including the human eye as well. Our eyes provide us with vision and this is extremely important for our day-to-day functioning and a good quality of life. Despite this, we don’t take proper care to maintain a good eyesight by consuming those foods that cater for good vision. The most important causes of visual impairment include cataracts, glaucoma, age-related macular degeneration (AMD) and diabetic retinopathy. Statistics show that cataract and AMD cases are only going to increase in numbers in the coming years which requires intervention as soon as possible. Intervention strategies are usually in the form of nutrient intake and when we talk about eye health one cannot but mention the involvement of lutein and zeaxanthin. Lutein and zeaxanthin are carotenoids that are together referred to as xanthophylls or macular pigment accumulating in the macular region of the retina and protecting the retinal cells needed for vision. Besides being integral for eye health lutein is also absolutely necessary for memory and brain function. It is known that improving brain health in adults is not easy and our target should be to improve nervous system functioning in infants when they are still in the development stage. Carotenoids are plant bioactive compounds that cannot be synthesized by mammals but must be consumed in the form of fruits and vegetables. But this doesn’t make lutein and zeaxanthin essential nutrients and research is still going on whether they should be included in the list too! Lutein is amazingly present in the cord blood at the time of delivery of the newborn transferred to the fetus via the placenta which makes the lutein concentration in the newborn dependent on the maternal concentration levels. Soon after birth the newborn receives lutein from mother’s milk. Studies on carotenoids concentration in breastmilk show that they are dependent on maternal dietary intake. This means that every newborn has different lutein levels as every mother follows a different dietary routine. Analysing breastmilk carotenoids might be the best way to find the link between maternal, breastmilk and infant carotenoids status. Carotenoids Levels in Infants: A Poland Study This was a study that consisted of three study sessions at the 1st, 3rd and 6th month of lactation during which breastmilk samples were collected, anthropometric measures assessed in infants as well as mothers, mom’s psychological state evaluated and the infant’s psychomotor development measured during the 6th month. All the participating moms were requested to fill a questionnaire that enquired about their lifestyle, health and nutrition during the preconception, prenatal and postnatal periods. The study was thrown open to anyone between 18 and 45 years of age who had given birth to a single, healthy infant. After applying exclusion criteria, the study included 53 mother-infant pairs. Most mothers had normal BMI during the first month of lactation, 78% of them had a normal weight at the third month and 85% during the sixth month. 47% were bearing their first child and 53% of the infants born were females. All the participants were requested to collect breastmilk at home: pre-feeding and post-feeding breastmilk was collected 24 hours prior to each study visit during 4 different time periods to compensate for any difference in carotenoid concentration. Macronutrient composition including energy and fat content was analysed three times and the average was used for comparisons. Carotenoid concentration was assessed using milk samples with the help of high-performance liquid chromatography. A 3-day dietary recall was taken at the 3rd and 6th month of lactation which helped the researchers predict macronutrient and micronutrient intake. These were used to calculated dietary fibre and fatty acid profiles. Lutein and other nutrient intakes were calculated and dietary data and supplement information was noted. Height, weight and BMI measurements were taken for all participating mothers. Results
Lutein Content: Mother’s Milk Versus Infant Formula Some infants don’t accept breastmilk and the parent is forced to feed them infant formula which drastically differs in lutein concentration compared to mother’s milk. Human milk contains higher concentrations of the carotenoid comparatively. A study in Poland enrolled exclusively formula-fed and breast-fed infants born between 37 and 42 weeks of gestation for a 12-week study period. Inclusion criteria included that mothers of these infants consumed at least 6 cups of dark green leafy vegetables (good sources of lutein) per week. Lutein fortification in infant formula was to be 20, 45, 120 or 225 mcg lutein per liter of formula. Formula-fed infants were fed with any one of the four study formulas. Human milk was expressed using a breast pump and a mid-afternoon sample represented the 24-h concentration of lutein. 40 infants were enrolled in the study of which 14 were fed with human milk and 26 were fed with formula milk. 6 of them could not complete the study leaving the researchers with 34 of them. Results showed that mean lutein concentration in human milk samples were similar at weeks 4,8 and 12. Lipid content was 41.5 g/l, lutein content was 21.1 mcg/l and average amount of lutein per gram of milk fat was 0.492 mcg. Infants fed with mother’s milk had higher lutein concentration than any of the infants fed with any of the four study formulas. But lutein concentration did increase from baseline in all formula-fed infants except in the unfortified group. After the 12-week study period human milk-fed infants had a 6-fold higher mean serum lutein concentration than the unfortified formula-fed infants. Lutein levels did increase in formula-fed infants as well depending on the dose of lutein fortification given at the end of the 12-week period. Serum lutein concentration increased by 3.7 mcg/l for every 1 mcg/l increase in human milk lutein concentration in breastfed infants but it was only 0.9 mcg/l for every 1 mcg/l increase in formula lutein concentration in infants fed with formula milk. Clearly human milk-fed infants had greater lutein concentrations compared to formula milk-fed infants. Breastmilk Facilitates Lutein Absorption Carotenoids protect our eyes (through absorption of blue light) by safeguarding the retina where they are highly concentrated. Lutein and zeaxanthin are transported in plasma in LDL and HDLs. In vitro studies show that lutein was delivered to cells by LDL via the LDL receptor while zeaxanthin was delivered by HDL via a scavenger receptor. The brain and the retina contain a lutein-binding protein called the steroidogenic acute regulatory domain protein (StARD3) whose concentration depends on the lutein concentration available in both these body organs thereby playing an integral role in lutein intake. We have studies showing that there is an increased absorption of lutein from breastmilk compared to formula but another study has taken it a step forward proving that there is not only increased absorption in the plasma but also increased deposition of lutein in the retina and brain. The researchers theorized that increased lutein absorption from milk might be due to two factors that differ in formula: the milk-fat