|
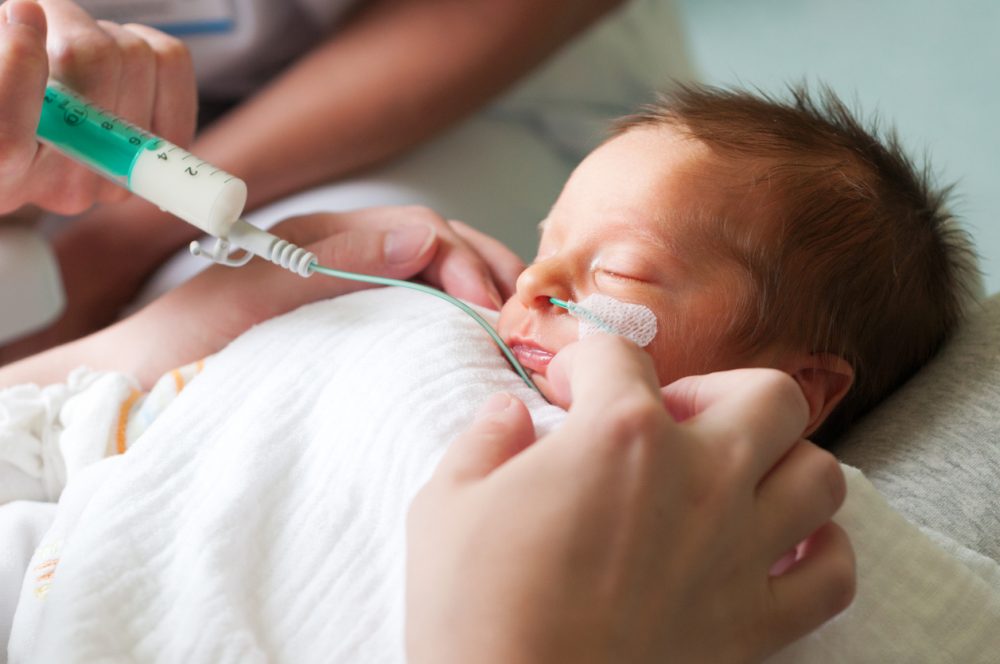
Every mother-to-be is given an estimated due date for her fetus but rarely more than 5% of infants are born on this date. As the name suggests, the specified date is only an ‘estimated’ date and not the exact date on which the child is due anyway. Every parent wishes for a full-term (happens after 37th week of pregnancy) delivery but deviations do happen frequently and some children are born before the start of the 37th week of pregnancy. The baby can be born as early as the 25th week of pregnancy and we call such babies as ‘extremely preterm’ infants. Any preterm baby is subjected to complications and the intensity of the complication depends on how early a baby is born.
Of the various complications, unmet nutritional requirements exist as one of the concerns for every person attending to a preterm infant. This is a challenge as establishing adequate intake is extremely painful to achieve in the initial few weeks after delivery. The recommended dietary intakes are based on needs for maintenance and growth alongside the assumption that post-natal growth approximates that in utero at the same post conceptional age. Even if these recommended nutrition levels are established in such infants there are frequent clinical interventions during the first 3-4 weeks after delivery that cause much hindrance to fulfill these requirements. Again, recommendations for weight gain include that it approximates that of the normal fetus at the same post conception age (10-15 g/kg/day). But this is practically not easy to achieve as preterm infants lose weight before regaining birth weight and there is the chance of a lag in expected weight at the same postconceptional age in these infants. If any infant wishes to break this and gain normal weight the weight gain must be in excess of what would happen in utero and this is next to impossible during the first few days/weeks of hospital stay. Many of the preterm infants have reduced organ development and the foremost goal of enteral feed is to support postnatal intestinal adaptation. We have research data supporting the fact that such children adapt better to human milk compared to low birthweight infant formula. If the infant doesn’t adapt well to human milk term infant formula might be fed until he/she adapts well and from thereon, preterm infant formula might be given. While it is of great importance that infants adopt well to enteral feeding once the tolerance is sustained it is then crucial to ensure that intake meets growth needs. Supplementing Nutritional Requirements Though breast milk is the recommended form of enteral nutrition for all infants including preterm babies sadly we do also understand this this alone is not sufficient to meet recommended nutritional needs for growth in preterm infants. Preterm infants feeding on human milk gain less weight than those feeding on fortified human milk. Also, those preterm infants feeding on human milk alone show poorer growth compared to those infants feeding on preterm infant formula because of lower concentration of proteins, minerals and energy density in human milk comparatively. It is better to provide these newborns with fortified human milk, preterm infant formula or a combination of both. It is easier said than done and fortification of human milk poses a significant challenge and there have been several steps taken to minimize this challenge. Among these steps, adjustable fortification (ADJ) seems to display favorable results-this includes using a protein supplement on an individualized basis alongside a multi-component fortifier. This basically involves providing the newborn with protein based on his/her metabolic response but this remains a challenge as the availability of a high-quality, well-tolerated protein supplement is almost non-existent. Doctors don’t recommend cow’s milk until a child’s first birthday owing to various reasons that include a risk of allergies and chances of intestinal inflammation in preterm neonates but most of the multi-nutrient fortifiers are derived from bovine milk that has a protein composition that’s different from human milk. Such disadvantages led researchers to check out on exclusive HM diets (human milk-based fortifier and donor HM