globule structure and milk lipases. Lutein is a fat-soluble carotenoid that actually requires fat for optimal absorption. So, lipid structure in the feed affects lutein absorption. Whereas the infant formula used in this study has a simple fat structure that’s based on high-oleic safflower oil, soybean oil and coconut oil. Formula lipids are designed in a certain way to increase shelf life and such a difference in lipid architecture could be one of the reasons for increased lutein absorption in breast milk compared to formula milk. Besides this difference, formula milk also lacks key bioactive ingredients from the mother that’s present in human milk-lipases. Lipases help in lipid digestion within the infant gut and this absence in formula milk once again leads to decreased lutein absorption. Lipases and structure differences in the milk-fat globule lead to enhanced carotenoids absorption from breast milk and this shows that infant formula cannot rely on supplements as a means to increase lutein concentration. It is ideal that researchers use blueprint of milk as a model to design novel lipid formulations with the right kind of architecture for increased absorption and improve enzyme presence for enhanced carotenoid delivery. First, this once again reinstates the fact that every mom should breastfeed unless it’s an unavoidable circumstance. Second, moms should ensure to increase their consumption of fruits and vegetables for increased dietary intake of lutein and zeaxanthin. Maximize intake of eggs, corn, kiwi, squash, pumpkin, spinach, orange and green bell pepper, cucumber, seedless grapes and peas for significant lutein absorption by the body. References Serum Lutein Concentrations in Healthy Term Infants Fed Human Milk or Infant Formula with Lutein: https://link.springer.com/article/10.1007/s00394-009-0047-5 Carotenoid Content in Breastmilk in the 3rd and 6th Month of Lactation & its Associations with Maternal Dietary Intake & Anthropometric Characteristics: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6356523/ How Does Breast Milk Enhance Lutein Absorption? https://academic.oup.com/jn/article/148/1/1/4823729 Fruits & Vegetables that Are Sources for Lutein & Zeaxanthin: The Macular Pigment in Human Eyes: https://bjo.bmj.com/content/82/8/907  Supplements are a Regular Routine in Every Woman’s Life Supplements are a Regular Routine in Every Woman’s Life Children are replicas of their moms and dads mostly with some of them not bearing any attributes of their parents which is rare. Personality and characteristic trait are genetically transferred which makes us gloat with glory when the child behaves like his/her parent. Reproduction is an indispensable part of every person’s life that adds meaning to our existence and helps in taking our family’s virtues and ideologies to future generations as well. But sadly, most women in reproductive age worldwide suffer from obesity/overweight and so younger adults, adolescents and kids. Such high prevalence of obesity during early years has been attributed to several risk factors that affect early during pregnancy in the form of higher maternal pre-pregnancy body mass index (BMI) and excessive gestational weight gain. These risk factors are modifiable ones but when left untreated they do have a serious effect on the infant size at birth and obesity risk later during life. We also have numerous studies showing that maternal obesity/overweight during pregnancy pose as significant risk factors for higher birth weight and neonatal adiposity and also for childhood obesity later. The pregnant mother is the sole means through which the developing fetus acquires all nutrients needed for normal growth and development but maternal pre-pregnancy status and environment also play an equally critical role as pre-pregnancy obesity has the ability to result in foetal macrosomia (where the birthweight ≥4 kg). Once pregnant, the in-utero environment has an upper hand on foetal development including cognitive, organ development and deposition of fat. The environment in which the fetus develops determines the foetus’s genetic transcription affecting it differently depending on the stage of pregnancy. Its isn’t uncommon for the pregnant woman to develop gestational diabetes during any time of pregnancy and the mother’s carbs intake and increase in insulin insensitivity results in higher levels of maternal blood glucose which can be transferred to the fetus besides the foetus’s own insulin production that increases foetal growth and adiposity. Hence, maintenance of maternal insulin levels is absolutely necessary to avoid any deviation in foetal glucose levels. When such is the effect of maternal nutrient intake it is also equally difficult to impose restrictions and help the woman lose weight before pregnancy as most of the pregnancies go unplanned. But once pregnant it is indeed possible to regulate dietary intake levels of the mother-to-be as maternal dietary energy and protein intake affect neonatal anthropometry making food consumption an integral part of the pregnancy process. Gynaecologists prescribe supplements even before the woman becomes pregnant (such as folates) and these continue until delivery of the child. Though maternal micro- and macronutrient intake affects neonatal body composition we don’t have much data available in this field of science as there are quite a lot other factors including physical activity, socioeconomic status, stress, smoking and drug intake that affect foetal growth and development. The study elaborated below uses cohort from the ROLO (Randomised Control trial of Low Glycemic index diet versus no dietary intervention to prevent recurrence of foetal macrosomia) to study the effect of maternal body composition, demographic characteristics, macronutrient intake and lifestyle changes on neonatal weight and adiposity. Cohort from ROLO Study The present study used 542 mother and infant pairs from the ROLO study in which the mothers had given birth to infants with macrosomia previously and hence, were put on a low-glucose diet to decrease the recurrence of macrosomia. Results of the ROLO study showed that the intervention group experienced significant reduction in glycaemic index and load and also had lower gestational weight gain and glucose intolerance but birthweight or risk of macrosomia was not significantly reduced. All the 542 mothers underwent well-being tests, maternal weight, height, BMI and upper-arm circumference were measured during the first antenatal consultation with maternal weight measurements and gestational weight calculations performed during every subsequent consultation. Once the mothers gave birth, neonatal weight, height, mid-upper arm, abdominal, hip and thigh circumference, biceps, triceps, subscapular and thigh skinfold measurements were taken. This resulted in only 266 neonates having complete data of all the measurements taken. The pregnant woman’s macronutrient intake, glycemic intake and glycemic load was measured using a 3-day food diary given during each trimester of pregnancy. Cluster analysis of the food intake resulted in two main clusters of healthy and unhealthy individuals with regard to diet. While the unhealthy cluster ate more of refined foods, white bread, confectionary, chips, processed meats and high-energy beverages the healthy cluster chose to eat more of fruits, vegetables, cereals, fruit juice, low-fat milk and white meat. Dietary intake was analysed using a self-administered 170 item SLAN (Survey of Lifestyle, Attitudes and Nutrition in Ireland) food frequency questionnaire (FFQ) that was given during the initial stages of pregnancy and returned by 28 weeks of gestation. The data in the FFQ was in turn used to create a Dietary Approaches to Stop Hypertension (DASH) index with a score of 0 indicating total non-concordance and 11 indicating total concordance. A glucose challenge test (GCT) was done at 28 weeks of gestation. Result Maternal characteristics did not change between the control and intervention group except for gestational weight gain, glucose intolerance and maternal well-being score. There was no difference in neonatal weight, length or anthropometric measurements between the intervention and control group except in the case of thigh circumference measurement and in the case of neonatal waist: length ratio that was lower in the intervention group. The control group experienced more gestational weight gain than the intervention group. It was also seen that birthweight was associated with gestational weight gain, birth length was negatively associated with maternal smoking, neonatal abdominal circumference was positively linked with maternal saturated fatty acid (SFA) intake which showed a negative trend as the association switched over to polyunsaturated fatty acids (PUFA) intake in trimester 3. Neonatal thigh circumference was negatively associated with frequency of strenuous physical activity, neonatal chest circumference was positively associated with maternal weight and negatively associated with frequency of strenuous physical activity. Neonatal subscapular skinfold thickness was negatively associated with PUFA intake in third trimester, neonatal waist circumference: length ratio was negatively associated with maternal age and positively associated with maternal smoking and maternal mid-upper arm circumference (MUAC) in early pregnancy. The study clearly shows that maternal diet and lifestyle factors were positively associated with the neonate’s body composition. It also shows the significant changes associated with the intake of different foods thereby proving that neonatal central adiposity was positively associated with maternal dietary saturated fat and negatively associated with low GI intervention groups. Healthy Start Study An observational, pre-birth cohort study was done on 1,410 pregnant women aged 16 years and above prior to 24 weeks of gestation after implementing various exclusion criteria. These moms participated in two research visits during pregnancy-the first visit occurred between 8 and 24 weeks of gestation and the second visit occurred between 24 and 32 weeks of gestation while a third visit happened at the hospital after delivery. The newborn baby’s weight, length, head circumference and skin-fold thickness were measured within 72 hours after delivery and the neonatal body composition, fat mass (FM) and fat-free mass (FFM) were calculate from total mass and volume. Maternal pre-pregnancy BMI was calculated using weight measurements and the woman was categorized accordingly and her physical activity levels were measured using a Pregnancy Physical Activity Questionnaire. The diet consumption of the pregnant woman was assessed several times during the study and its quality was assessed using the Healthy Eating Index-2010 that consisted of twelve components giving a maximum score of 100. The study showed a HEI-2010 score between 18 and 89 with a mean of 54.2. Women with a score ≤ 57 were likelier to be obese and have reported of smoking during pregnancy. Lower diet quality was related to younger maternal age, shorter length of gestation and higher energy expenditure. Also, those neonates born to women with this score also had significantly lower birth weight and fat-free mass (FFM) but there was no difference in birth head circumference or birth length between the two groups. Results showed that energy intake as fat and saturated fat was significantly higher in the group with an HEI total score ≤57 but at the same time empty calories were also significantly lower which is a surprising one! Also neonates born to these women had .58% higher fat mass (FM) compared to neonates born to women with a score ≥57. But women with a score ≤57 had no significantly different FFM proving that an increased %FM linked to lower maternal diet quality shows an increase in neonatal FM rather than a decrease in FFM. This large pre-birth cohort showed that lower diet quality had a greater impact on neonatal adiposity, neonates of women with lower diet quality had 24.9 g more fat mass comparatively. Hence, poor maternal diet quality has the ability to increase neonatal adiposity regardless of maternal BMI. Another study on Middle-Eastern women showed that women having a pregestational BMI were at a 2.5 times higher risk of giving birth to low birth weight infants and having a smaller birth height compared to women with a normal BMI while obese women were at a 7.44 times higher risk of giving birth to macrosomic infants compared to women with a normal BMI. References Maternal Low Glycemic Index Diet, Fat Intake and Postprandial Glucose Influences Neonatal Adiposity-Secondary Analysis from the ROLO Study: https://nutritionj.biomedcentral.com/articles/10.1186/1475-2891-13-78 Maternal Diet Quality in Pregnancy & Neonatal Adiposity: The Healthy Start Study: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5356926/ Impact of Maternal Body Mass Index & Gestational Weight Gain on Neonatal Outcomes among Healthy Middle-Eastern Females: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0181255  Relief from Stress with Herbs is Amazing Relief from Stress with Herbs is Amazing It isn’t surprising that something new pops up every time we read about health and wellness in the form of superfoods, fad diets or quick fixes for weight loss, weight gain, muscle buildup and more. Adaptogens are the latest buzzword in the wellness world occupying top place in magazines, health blogs and juice bars. The word adaptogen was first coined by a scientist in 1940 when he defined plant-originated adaptogens that bring health upon the human body. An adaptogen is a phytochemical that stabilizes physiological processes and also encourages homeostasis in the body promoting tolerance to stress. Stress is yet another buzzword in today’s world which spares none and attacks everyone right from school-going kids to elderly adults. There is not a possibility of life without stress but we can dismiss it by handling stress in the right way. Stress is a physiological reaction to environmental pressures that can either be self-induced (such as working hard for perfect results or looking to fulfill life’s goals) or even a result of external pressures such as workload, family demands, monetary crunches or societal pressures. Each of us have the potential to withstand stress and perform well under stress but if the same prolongs there are heavy chances that the same