when mother’s milk is unavailable) and one such research led them to donkey milk. These researchers were surprised to find that when children allergic to cow milk were fed with donkey milk (DM) it was well-tolerated by these kids as the protein and lipid structure of DM was similar to human milk composition. According to the research group, feeding preterm children with human milk fortified by protein and multi-component supplements derived from DM is more suitable than any other fortification for their short- and long-term well-being. The study selected infants that were born before 32 weeks of pregnancy, <1500 g at birth, fed with exclusive breast milk (mother’s own or donor milk) and did not suffer from certain medical conditions laid down. Once selected, the kids were divided into two groups-the control group and the fortilat group. The kids in the control group were fed with multi-component fortifier and protein concentrate named BMC and BPC respectively derived from bovine milk for a minimum period of 21 days. The fortilat group were provided with multi-component fortifier and protein concentrate namely DMC and DPC derived from donkey milk for a period of 21 days. The study included 115 infants who were born before 32 weeks of gestation weighing less than 1500 grams with breastfeeding initiation rates present in 90% of kids. The researchers found that the DM had an n-3 PUFA (poly unsaturated fatty acids) structure that was similar to the one found in humans and was also rich in lysosome, a protein that has antibacterial property, that can hamper pathogen growth and milk spoilage. Supplementing infants with DM decreases body lipid concentration and affects glucose and lipid metabolism in ways similar to human milk than cow’s milk. The researchers hypothesized from the study that feeding newborns with human milk fortified by protein and multi-component supplements derived from DM will improve feeding tolerance and clinical, metabolic, neurological and auxological outcomes. But we do need further evidence to confirm the usage of DM as a fortifier for human milk. This would indeed open the door for a sea of opportunities as it minimizes the risk of neurocognitive impairment and poor health outcomes such as retinopathy and bronchopulmonary dysplasia. It is mandatory that human milk is supplemented with nutrients such as protein, calcium and phosphate to meet the nutrient requirements of babies. References Nutritional Adequacy of a Novel Human Milk Fortifier from Donkey Milk in Feeding Preterm Infants: https://nutritionj.biomedcentral.com/articles/10.1186/s12937-017-0308-8 Feeding Issues in Preterm Infants: https://fn.bmj.com/content/fetalneonatal/83/3/F215.full.pdf Fortification in Human Milk for Preterm Infants: https://www.frontiersin.org/articles/10.3389/fped.2019.00076/full Comments are closed.
|
AVOID FRAUD. EAT SMART+91 7846 800 800
|
- Home
- Written Testimonials
- Consult
- Clinics
- Blogs
-
Diet & Nutrition
- Diabetes Reversal
- IVF IUI not needed for PCOS PCOD Infertility
-
Medical Nutrition
>
-
Disease & Conditions
>
- Infertility | PCOS
- Diabetes Mellitus
- Cholesterol
- Hypothyroid
- Kidney Problems
- Hypertension
- Cardiovascular Diseases
- Liver Diseases
- Gastro intestinal disorder
- Cancer
- Metabolic Disorders
- Orthopedic Disorders
- Eating Disorders
- Dietary Recall
- Weight Record Filled By Clients
- Online Payment Transaction Details
- Online Clients Weight Check Form
- Our Program Package Service Charges
- Weight Record 2017 Clients
- Measurements sent by Clients
- Terms & Conditions Of Payment
- Thanks. Your Form is Submitted
- Video Testimonials
- Lifestyle & Wellness
- Lifestyle & Wellness Blog
- Allergy & Intolerance
- Weight Loss / Gain
- Weight Loss / Slimming Blog
-
Disease & Conditions
>
- Life Cycle Nutrition >
- Sports Nutrition >
- Integrity in Nutrition
- Knowledge Centre
© COPYRIGHT 2022. ALL RIGHTS RESERVED. FRST HEALTHCARE PVT LTD.
Dr. Nafeesa Imteyaz of First Eat Right clinic, is the Best Dietitian Nutritionist in Bangalore. Best Dietitian Nutritionist in Pune. Best Dietitian Nutritionist in Hyderabad. Best Dietitian Nutritionist in Chennai. Best Dietitian Nutritionist in Mumbai. Best Dietitian Nutritionist in Delhi. Best Dietitian Nutritionist in Kolkata.