affects our personal life too. Stress is the cause for 50% of all lost working days, the root cause for may illnesses such as depression, anxiety, diabetes as well as neurological problems and the factor behind reduced quality of life for many individuals that the World Health Organization has defined stress to be ‘the health epidemic of the 21st century’. Herbs for Safeguarding Health from Stress There are quite a number of ways proposed for dealing with stress in life including yoga, meditation, exercises, physical activities, hobby classes and more but mankind loves to venture into unexplored territories and come up with new ideas that could benefit humans. Yoga and meditation are tried and tested ways to deal with stress, there are more and more studies coming up on the benefits of physical activity to avoid or displace stress and the latest research is on herbs-a completely new domain that provides ample scope for researchers to try and gain massive information and results. Herbs have been used since thousands of years in Ayurveda and Chinese medicines, occupy prominent roles in culinary domain and are also used as garnishing and fragrance agents. Gardens and terraces are now filled with potted cilantro, basil or thyme plants that bring about an aroma of freshness and herbal gardens are the latest in trend now. Amidst all the behavioral therapies, medications and wellness programs surrounding stress, besides the use of herbs in culinary and medication purposes we now have the latest use of these aromatic agents-as adaptogens. Adaptogens Herbs used in Chinese medication and Ayurveda is not new but the fact that the same herbal plants might help fight against chronic stress has also been proposed in Western medicine for more than 50 years now. I. Brekhman, studied ginseng in 1950 extending the concept of adaptogens as: medicines that are similar to adaptogens but help in maintaining ideal homeostasis under stressful conditions. Later in 1969 new rules were formulated for plant-originated adaptogens stating that they must minimize harms caused by stressful conditions such as fatigue and depression, they must have a positive excitatory effect on the body, these excitatory effects should not cause side effects such as insomnia or excess energy consumption and finally, must not end up harming the human body. The definition for an adaptogen has been changing ever since and in 1998, the Food and Drug Administration of America defined adaptogen as a new kind of metabolic regulator that helps in environmental adaptation and prevents external harm. Adaptogens function mainly by affecting the hypothalamic-pituitary-adrenal (HPA). Yance, an American herbal doctor, proposed that adaptogens should be divided into three categories-primary, secondary and adaptogen companions. Primary adaptogens help in maintaining and restoring homeostasis, produce positive stress response and regulate energy use. Secondary adaptogens do not influence HPA axis directly but influence immune, nervous and endocrine systems. Adaptogen companions have beneficial effects on the HPA axis but do not formally belong to adaptogens unlike the other two types because they only interact with the other two adaptogen categories to improve their effect. Similar to how exercise works on the muscles so do adaptogens work on our adrenal glands. Initially when we exercise it causes stress on our body but as we continue to train and exercise our body becomes better at dealing with the stress and we don’t get as tired as before. Likewise, with adaptogens we are training the body to handle stress and its effects. We have a journal study elaborating on the effects of adaptogens on human health: Adrenal fatigue: Adrenal fatigue occurs when capacity of adrenals to secrete enough hormones to make necessary physiological and biochemical compensations for the stipulated stress levels doesn’t meet the requirements of continuous excess pressure. Stress hormone production increases as eternal pressure increases. Using adaptogens increases effectiveness of adrenal gland secretion reducing excess hormone production. Arthritis: Osteoarthritis and rheumatoid are the common forms of arthritis that are characterized by elevated pain and swelling. Adaptogens are noteworthy solutions for alleviating pain and inflammation. Sleep: Sleep has become a major problem with most people nowadays mainly due to presence of excess stress that affects the normal secretion of cortisol, the stress hormone. Sleep, exercise and diet are integral for sleep. Adaptogens help in producing the right amount of cortisol thereby relieving stress and enabling sleep. Neuroendocrine system: Adaptogens help in stabilizing internal environment of the human body by affecting the neuroendocrine system and also increase rates of oxygen, fats, protein and sugar utilization. Anti-tumor properties: Adaptogens inhibit cancer cell production and stabilization of the functions of human body. They also promote cell repair, prevent growth of tumors and pave way for cell-selective apoptosis. In cancer patients too, adaptogens help in improving their physical condition by modulating biological responses, remodeling immune mechanism and enhancing resistance of the human body. They also promote the production of marrow, increase the amount of blood cells, reduce infection, strengthen lethal effects of chemotherapy and radiation on cancer cells, inhibit tumor metastasis and development of multidrug resistance and also reduce stress hormone levels during immune dysfunction which is linked to tumor growth. Rhodiola rosea Extract (RRE) Roots and rhizome extract of Rhodiola rosea are adaptogens that act to increase the body’s resistance to stress, exhaustion and fatigue. It was long back in 1969 that USSR recommended using RRE for patients suffering from asthenia syndrome, neuroses, vascular dystonia, hypotension and schizophrenia. The affected individual was suggested to take 5-25 drops of the extract in a quarter glass of water thrice daily some 15-30 minutes before meals. Duration of therapy differed based on the individual anywhere between 10 days and 4 months. In another study, 128 patients between 17 and 55 years including both men and women were given RRE as a part of their treatment protocol after being diagnosed with fatigue. Results showed that these patients showed marked improvements in fatigue levels or they disappeared completely. Another open label study on 65 participants suffering from irritability, insomnia and somatic disorders showed improved effect on neuroses. Dispensing therapy with RRE in 177 patients with vascular hypotension showed that the extract helped to stabilize partially or completely 92% patients with hypotension. Another experiment that fed 58 patients suffering from stress-induced depression with 15 drops of extract thrice daily for up to a month or up to four months showed symptomatic improvement. Suffering from weakness or fatigue soon after getting up in the morning or hypersomnia both reduced greatly. There have been no potentially dangerous side effects of RRE observed and it seems to be pretty safe with no complaints of drug-drug interactions or others. Rarely, there have been cases of insomnia, headache, irritability and excitement reported. Tulsi & Ashwagandha There are a couple of studies that show that tulsi (Basil) has therapeutic properties such as adaptogenic, antimicrobial and anti-inflammatory. Basil is holy to Indians, is included as part of meals or even taken as supplements or used for preparing tea. It is said to enhance body’s natural response to deal with physical and emotional stress. But we also do have information against using basil in pregnant and lactating women due to unavailability of authentic data. The herb Ashwagandha gets its name from the odor it emits which is close to the smell of a horse. Its known as Indian Ginseng, Winter Cherry or even the royal herb in Eastern Medicine but there are not many human studies on this most commonly used herb that’s believed to empower the individual with strength and vitality similar to that found in horses, living up to its name! A study on this herb testing its safety and efficiency in reducing stress and anxiety in adults showed marked reduction in their stress and anxiety levels and also revealed no side effects. Other important herbs that do find their place as adaptogens include Eleutherococcus senticosus that’s used to treat chemotherapy-induced bone marrow suppression, angina, insomnia and poor appetite; Lepidium meyenii that’s claimed to increase strength, energy and stamina; Schisandra that’s used to decrease fatigue and stress and improve physical performance and reishi that’s believed to improve immunity. Incorporating Adaptogens in Real-time Cases While positive effects of adaptogens in stress-related changes have been observed in animal experiments there are a handful of drugs that have been adapted as adaptogens in today’s scenario. Though we do have studies and applications showing that plant-originated adaptogens are part of the elite herbal medicine helping mankind overcome stressors the clinical application of these plant-originated adaptogens and their use in healthcare products remains a mystery. We do have studies suggesting what affects our health right from helping us sleep better to stay energetic but we still are in a stage where we cannot 100% convey the message that adaptogens can have a significant impact on the body. But before adding them to our diet or as a supplement it is advisable to talk to the physician about it as one study found that common herbal supplements interact negatively with prescription medications and many times, patients don’t convey the names of all the supplements and pills they take before the doctor prescribes yet another one for their present illness. Still, we are not aware of the long-term effects of adaptogens. Individuals find it easier to pop a pill rather than take precautionary steps to avoid or overcome stress by practicing other stress-relief measures. It is not harmful to sip herbal teas and mix adaptogens with your soups or smoothies but when it comes to supplements ensure that they are safe as many supplement companies add plenty other things that’s been unheard of to improve both your strength and vitality. References A Preliminary Review of Studies on Adaptogens: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6240259/ Effects of Adaptogens on the Central Nervous System : https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3991026/ Stress Management & the Role of Rhodiola Rosea: https://www.tandfonline.com/doi/full/10.1080/13651501.2017.1417442  The Image Aptly Portrays the Food Choices of Teenagers The Image Aptly Portrays the Food Choices of Teenagers Adolescence is an age where every teenager seems to be on a knife-edge and one cannot agree more on this point of view! It’s around puberty that girls and boys experience maximum growth with evident body changes happening in each of them. Besides physical growth, teens also evolve into mature individuals starting to form their own views and ideas. They start making judgements on our way of handling stuffs, comment on people’s appearance (fat or thin, beautiful and ugly and likewise), don’t extend an invitation to our advices and recommendations and feel like they have reached a stage where they are big enough to take decisions on their own. This decision-making idea has proved to be a costly affair in various domains of their life and one of them is certainly food habits. Many teenagers have brought about drastic changes to their lifestyles that include more unhealthy food choices, eating out frequently, absence of activity and late-night snacking all of which increase the adolescent’s nutritional risk over time. Having a teen in your household? I am sure you have been vigorously nodding your head to every sentence that’s written here! Terrible Nutritional Choices Taken During the Vulnerable Stage of Life The period between 10 and 19 years of age is a vulnerable period where health-related behaviors that influence critical chronic degenerative diseases start and the food kids eat during this period are strong factors that determine their present and future health. Unfortunately, with the advent of processed foods and fast food restaurants, the diet quality of adolescents has sharply taken a dip and evidences too support this notion. There has been an increase in intake of energy-dense foods, aerated beverages and salty snacks while the consumption of fruits, veggies and whole grains has decreased paving way for obesity/overweight to be a major public health concern worldwide. Most of the teenager’s dietary choices are due to some distorted perception adopted by them. For instance, a study on adolescent girls found that these kids associated consumption of fast food with pleasure, independence and friends while consumption of healthy food was associated with parents and being at home. Environmental factors including family, friends and society have a strong influence on these children’s ideologies, weight gain and eating habits during their transition from adolescence to adulthood. Nurturing kids with disciplined eating patterns and activity schedules right from younger years is crucial for setting the stage for a healthier adolescence and adulthood. For this, parents should not only emphasize on the need to eat right but also lead the way being a role model for their child. Habits and behaviors form by adolescence and when dietary behaviors are formed these are established through adulthood staying for a lifetime. The prevalence of unhealthy lifestyle patterns hence increases the risk of chronic health diseases such as obesity that impede well-being. United States was the first country to popularize the fast food culture during the 1970s and now has become the largest fast food industry in the world. We have numerous reports on developed countries such as USA, UK and Australia that clearly emphasize the fact that adolescents in these places do not meet the required dietary guidelines as they display overconsumption of energy-dense foods and underconsumption of fruits and vegetables. But we have limited evidence on developing countries such as India and Africa. Still, existing research shows that adolescent’s food consumption varies according to gender and females, in general, display healthier dietary patterns than males. Australian girls consumed more fruits compared to boys while boys drank more carbonated beverages. Likewise, British girls preferred to eat more fruits and vegetables compared to boys while boys chose nutrient-poor foods comparatively. Researchers expect similar dietary habits from adolescents residing in developing countries as well and some of the studies are elaborated here. Food Consumption Pattern in Indian Adolescents A 15-page questionnaire with questions pertaining to meal consumption pattern, vegetarianism, food and beverage intake, snacking practices, home food environment, curriculum, consumerism, school canteen, acquisition of food skills and family characteristics was included in the dietary and lifestyle questionnaire (DALQ). The study included 356 boys and 670 girls who were between 14 and 15 years of age while most others were around 16 years of age. Nine food groups were chosen and with excluding water, among the other eight food groups energy-dense snacks was the commonly consumed food group. The other groups in descending order of food intake include cereals, energy-dense beverages, vegetables, fruits, milk and milk products, non-vegetarian food products and pulses and legumes. Adolescents generally consumed around 10.54 servings of water daily. Results It was observed that a majority of the adolescents did not consume food from all eight food groups, almost two-thirds (59%) did not consume pulses and legumes, more than 50% refrained from eating non-vegetarian items such as fish, meat and chicken, 45% did not eat fruits, 30% did not eat vegetables and 36% did not consume milk and milk products. Visible gender difference in the consumption of these 8 food groups were visible. While girls consumed more of veggies, fruits, cereals and non-vegetarian food products compared to boys it was also seen that male kids consumed more of milk and milk products and energy-dense beverages. Energy-dense snacks, pulses and legumes did not display evident differences in consumption portion between boys and girls. The present study is a clear evidence that more than 75% of adolescents consumed three or more servings of energy-dense snacks and 50% of participants consumed 3 or more servings of energy-dense beverages. While this study happened in Kolkata, another study in New Delhi showed that more than a quarter (32%) of secondary school kids consumed fast foods such as pizzas, burgers and fried foods three and more times every week. Despite being the largest producer of milk, the study showed that almost two-fifth of participants did not consume recommended dairy servings that nourish the body with energy, protein and micronutrients. Also, girls in the study ate healthier than boys reflecting the worldwide ideology that females ate healthier than males. This could be attributed to the weight-consciousness of the female population and also to the male population which often feels that eating greens, surviving on salads and healthy food was not a display of masculinity. A global survey on adolescents residing in Southeast Asian countries such as India, Indonesia, Myanmar, Thailand and Sri Lanka suggested that nearly 28% of participants reported consuming fruits less than once daily. Indian adolescents display unhealthy dietary patterns and until this trend changes we cannot expect to see remarkable changes in obesity/overweight rates in the Indian population. Food Patters of Saudi Arabian Adolescents A cross-sectional study was conducted on girls aged between 13 and 29 years and their body measurements were taken at the start of the study. Of the 196 participants involved in the study, 64.8% of them were adolescents aged between 13 and 18 years while the rest were adults. Results showed that more than 95% of them ate fast food at restaurants with 52.8% adolescent girls and 60.9% young adult girls consuming fast food once per week. 25.2% adolescent girls and 20.3% young adult girls consumed fast food twice or more per week. Common fast foods included beef or chicken burgers (70.4%), pizzas (32.7%) and French fries (29.6%). Most of the participants chose small or medium portion sizes and it was only 17.9% participants who went for large portion sizes. 89% adolescents and 75% adult girls consumed carbonated soft drinks along with their fast food meal while consumption of coffee, tea, sweetened fruit drinks and energy drinks were a rare combination with fast food. While adolescents mostly consumed fast food for taste, adult females consumed it for the sake of convenience. It was a surprising to find that a majority of these girls did not know the nutritional value of these fast foods or were totally ignorant of the concept of nutrition value. Cohort Study on Malaysian Adolescents The study on Malaysian students included 1361 adolescent girls and boys aged around 13 years. A 7-day dietary intake history regarding information on food and drink consumption at breakfast, mid-morning snack, lunch, tea, dinner and supper were noted by reputed dietitians. Height, weight and body mass index measurements were calculated at the start of the study. Among the total number of participants involved in the study 1290 of them completed a dietary interview. Of the lot, almost 65% were females. Study results showed that male adolescents consumed more energy (carbs, protein, fats and saturated fats), macronutrients and sugars compared to females. Females consumed more of vitamin D compared to their male counterparts but had inadequate consumption of iron. Both males and females had decreased intake of energy, vitamin D and calcium but showed optimal intake of proteins and fats. All these studies are a clear indication that adolescents anywhere around the world are not consuming a well-balanced meal that’s rich in nutrients. Most of the teenagers are inclined towards processed foods consumption quoting different reasons which also exists as the cause behind the obesity epidemic. Parents, teachers and the society must come together in helping children change their attitude towards food, help them choose more of vegetables, fruits and pulses to eat daily and make them realize the importance of a healthy diet in one’s life. References Food Consumption Patterns of Adolescents Aged 14-16 Years in Kolkata: https://nutritionj.biomedcentral.com/articles/10.1186/s12937-017-0272-3 Trends of Fast Food Consumption Among Adolescent & Young Adult Saudi Girls Living in Riyadh: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4366480/ Dietary Intake Among Adolescents in a Middle-income Country: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0155447 My kid loves to attend birthday parties and this is no surprise but being an introvert who doesn’t even open her mouth to ask for a glass of water to the host the fact that she runs to these get-togethers is amazing indeed. But this happiness of mine was short-lived once I realized that she loved eating the creamy cakes, greasy fries and drinking chilled soft-drinks (all of which are almost never present in my house) with no intention of even wishing the birthday kid! She is not an exception and there are many other kids with a similar state of mind living in this world amongst whom many of them are bad victims of obesity.
Obesity exists as a public health epidemic affecting both children and adults alike. Abdominal obesity has affected innumerable number of people as reducing tummy fat has become almost next-to-impossible for individuals. Fat is not our enemy and it is a macronutrient that’s very much needed by our body for proper functioning but we do have good and bad fat whose imbalance creates havoc in each of those whose dietary intake is not well-balanced. Such abdominal obesity is a major risk factor for metabolic diseases such as type 2 diabetes (T2DM), cardiovascular diseases (CVD) and non-alcoholic fatty liver disease (NAFLD). Fat accumulation can be visceral and subcutaneous and any type of fat accumulation is dangerous. But visceral fat causes more harm as it is the fat lining internal body organs. The higher risk for CVD and other diseases due to abdominal obesity is due to the accumulation of fat in non-adipose tissue. Such visceral adipose tissue (VAT) and hepatic triglyceride content (HTGC) are linked to metabolic risk factors including insulin resistance, coronary artery disease and cardiovascular disease. VAT releases free fatty acids (FFA) and cytokine secretion which together with insulin resistance result in fat accumulation in the liver and higher risk of T2DM and CVD. So, this makes both liver and visceral fats the main fat regions that need immediate intervention to prevent cardiometabolic disease in the form of physical activity and dietary changes. Studies show that dietary fibre, calcium and phytochemicals were inversely related to visceral fat deposits; following a healthy dietary intake and intake of medium-chain triacylglycerols show an inverse association with visceral fat and subcutaneous fat and studies show that increased energy intake during childhood years increases the risk of non-alcoholic fatty liver disease (NAFLD) irrespective of macronutrient intake. All these studies and other related ones focus on one single nutrient and its impact but it would be better to study the effects of food groups and foods together as foods might have multiple nutrients acting and interacting with each other brining in various effects. Though we know that fruits, vegetables and whole grains have a positive impact in reducing the risk of diseases and aid in weight maintenance/loss we don’t have much knowledge about the relationship between food groups and ectopic fat deposit. A group of researchers tried to understand the relationship between dietary intake of food groups and visceral and liver fat content in a population-based cohort. Netherlands Epidemiology of Obesity (NEO) Study The NEO is a prospective cohort study of 6671 individuals aged between 45 and 65 years with a self-reported BMI≥27 eligible for participation. All of them filled a questionnaire about demographic and clinical information and the next day visited the NEO study centre after an overnight fast. The study assessing relationship between food groups and fat content is a cross-sectional analysis of the baseline measurement of participants (who were chosen after imposing all exclusion criteria) with a measurement of VAT. Ethnicity was self-reported, tobacco smoking was categorized as current, former or never smoking; education level was self-reported; BMI calculation were made; menopause state was mentioned; basal metabolic rate was calculated based on age, sex, height and weight and participant’s frequency and duration of physical activity during leisure time was measured. A self-administered food frequency questionnaire (FFQ) helped the participants answer questions on the frequency (times per day, times per week, times per month or never) of food intakes during the past month. Serving size was estimated for calculating calories in terms of pieces of fruits, spoons of potatoes, etc. Nutrient intake and total energy were calculated using the Dutch Food Composition Table. Depending on nutrients, sources and biological effects foods were categorized into different food groups with the help of the FFQ. This included classifying them under dairy (milk, cheese, yogurt and butter), fruits and veggies, meat, sweet snacks (candy and cake), fish and plant-based fats and oils (margarine and oils). Calorie value of each food group was divided by the total calorie intake per day to find the total energy percentage. VAT and HTGC were measured in appropriate ways. Of the 6671 who were interested in the study only 2304 were included in the analysis due to various exclusion criteria including diabetes, elevated energy intake, incomplete FFQ, energy-restricted diet intake and unavailable data on smoking. The research team assessed the reproducibility of the dietary intakes of the food groups in 100 participants who completed the FFQ twice with only a 3-month gap between them. It was seen that after adjusting different factors dietary intake of fruits and vegetables was linked to 1.12 cm2 less VAT; intake of plant-based fats and oils was linked to 13.9 cm2 less VAT and dietary intake of fish, dairy, meat and sweet snacks was not linked with VAT. Introspecting on the food groups minutely showed that yogurt created a negative association between dairy and VAT in women whereas dietary intake of dairy, meat and fruits and vegetables was more strongly linked to VAT in postmenopausal women than in premenopausal women. Of 1715 participants with HTGC measurements dietary intake of sweet snacks was associated with a 1.19-fold higher HTGC while intake of fruits, dairy, vegetables, fish, meat and fats and oils were not linked to HTGC. Finetuning showed that vegetables were strongly associated with HTGC than fruits, and yogurt was linked with liver fat of all the dairy components. Sweet snacks and HTGC was linked strongly in premenopausal women than in postmenopausal women. The study shows that fish and meat are not associated with visceral fat, dairy was negatively associated with visceral fat and sweet snacks intake is linked to more visceral fat. Effect of Macronutrients on Liver Fat Content Hypercaloric Diet Most of the studies involve a hypercaloric diet where most of the participants are males with a BMI<27 who were overfed a fructose diet. Such consumption leads to increased fatty deposits in the liver. Men almost consumed >180 g/d of fructose compared to the recommended 30-50 g/d. fructose consumption is generally higher in the adolescent population. When studies tried to overfeed calories while reducing the quantity of fructose consumed there was no increase in fatty liver content even after 28 days. Fructose and glucose have similar effect on liver fat accumulation. We don’t consume fructose as an individual product but it is a by-product of fruits and of those containing free sugars (sugar-sweetened beverages or confectionaries). A study by Maersk et al compared the effects of ingesting 1L/d of a sugar-sweetened beverage, calorie-matched milk, non-nutritive beverage or water for 6 months. It was seen that consuming a sugar-sweetened beverage increased liver fat by 132-149% compared to other beverage groups but it must be noticed that as the different groups were having gender disparity and diets too were not standardized between the groups. Sevastianova et al. researched on a 3-week hypercaloric diet where 98% of excess calories was given in the form of added sugars such as candy, fruit juice and sugar-sweetened beverages. There was almost 27% increase in liver fat at the end of the high-sugar diet. A couple of studies showed that alongside increased total fat intake the fatty acid composition of a high-energy diet might also be an important regulator of lover fat accumulation. Bortolotti et al. showed that while increased fat intake elevated liver fat by 90% supplementing it with protein led to a reduction in liver fat accumulation compared to a high-fat diet. A protein-rich diet helped in moderating liver fat accumulation to a great extent. Excess consumption of fat and sugar led to increased fatty deposits in the liver. Hypocaloric Diet Various studies show that significant reduction in total calorie intake was linked to a significant reduction in liver fat content. This shows that weight loss interventions are standard or helpful strategies against NAFLD. A study by Browning et al. showed that reducing carbohydrate intake helped in reducing liver fat content than reducing total calories without changes to the macronutrient composition of the diet but some studies show that carbohydrate intake has little influence on change in liver fat content. But a large number of studies showed that total calorie deficits is the need of the hour for decreasing liver fat and alterations in macronutrient composition have little influence. Isocaloric Diet The difference in nutrient intake modulates liver fat content. Altering macronutrient composition to a higher fat intake leads to increase in liver fat content. This is applicable only to increase in SFA levels and increasing MUFA and PUFA levels reduce liver fat content. Consumption of a hypercaloric diet increases liver fat content, consumption of a hypocaloric diet decreases liver fat content and consumption of dietary sugars requires further clarity as the effect depends on the form in which they are consumed. Bottomline It has been proposed that obese/overweight children with fatty liver disease reduce fatty deposits in the liver by refraining from drinking soft drinks and fruit juices and cutting down consumption of sugary foods. Physicians advise patients with a fatty liver disease to cut down on excess sugar intake that’s generally high in processed foods and exercise regularly. Its tempting when you look at the glossy supermarket aisles stuffed with your favourite candies and treats. It is always advisable to stay away from the middle aisles that contain these stuffs. Avoid storing junk foods at home as these once again disturb the individual provoking him/her to eat them when its right before the eye. Staying on a healthy diet, avoiding excess consumption of processed foods and exercising regularly keeps you away from weight gain and fatty deposits anywhere in the body, especially the liver. References Sweet Snacks are Positively & Fruits & Vegetables are Negatively Associated with Visceral or Lover Fat Content in Middle-Aged Men & Women: https://academic.oup.com/jn/article/149/2/304/5290057 Influence of Dietary Macronutrients on Liver Fat Accumulation & Metabolism: https://jim.bmj.com/content/65/8/1102 To Avoid Fatty Liver, Avoid Sugary Foods & Drinks: https://www.nytimes.com/2019/01/22/well/eat/to-fight-fatty-liver-avoid-sugary-foods-and-drinks.html |
AVOID FRAUD. EAT SMART+91 7846 800 800
|
- Home
- Written Testimonials
- Consult
- Clinics
- Blogs
-
Diet & Nutrition
- Diabetes Reversal
- IVF IUI not needed for PCOS PCOD Infertility
-
Medical Nutrition
>
-
Disease & Conditions
>
- Infertility | PCOS
- Diabetes Mellitus
- Cholesterol
- Hypothyroid
- Kidney Problems
- Hypertension
- Cardiovascular Diseases
- Liver Diseases
- Gastro intestinal disorder
- Cancer
- Metabolic Disorders
- Orthopedic Disorders
- Eating Disorders
- Dietary Recall
- Weight Record Filled By Clients
- Online Payment Transaction Details
- Online Clients Weight Check Form
- Our Program Package Service Charges
- Weight Record 2017 Clients
- Measurements sent by Clients
- Terms & Conditions Of Payment
- Thanks. Your Form is Submitted
- Video Testimonials
- Lifestyle & Wellness
- Lifestyle & Wellness Blog
- Allergy & Intolerance
- Weight Loss / Gain
- Weight Loss / Slimming Blog
-
Disease & Conditions
>
- Life Cycle Nutrition >
- Sports Nutrition >
- Integrity in Nutrition
- Knowledge Centre
© COPYRIGHT 2022. ALL RIGHTS RESERVED. FRST HEALTHCARE PVT LTD.
Dr. Nafeesa Imteyaz of First Eat Right clinic, is the Best Dietitian Nutritionist in Bangalore. Best Dietitian Nutritionist in Pune. Best Dietitian Nutritionist in Hyderabad. Best Dietitian Nutritionist in Chennai. Best Dietitian Nutritionist in Mumbai. Best Dietitian Nutritionist in Delhi. Best Dietitian Nutritionist in Kolkata.